Intraoperative Molecular Imaging Combined With Positron Emission Tomography Improves Surgical Management of Peripheral Malignant Pulmonary Nodules
- PMID: 28746152
- PMCID: PMC11073793
- DOI: 10.1097/SLA.0000000000002382
Intraoperative Molecular Imaging Combined With Positron Emission Tomography Improves Surgical Management of Peripheral Malignant Pulmonary Nodules
Abstract
Objective: To determine if intraoperative molecular imaging (IMI) can improve detection of malignant pulmonary nodules.
Background: 18-Fluorodeoxyglucose positron emission tomography (PET) is commonly utilized in preoperative assessment of patients with solid malignancies; however, false negatives and false positives remain major limitations. Using patients with pulmonary nodules as a study model, we hypothesized that IMI with a folate receptor targeted near-infrared contrast agent (OTL38) can improve malignant pulmonary nodule identification when combined with PET.
Methods: Fifty patients with pulmonary nodules with imaging features suspicious for malignancy underwent preoperative PET. Patients then received OTL38 before pulmonary resection. During resection, IMI was utilized to evaluate known pulmonary nodules and identify synchronous lesions. Tumor size, PET standardized uptake value, and IMI tumor-to-background ratios were compared for known and synchronous nodules via paired and unpaired t tests, when appropriate. Test characteristics of PET and IMI with OTL38 were compared.
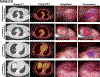
Results: IMI identified 56 of 59 (94.9%) malignant pulmonary nodules identified by preoperative imaging. IMI located an additional 9 malignant lesions not identified preoperatively. Nodules only detected by IMI were smaller than nodules detected preoperatively (0.5 vs 2.4 cm; P < 0.01), but displayed similar fluorescence (tumor-to-background ratio 3.3 and 3.1; P = 0.50). Sensitivity of IMI and PET were 95.6% and 73.5% (P = 0.001), respectively; and positive predictive values were 94.2% and 89.3%, respectively (P > 0.05). Additionally, utilization of IMI clinically upstaged 6 (12%) subjects and improved management of 15 (30%) subjects.
Conclusions: These data suggest that combining IMI with PET may provide superior oncologic outcomes for patients with resectable lung cancer.
Conflict of interest statement
Figures
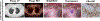

References
-
- Ost D. and Fein A, Evaluation and management of the solitary pulmonary nodule. Am J Respir Crit Care Med, 2000. 162(3 Pt 1): p. 782–7. - PubMed
-
- Henschke CI, et al., Early Lung Cancer Action Project: overall design and findings from baseline screening. Lancet, 1999. 354(9173): p. 99–105. - PubMed
-
- Wahidi MM, et al., Evidence for the treatment of patients with pulmonary nodules: when is it lung cancer?: ACCP evidence-based clinical practice guidelines (2nd edition). Chest, 2007. 132(3 Suppl): p. 94S–107S. - PubMed
-
- Gould MK, et al., Accuracy of positron emission tomography for diagnosis of pulmonary nodules and mass lesions: a meta-analysis. JAMA, 2001. 285(7): p. 914–24. - PubMed
-
- Kernstine KH, Grannis FW Jr., and Rotter AJ, Is there a role for PET in the evaluation of subcentimeter pulmonary nodules? Semin Thorac Cardiovasc Surg, 2005. 17(2): p. 110–4. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

