Exploring factors related to changes in body composition, insulin sensitivity and aerobic capacity in response to a 12-week exercise intervention in overweight and obese women with and without polycystic ovary syndrome
- PMID: 28771628
- PMCID: PMC5542389
- DOI: 10.1371/journal.pone.0182412
Exploring factors related to changes in body composition, insulin sensitivity and aerobic capacity in response to a 12-week exercise intervention in overweight and obese women with and without polycystic ovary syndrome
Abstract
Objective: To determine factors associated with differential changes in body fat, insulin resistance and aerobic capacity following a 12-week exercise intervention in overweight and obese women with and without polycystic ovary syndrome (PCOS).
Methods: 16 overweight and obese women (9 PCOS; 7 without PCOS) completed a supervised progressive 12-week exercise program. Primary outcomes included changes in indicators of insulin sensitivity (including glucose infusion rate relative to fat-free mass [GIR/FFM]), body composition, and aerobic capacity (VO2 peak; 12 participants only). Comparisons were made between women with and without PCOS, and between participants who lost ≥5% (classified as exercise responders) and <5% (non-responders) in body fat (assessed by dual-energy X-ray absorptiometry).
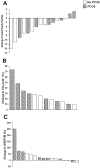
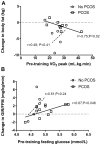
Results: Training decreased body fat percentage by (mean; 95% CI) -2.3%; -5.3, 0.7% in women with PCOS and by -6.4%; -10.9, -1.9% in women without PCOS (P = 0.08). Ten women (7 PCOS; 3 without PCOS) did not reduce body fat by ≥5%. All participants improved VO2 peak (mean change 27%; 16-39%) but four (2 PCOS; 2 without PCOS) demonstrated decreases in GIR/FFM (mean change for whole cohort: 37%; 3-71%). Android-gynoid fat ratio (0.58; 0.51, 0.66 vs 0.46; 0.40, 0.51; P<0.01) was significantly higher and GIR/FFM (6.69; 3.49, 9.90 vs 11.44; 9.15, 13.72 mg/kg/min; P = 0.01) was significantly lower in non-responders compared with responders at baseline, but non-responders had significant post-training decreases in android-gynoid ratio (-0.02; -0.04, -0.01; P = 0.03), and increases in VO2 peak (7.24; 2.28, 12.21 mL/kg/min; P = 0.01) and GIR/FFM (1.44; 0.27, 2.61 mg/kg/min; P = 0.02). In women with PCOS, pre-training VO2 peak was significantly negatively correlated with change in total body fat (r = -0.75; P = 0.02), and pre-training fasting glucose negatively correlated with changes in VO2 peak (r = -0.76; P = 0.04), but positively correlated with changes in GIR (r = 0.67; P = 0.046).
Conclusion: A high proportion of overweight and obese women with PCOS had small reductions in body fat following a 12-week exercise intervention, but nevertheless significantly reduced relative central adiposity and improved aerobic capacity and insulin sensitivity.
Conflict of interest statement
Figures
Similar articles
-
Effects of exercise on insulin resistance and body composition in overweight and obese women with and without polycystic ovary syndrome.J Clin Endocrinol Metab. 2011 Jan;96(1):E48-56. doi: 10.1210/jc.2010-0828. Epub 2010 Oct 6. J Clin Endocrinol Metab. 2011. PMID: 20926534
-
The effect of a hypocaloric diet with and without exercise training on body composition, cardiometabolic risk profile, and reproductive function in overweight and obese women with polycystic ovary syndrome.J Clin Endocrinol Metab. 2008 Sep;93(9):3373-80. doi: 10.1210/jc.2008-0751. Epub 2008 Jun 26. J Clin Endocrinol Metab. 2008. PMID: 18583464 Clinical Trial.
-
Associations of Vitamin D with Inter- and Intra-Muscular Adipose Tissue and Insulin Resistance in Women with and without Polycystic Ovary Syndrome.Nutrients. 2016 Nov 30;8(12):774. doi: 10.3390/nu8120774. Nutrients. 2016. PMID: 27916865 Free PMC article.
-
The role of obesity in the development of polycystic ovary syndrome.Curr Pharm Des. 2012;18(17):2482-91. doi: 10.2174/13816128112092482. Curr Pharm Des. 2012. PMID: 22376149 Review.
-
Exercise, or exercise and diet for the management of polycystic ovary syndrome: a systematic review and meta-analysis.Syst Rev. 2019 Feb 12;8(1):51. doi: 10.1186/s13643-019-0962-3. Syst Rev. 2019. PMID: 30755271 Free PMC article.
Cited by
-
Exercise Recommendations for Women with Polycystic Ovary Syndrome: Is the Evidence Enough?Sports Med. 2019 Aug;49(8):1143-1157. doi: 10.1007/s40279-019-01133-6. Sports Med. 2019. PMID: 31166000 Free PMC article.
-
Heat therapy improves glucose tolerance and adipose tissue insulin signaling in polycystic ovary syndrome.Am J Physiol Endocrinol Metab. 2019 Jul 1;317(1):E172-E182. doi: 10.1152/ajpendo.00549.2018. Epub 2019 May 28. Am J Physiol Endocrinol Metab. 2019. PMID: 31136202 Free PMC article. Clinical Trial.
-
Health-related physical fitness in women with polycystic ovary syndrome versus controls: a systematic review and meta-analysis.Arch Gynecol Obstet. 2024 Jan;309(1):17-36. doi: 10.1007/s00404-023-07004-w. Epub 2023 Mar 15. Arch Gynecol Obstet. 2024. PMID: 36920532
-
A Systematic Review of the Effects of Exercise on Hormones in Women with Polycystic Ovary Syndrome.J Funct Morphol Kinesiol. 2020 May 31;5(2):35. doi: 10.3390/jfmk5020035. J Funct Morphol Kinesiol. 2020. PMID: 33467251 Free PMC article. Review.
-
Effects of Different Resistance Training Frequencies on Body Composition, Cardiometabolic Risk Factors, and Handgrip Strength in Overweight and Obese Women: A Randomized Controlled Trial.J Funct Morphol Kinesiol. 2020 Jul 17;5(3):51. doi: 10.3390/jfmk5030051. J Funct Morphol Kinesiol. 2020. PMID: 33467267 Free PMC article.
References
-
- Teede HJ, Misso ML, Deeks AA, Moran LJ, Stuckey B, Wong J, et al. Assessment and management of polycystic ovary syndrome: summary of an evidence-based guideline. Med J Aust. 2011;195(6):S65 - PubMed
-
- Moran LJ, Hutchison SK, Norman RJ, Teede HJ. Lifestyle changes in women with polycystic ovary syndrome. Cochrane Database Syst Rev. 2011;(2). doi: 10.1002/14651858.CD007506.pub2 - DOI - PubMed
-
- Harrison CL, Lombard CB, Moran LJ, Teede HJ. Exercise therapy in polycystic ovary syndrome: a systematic review. Hum Reprod Update. 2011;17(2):171–83. doi: 10.1093/humupd/dmq045 - DOI - PubMed
-
- Harrison CL, Stepto NK, Hutchison SK, Teede HJ. The impact of intensified exercise training on insulin resistance and fitness in overweight and obese women with and without polycystic ovary syndrome. Clin Endocrinol (Oxf). 2012;76(3):351–7. - PubMed
-
- Jaatinen TA, Anttila L, Erkkola R, Koskinen P, Laippala P, Ruutiainen K, et al. Hormonal responses to physical exercise in patients with polycystic ovarian syndrome. Fertil Steril. 1993;60(2):262–7. . - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

