Comparison of postoperative visual quality after SMILE and LASEK for high myopia: A 1-year outcome
- PMID: 28771544
- PMCID: PMC5542625
- DOI: 10.1371/journal.pone.0182251
Comparison of postoperative visual quality after SMILE and LASEK for high myopia: A 1-year outcome
Abstract
Purpose: To compare the 1-year outcome of visual quality after laser-assisted subepithelial keratomileusis (LASEK) and femtosecond laser-assisted small incision lenticule extraction (SMILE) for high myopia correction.
Materials and methods: This prospective, comparative study included 24 eyes of 24 patients in the LASEK group, with a mean spherical equivalent (SE) of -7.59 ± 1.32 diopters, and 26 eyes of 26 patients in the SMILE group, with a mean SE of -7.91 ± 1.08 diopters. Visual acuity, corneal topography, contrast sensitivity (CS), and wavefront aberrations were recorded preoperatively and compared with postoperative measurements. Objective scatter index (OSI) and modulation transfer function (MTF) cut-off frequency were measured 1 year postoperatively.
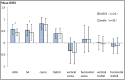
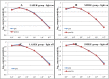
Results: One year postoperatively, the two groups demonstrated no significant difference in the CS at all spatial frequencies. The increments of higher-order aberrations (HOAs) (HOA = 0.583 ± 0.210 μm), including spherical aberration (SA) (SA = 0.546 ± 0.249 μm), were higher (P < 0.05) in the LASEK group than those in the SMILE group (HOA = 0.451 ± 0.143 μm; SA = 0.450 ± 0.340 μm) after surgery. There were no significant differences in the increments of coma and trefoil aberrations between the two groups. The OSI and MTF cut-off frequency exhibited no significant differences between the two groups postoperatively. No vision-threatening complications were noted at any stage in either group.
Conclusions: Both LASEK and SMILE are safe and effective surgical options for the correction of high myopia. SMILE has a lower HOAs and SA induction rate 1 year postoperatively.
Conflict of interest statement
Figures
References
-
- Holden BA, Fricke TR, Wilson DA, Jong M, Naidoo KS, Sankaridurg P, et al. (2016) Global Prevalence of Myopia and High Myopia and Temporal Trends from 2000 through 2050. Ophthalmology 123: 1036–1042. doi: 10.1016/j.ophtha.2016.01.006 - DOI - PubMed
-
- Fricke TR, Holden BA, Wilson DA, Schlenther G, Naidoo KS, Resnikoff S, et al. (2012) Global cost of correcting vision impairment from uncorrected refractive error. Bull World Health Organ 90: 728–738. doi: 10.2471/BLT.12.104034 - DOI - PMC - PubMed
-
- Al-Tobaigy FM (2012) Efficacy, predictability, and safety of laser-assisted subepithelial keratectomy for the treatment of myopia and myopic astigmatism. Middle East Afr J Ophthalmol 19: 304–308. doi: 10.4103/0974-9233.97931 - DOI - PMC - PubMed
-
- Chansue E, Tanehsakdi M, Swasdibutra S, McAlinden C (2015) Efficacy, predictability and safety of small incision lenticule extraction (SMILE). Eye Vis (Lond) 2: 14 doi: 10.1186/s40662-015-0024-4 - DOI - PMC - PubMed
-
- Kirwan C, O'Keefe M (2009) Comparative study of higher-order aberrations after conventional laser in situ keratomileusis and laser epithelial keratomileusis for myopia using the technolas 217z laser platform. Am J Ophthalmol 147: 77–83. doi: 10.1016/j.ajo.2008.07.014 - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

