Cardiovascular risk after hospitalisation for unexplained syncope and orthostatic hypotension
- PMID: 28775101
- PMCID: PMC5861388
- DOI: 10.1136/heartjnl-2017-311857
Cardiovascular risk after hospitalisation for unexplained syncope and orthostatic hypotension
Abstract
Objective: To investigate the relationship of hospital admissions due to unexplained syncope and orthostatic hypotension (OH) with subsequent cardiovascular events and mortality.
Methods: We analysed a population-based prospective cohort of 30 528 middle-aged individuals (age 58±8 years; males, 40%). Adjusted Cox regression models were applied to assess the impact of unexplained syncope/OH hospitalisations on cardiovascular events and mortality, excluding subjects with prevalent cardiovascular disease.
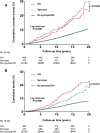
Results: After a median follow-up of 15±4 years, 524 (1.7%) and 504 (1.7%) participants were hospitalised for syncope or OH, respectively, yielding 1.2 hospital admissions per 1000 person-years for each diagnosis. Syncope hospitalisations increased with age (HR, per 1 year: 1.07, 95% CI 1.05 to 1.09), higher systolic blood pressure (HR, per 10 mm Hg: 1.06, 95% CI 1.01 to 1.12), antihypertensive treatment (HR: 1.26, 95% CI 1.00 to 1.59), use of diuretics (HR: 1.77, 95% CI 1.31 to 2.38) and prevalent cardiovascular disease (HR: 1.59, 95% CI 1.14 to 2.23), whereas OH hospitalisations increased with age (HR: 1.11, 95% CI 1.08 to 1.12) and prevalent diabetes (HR: 1.82, 95% CI 1.23 to 2.70). After exclusion of 1399 patients with prevalent cardiovascular disease, a total of 473/464 patients were hospitalised for unexplained syncope/OH before any cardiovascular event. Hospitalisation for unexplained syncope predicted coronary events (HR: 1.85, 95% CI 1.49 to 2.30), heart failure (HR: 2.24, 95% CI 1.65 to 3.04), atrial fibrillation (HR: 1.84, 95% CI 1.50 to 2.26), aortic valve stenosis (HR: 2.06, 95% CI 1.28 to 3.32), all-cause mortality (HR: 1.22, 95% CI 1.09 to 1.37) and cardiovascular death (HR: 1.72, 95% CI 1.23 to 2.42). OH-hospitalisation predicted stroke (HR: 1.66, 95% CI 1.24 to 2.23), heart failure (HR: 1.78, 95% CI 1.21 to 2.62), atrial fibrillation (HR: 1.89, 95% CI 1.48 to 2.41) and all-cause mortality (HR: 1.14, 95% CI 1.01 to 1.30).
Conclusions: Patients discharged with the diagnosis of unexplained syncope or OH show higher incidence of cardiovascular disease and mortality with only partial overlap between these two conditions.
Keywords: cardiovascular disease; hospital admission; mortality; orthostatic hypotension; unexplained syncope.
© Article author(s) (or their employer(s) unless otherwise stated in the text of the article) 2018. All rights reserved. No commercial use is permitted unless otherwise expressly granted.
Conflict of interest statement
Competing interests: All authors have completed the ICMJE uniform disclosure at www.icmje.org/coi_disclosure.pdf and declare: AF reports personal fees from Cardiome Corp. and a patent Thermo Fisher pending outside the submitted work; RDC reports grants from Boehringer-Ingelheim, Bayer and BMS/Pfizer, personal fees from Boehringer-Ingelheim, Bayer, BMS/Pfizer, Daiichi-Sankyo and Lilly outside the submitted work; RS reports personal fees and other from Medtronic Inc., St. Jude Medical Inc. outside the submitted work; RS performs consultancy for Medtronic Inc.; RS is a member of the speaker’s Bureau St. Jude Medical/Abbott Inc.; RS is shareholder in Boston Scientific Inc., Edwards Lifesciences Inc., Shire PLC, Roche SA and Astrazeneca PLC; no other relationships or activities that could appear to have influenced the submitted work.
Figures



Comment in
-
Syncope and orthostatic hypotension: early markers of cardiac disease in the general population.Heart. 2018 Mar;104(6):456-457. doi: 10.1136/heartjnl-2017-312112. Epub 2017 Aug 16. Heart. 2018. PMID: 28814494 No abstract available.
References
-
- Ricci F, De Caterina R, Fedorowski A, et al. Prognosis, and treatment. J Am Coll Cardiol 2015;66:848–60. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
