Role of radiotherapy fractionation in head and neck cancers (MARCH): an updated meta-analysis
- PMID: 28757375
- PMCID: PMC5737765
- DOI: 10.1016/S1470-2045(17)30458-8
Role of radiotherapy fractionation in head and neck cancers (MARCH): an updated meta-analysis
Erratum in
-
Correction to Lancet Oncol 2017; 18: 1221-37.Lancet Oncol. 2018 Apr;19(4):e184. doi: 10.1016/S1470-2045(18)30211-0. Lancet Oncol. 2018. PMID: 29611524 No abstract available.
Abstract
Background: The Meta-Analysis of Radiotherapy in squamous cell Carcinomas of Head and neck (MARCH) showed that altered fractionation radiotherapy is associated with improved overall and progression-free survival compared with conventional radiotherapy, with hyperfractionated radiotherapy showing the greatest benefit. This update aims to confirm and explain the superiority of hyperfractionated radiotherapy over other altered fractionation radiotherapy regimens and to assess the benefit of altered fractionation within the context of concomitant chemotherapy with the inclusion of new trials.
Methods: For this updated meta-analysis, we searched bibliography databases, trials registries, and meeting proceedings for published or unpublished randomised trials done between Jan 1, 2009, and July 15, 2015, comparing primary or postoperative conventional fractionation radiotherapy versus altered fractionation radiotherapy (comparison 1) or conventional fractionation radiotherapy plus concomitant chemotherapy versus altered fractionation radiotherapy alone (comparison 2). Eligible trials had to start randomisation on or after Jan 1, 1970, and completed accrual before Dec 31, 2010; had to have been randomised in a way that precluded prior knowledge of treatment assignment; and had to include patients with non-metastatic squamous cell carcinoma of the oral cavity, oropharynx, hypopharynx, or larynx undergoing first-line curative treatment. Trials including a non-conventional radiotherapy control group, investigating hypofractionated radiotherapy, or including mostly nasopharyngeal carcinomas were excluded. Trials were grouped in three types of altered fractionation: hyperfractionated, moderately accelerated, and very accelerated. Individual patient data were collected and combined with a fixed-effects model based on the intention-to-treat principle. The primary endpoint was overall survival.
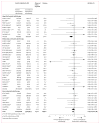
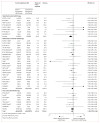
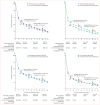
Findings: Comparison 1 (conventional fractionation radiotherapy vs altered fractionation radiotherapy) included 33 trials and 11 423 patients. Altered fractionation radiotherapy was associated with a significant benefit on overall survival (hazard ratio [HR] 0·94, 95% CI 0·90-0·98; p=0·0033), with an absolute difference at 5 years of 3·1% (95% CI 1·3-4·9) and at 10 years of 1·2% (-0·8 to 3·2). We found a significant interaction (p=0·051) between type of fractionation and treatment effect, the overall survival benefit being restricted to the hyperfractionated group (HR 0·83, 0·74-0·92), with absolute differences at 5 years of 8·1% (3·4 to 12·8) and at 10 years of 3·9% (-0·6 to 8·4). Comparison 2 (conventional fractionation radiotherapy plus concomitant chemotherapy versus altered fractionation radiotherapy alone) included five trials and 986 patients. Overall survival was significantly worse with altered fractionation radiotherapy compared with concomitant chemoradiotherapy (HR 1·22, 1·05-1·42; p=0·0098), with absolute differences at 5 years of -5·8% (-11·9 to 0·3) and at 10 years of -5·1% (-13·0 to 2·8).
Interpretation: This update confirms, with more patients and a longer follow-up than the first version of MARCH, that hyperfractionated radiotherapy is, along with concomitant chemoradiotherapy, a standard of care for the treatment of locally advanced head and neck squamous cell cancers. The comparison between hyperfractionated radiotherapy and concomitant chemoradiotherapy remains to be specifically tested.
Funding: Institut National du Cancer; and Ligue Nationale Contre le Cancer.
Copyright © 2017 Elsevier Ltd. All rights reserved.
Conflict of interest statement
AA, BL, J-PP, and PB report grants from Ligue National Contre le Cancer and Institut National du Cancer during the conduct of the study. All other authors declare no competing interests.
Figures


Comment in
-
The true value of altered fractionation in head and neck cancer.Lancet Oncol. 2017 Sep;18(9):1147-1148. doi: 10.1016/S1470-2045(17)30568-5. Epub 2017 Jul 27. Lancet Oncol. 2017. PMID: 28757378 No abstract available.
References
-
- Bourhis J, Overgaard J, Audry H, et al. Hyperfractionated or accelerated radiotherapy in head and neck cancer: a meta-analysis. Lancet. 2006;368:843–54. - PubMed
-
- Overgaard J, Hansen HS, Specht L, et al. Five compared with six fractions per week of conventional radiotherapy of squamous-cell carcinoma of head and neck: DAHANCA 6 and 7 randomised controlled trial. Lancet. 2003;362:933–40. - PubMed
-
- Saunders MI, Rojas AM, Parmar MKB, Dische S CHART Trial Collaborators. Mature results of a randomized trial of accelerated hyperfractionated versus conventional radiotherapy in head-and-neck cancer. Int J Radiat Oncol Biol Phys. 2010;77:3–8. - PubMed
-
- Pignon J-P, le Maitre A, Maillard E, Bourhis J. Meta-analysis of chemotherapy in head and neck cancer (MACH-NC): an update on 93 randomised trials and 17,346 patients. Radiother Oncol. 2009;92:4–14. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

