Enhanced recovery after surgery program reduces length of hospital stay and complications in liver resection: A PRISMA-compliant systematic review and meta-analysis of randomized controlled trials
- PMID: 28767578
- PMCID: PMC5626132
- DOI: 10.1097/MD.0000000000007628
Enhanced recovery after surgery program reduces length of hospital stay and complications in liver resection: A PRISMA-compliant systematic review and meta-analysis of randomized controlled trials
Abstract
Background: Many enhanced recovery after surgery (ERAS) guidelines have already been established in several kinds of surgeries. But due to concerns of the specific complications, it has not yet been considered the standard of care in liver surgery.
Objective: The aim of this review is to assess the effect of ERAS in patients undergoing liver surgery.
Methods: EMBASE, CNKI, PubMed, and the Cochrane Database were searched for randomized controlled trials (RCTs) comparing ERAS with conventional care in patients undergoing liver surgery. Subgroup meta-analysis between laparoscopic and open surgical approaches to liver resection was also conducted.
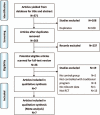
Results: Seven RCTs were included, representing 996 patients. Length of stay (LOS) (MD -3.17, 95% CI: -3.99 to -2.35, P < .00001, I = 89%) and time to first flatus (MD -0.9, 95% CI: -1.36 to -0.45, P = .0001, I = 98%) were both reduced in the ERAS group. There were also fewer complications in the ERAS group (OR 0.52, 95% CI: 0.37-0.72, P < .0001, I = 0%).
Conclusion: The ERAS program can obviously enhance short-term recovery after liver resection. It is safe and worthwhile. A specific ERAS guideline for liver resection is recommended.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures





References
-
- Lemmens L, van Zelm R, Borel Rinkes I, et al. Clinical and organizational content of clinical pathways for digestive surgery: a systematic review. Dig Surg 2009;26:91–9. - PubMed
-
- Gustafsson UO, Scott MJ, Schwenk W, et al. Guidelines for perioperative care in elective colonic surgery: Enhanced Recovery After Surgery (ERAS((R))) Society recommendations. World J Surg 2013;37:259–84. - PubMed
-
- Geltzeiler CB, Rotramel A, Wilson C, et al. Prospective study of colorectal enhanced recovery after surgery in a community hospital. JAMA Surg 2014;149:955–61. - PubMed
-
- Gouvas N, Tan E, Windsor A, et al. Fast-track vs standard care in colorectal surgery: a meta-analysis update. Int J Colorectal Dis 2009;24:1119–31. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

