Localizing the L5 Vertebra Using Nerve Morphology on MRI: An Accurate and Reliable Technique
- PMID: 28775057
- PMCID: PMC7963613
- DOI: 10.3174/ajnr.A5311
Localizing the L5 Vertebra Using Nerve Morphology on MRI: An Accurate and Reliable Technique
Abstract
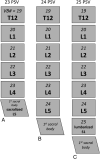
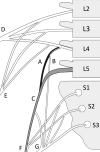
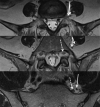
Background and purpose: Multiple methods have been used to determine the lumbar vertebral level on MR imaging, particularly when full spine imaging is unavailable. Because postmortem studies show 95% accuracy of numbering the lumbar vertebral bodies by counting the lumbar nerve roots, attention to lumbar nerve morphology on axial MR imaging can provide numbering clues. We sought to determine whether the L5 vertebra could be accurately localized by using nerve morphology on MR imaging.
Materials and methods: One hundred eight cases with full spine MR imaging were numbered from the C2 vertebral body to the sacrum with note of thoracolumbar and lumbosacral transitional states. The origin level of the L5 nerve and iliolumbar ligament were documented in all cases. The reference standard of numbering by full spine imaging was compared with the nerve morphology numbering method. Five blinded raters evaluated all lumbar MRIs with nerve morphology technique twice. Prevalence and bias-adjusted κ were used to measure interrater and intrarater reliability.
Results: The L5 nerve arose from the 24th presacral vertebra (L5) in 106/108 cases. The percentage of perfect agreement with the reference standard was 98.1% (95% CI, 93.5%-99.8%), which was preserved in transitional and numeric variation states. The iliolumbar ligament localization method showed 83.3% (95% CI, 74.9%-89.8%) perfect agreement with the reference standard. Inter- and intrarater reliability when using the nerve morphology method was strong.
Conclusions: The exiting L5 nerve can allow accurate localization of the corresponding vertebrae, which is essential for preprocedure planning in cases where full spine imaging is not available. This neuroanatomic method displays higher agreement with the reference standard compared with previously described methods, with strong inter- and intrarater reliability.
© 2017 by American Journal of Neuroradiology.
Figures

References
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous
