Autoreactive T cells in type 1 diabetes
- PMID: 28762987
- PMCID: PMC5531393
- DOI: 10.1172/JCI94549
Autoreactive T cells in type 1 diabetes
Abstract
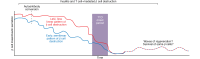
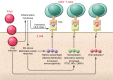
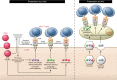
Type 1 diabetes (T1D) is a chronic autoimmune disease that causes severe loss of pancreatic β cells. Autoreactive T cells are key mediators of β cell destruction. Studies of organ donors with T1D that have examined T cells in pancreas, the diabetogenic insulitis lesion, and lymphoid tissues have revealed a broad repertoire of target antigens and T cell receptor (TCR) usage, with initial evidence of public TCR sequences that are shared by individuals with T1D. Neoepitopes derived from post-translational modifications of native antigens are emerging as novel targets that are more likely to evade self-tolerance. Further studies will determine whether T cell responses to neoepitopes are major disease drivers that could impact prediction, prevention, and therapy. This Review provides an overview of recent progress in our knowledge of autoreactive T cells that has emerged from experimental and clinical research as well as pathology investigations.
Conflict of interest statement
Figures
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

