Identification of factors associated with stillbirth in the Indian state of Bihar using verbal autopsy: A population-based study
- PMID: 28763449
- PMCID: PMC5538635
- DOI: 10.1371/journal.pmed.1002363
Identification of factors associated with stillbirth in the Indian state of Bihar using verbal autopsy: A population-based study
Abstract
Background: India was estimated to have the largest numbers of stillbirths globally in 2015, and the Indian government has adopted a target of <10 stillbirths per 1,000 births by 2030 through the India Newborn Action Plan (INAP). The objective of this study was to use verbal autopsy interviews to examine factors associated with stillbirth in the Indian state of Bihar and make recommendations for the INAP to better inform the setting of priorities and actions to reduce stillbirths.
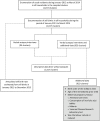
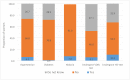
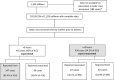
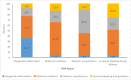
Methods and findings: Verbal autopsy interviews were conducted for deaths including stillbirths that occurred from January 2011 to March 2014 in a sample of 109,689 households (87.1% participation) in 1,017 clusters representative of the state of Bihar. The Population Health Metrics Research Consortium shortened verbal autopsy questionnaire was used for each interview, and cause of death was assigned using the SmartVA automated algorithm. A stillbirth was defined as a foetal death with a gestation period of ≥28 weeks wherein the foetus did not show any sign of life. We report on the stillbirth epidemiology and present case studies from the qualitative data on the health provider interface that can be used to improve success of improved, skilled care at birth and delivery interventions. The annualised stillbirth incidence was 21.2 (95% CI 19.7 to 22.6) per 1,000 births, with it being higher in the rural areas. A total of 1,132 stillbirths were identified; 686 (62.2%) were boys, 327 (29.7%) were firstborn, and 760 (68.9%) were delivered at a health facility. Of all the stillbirths, 54.5% were estimated to be antepartum. Only 6,161 (55.9%) of the women reported at least 1 antenatal care visit, and 33% of the women reported not consuming the iron folic acid tablets during pregnancy. Significant differences were seen in delivery-related variables and associated maternal conditions based on the place of delivery and type of stillbirth. Only 6.1% of the women reported having undergone a test to rule out syphilis. For 34.2% of the stillbirths, the possible risk factor for stillbirth was unexplained. For the remaining 65.8% of the women who reported at least 1 complication during the last 3 months of pregnancy, maternal conditions including anaemia, fever during labour, and hypertension accounted for most of the complications. Of importance to note is that the maternal conditions overlapped quite significantly with the other possible underlying risk factors for stillbirth. Obstetrics complications and excessive bleeding during delivery contributed to nearly 30% of the cases as a possible risk factor for stillbirth, highlighting the need for better skilled care during delivery. Of the 5 major themes identified in open narratives, 3 were related to healthcare providers-lack of timely attention, poor skills (knowledge or implementation), and reluctance to deliver a dead baby. The case studies document the circumstances that highlight breakdowns in clinical care around the delivery or missed opportunities that can be used for improving the provision of quality skilled care. The main limitation of these data is that stillbirth is defined based on the gestation period and not based on birth weight; however, this is done in several studies from developing country settings in which birthweight is either not available or accurate.
Conclusions: To our knowledge, this study is among the few large, population-based assessments of stillbirths using verbal autopsy at the state level in India. These findings provide detailed insight into investigating the possible risk factors for stillbirths, as well as insight into the ground-level changes that are needed within the health system to design and implement effective preventive and intervention policies to reduce the burden of stillbirths. As most of the stillbirths are preventable with high-quality, evidence-based interventions delivered before and during pregnancy and during labour and childbirth, it is imperative that with INAP in place, India aspires to document stillbirths in a systematic and standardised manner to bridge the knowledge gap for appropriate actions to reduce stillbirths. We have made several recommendations based on our study that could further strengthen the INAP approach to improve the quality and quantity of stillbirth data to avoid this needless loss of lives.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
References
-
- Lawn JE, Blencowe H, Waiswa P, Amouzou A, Mathers C, Hogan D, et al. Stillbirths: rates, risk factors, and acceleration towards 2030. Lancet (London, England). 2016;387(10018):587–603. Epub 2016/01/23. doi: 10.1016/s0140-6736(15)00837-5 . - DOI - PubMed
-
- Bhutta ZA, Yakoob MY, Lawn JE, Rizvi A, Friberg IK, Weissman E, et al. Stillbirths: what difference can we make and at what cost? Lancet (London, England). 2011;377(9776):1523–38. Epub 2011/04/19. doi: 10.1016/s0140-6736(10)62269-6 . - DOI - PubMed
-
- Lawn JE, Blencowe H, Pattinson R, Cousens S, Kumar R, Ibiebele I, et al. Stillbirths: Where? When? Why? How to make the data count? Lancet (London, England). 2011;377(9775):1448–63. Epub 2011/04/19. doi: 10.1016/s0140-6736(10)62187-3 . - DOI - PubMed
-
- Pattinson R, Kerber K, Buchmann E, Friberg IK, Belizan M, Lansky S, et al. Stillbirths: how can health systems deliver for mothers and babies? Lancet (London, England). 2011;377(9777):1610–23. Epub 2011/04/19. doi: 10.1016/s0140-6736(10)62306-9 . - DOI - PubMed
-
- Goldenberg RL, McClure EM, Bhutta ZA, Belizan JM, Reddy UM, Rubens CE, et al. Stillbirths: the vision for 2020. Lancet (London, England). 2011;377(9779):1798–805. Epub 2011/04/19. doi: 10.1016/s0140-6736(10)62235-0 . - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

