Petersen's hernia after living donor liver transplantation
- PMID: 28831719
- PMCID: PMC5567578
- DOI: 10.1186/s40792-017-0364-5
Petersen's hernia after living donor liver transplantation
Abstract
Background: Hepaticojejunostomy may be used for biliary reconstruction in certain cases of liver transplantation. In this occasion, Roux-en-Y biliary reconstruction is predominantly performed. Petersen's hernia is an internal hernia that can occur after Roux-en-Y reconstruction, and it may lead to extensive ischemic changes affecting incarcerated portions of the small bowel or Roux limb resulting in severe complications with a poor prognosis.
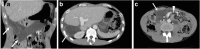
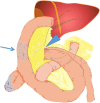
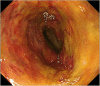
Case presentation: The present case was a 44-year-old male who underwent living donor liver transplantation (LDLT) for familial amyloid polyneuropathy and in whom biliary reconstruction was performed with Roux-en-Y hepaticojejunostomy. Two years after liver transplantation, symptomatic bowel strangulation was diagnosed by CT examination and emergent surgery was performed accordingly. On exploration, an ischemic limb associated with Petersen's hernia was observed. Although repositioning of the incarcerated bowel loop gradually improved the color of the limb, the limb failed to completely recover to a normal color. To allow accurate evaluation for the viability of the limb, we decided to perform a second-look operation after 48 h. On re-exploration, the surface of the limb remained a dark color; however, intraoperative endoscopic findings revealed only partial necrosis of the mucosa. Next, we resected the portion of ischemic damaged limb only following side-to-side jejunojejunostomy. Consequently, redoing of biliary reconstruction could be avoided and the original hepaticojejunostomy site was preserved. Although the stricture of the remnant Roux limb occurred 1 month thereafter, it was successfully managed by balloon dilation via percutaneous transhepatic biliary drainage route.
Conclusions: The occurrence of Petersen's hernia should always be considered in cases of liver transplantation with Roux-en-Y biliary reconstruction. On the basis of an accurate assessment of the extent of jejunal limb injury, reanastomosis of the hepaticojejunostomy, a potentially high-risk surgical procedure, can be avoided in emergent situations.
Keywords: Biliary reconstruction; Hepaticojejunostomy; Living donor liver transplantation; Petersen’s hernia.
Conflict of interest statement
Consent for publication
Written informed consent was obtained from the patient for publication of this Case Report and all accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures

Similar articles
-
Easy fixation effects the prevention of Peterson's hernia and Roux stasis syndrome.World J Gastrointest Surg. 2020 Aug 27;12(8):346-354. doi: 10.4240/wjgs.v12.i8.346. World J Gastrointest Surg. 2020. PMID: 32904043 Free PMC article.
-
Novel technique using a bioabsorbable prosthesis with fibrin glue fixation to prevent a Petersen's space hernia.J Surg Case Rep. 2017 Dec 15;2017(12):rjx246. doi: 10.1093/jscr/rjx246. eCollection 2017 Dec. J Surg Case Rep. 2017. PMID: 29318008 Free PMC article.
-
Petersen's hernia after laparoscopic distal gastrectomy with Roux-en-Y reconstruction for gastric cancer.Gastric Cancer. 2014 Jan;17(1):146-51. doi: 10.1007/s10120-013-0256-8. Epub 2013 Apr 5. Gastric Cancer. 2014. PMID: 23558458 Clinical Trial.
-
Petersen's hernia as a complication of bariatric surgery: CT findings.Abdom Imaging. 2011 Apr;36(2):126-9. doi: 10.1007/s00261-010-9626-4. Abdom Imaging. 2011. PMID: 20473666 Review.
-
Endoscopic management of biliary strictures after living donor liver transplantation.Clin J Gastroenterol. 2017 Aug;10(4):297-311. doi: 10.1007/s12328-017-0754-z. Epub 2017 Jun 9. Clin J Gastroenterol. 2017. PMID: 28600688 Review.
Cited by
-
Internal hernia of the small intestine around biliary catheter after living-donor liver transplantation: A case report.Int J Surg Case Rep. 2018;49:158-162. doi: 10.1016/j.ijscr.2018.06.023. Epub 2018 Jun 28. Int J Surg Case Rep. 2018. PMID: 30007264 Free PMC article.
References
-
- Petersen W. Uber Darmverschlinung nach der Gastroenterostomie. Arch Klin Chir. 1900;62:94–114.
-
- Akamatsu N, Sugawara Y, Hashimoto D. Biliary reconstruction, its complications and management of biliary complications after adult liver transplantation: a systematic review of the incidence, risk factors and outcome. Transpl Int. 2011;24(4):379–392. doi: 10.1111/j.1432-2277.2010.01202.x. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

