Engaging and staying engaged: a phenomenological study of barriers to equitable access to mental healthcare for people with severe mental disorders in a rural African setting
- PMID: 28851421
- PMCID: PMC5576237
- DOI: 10.1186/s12939-017-0657-0
Engaging and staying engaged: a phenomenological study of barriers to equitable access to mental healthcare for people with severe mental disorders in a rural African setting
Abstract
Background: In low-and middle-income countries, integration of mental health into primary care is recommended to reduce the treatment gap. In this study we explored barriers to initial and ongoing engagement of people with severe mental disorders (SMD) in rural Ethiopia after implementing integrated primary mental healthcare services.
Methods: A qualitative approach was employed. In-depth interviews were conducted with 50 key informants: service users/caregivers engaged with care (n = 17), non-engagers and their caregivers (n = 10), those who had initiated treatment but disengaged and their caregivers (n = 12) and primary healthcare professionals (n = 11). Two focus group discussions were conducted with community health workers (10 per group). Thematic analysis was used.
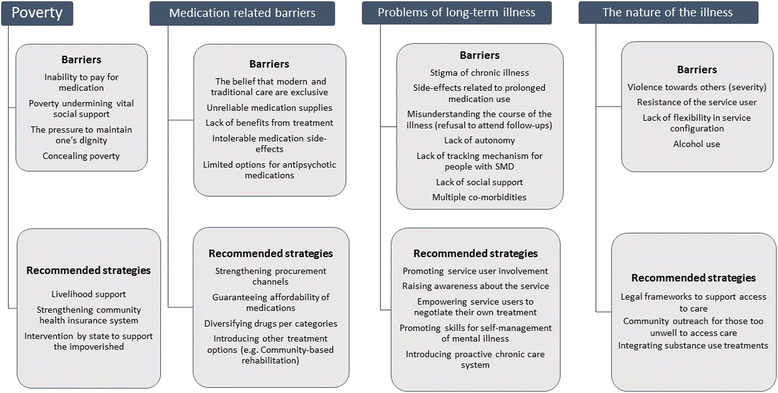
Results: Most respondents reported improved access to care, usually equated with medication, and were motivated to remain engaged due to experienced benefits of care. However, four main barriers to engagement emerged. (1) Poverty: resulting in inability to pay for medication and undermining vital social support affected engagement for all respondents. (2) Unreliable medication supplies and lack of second line options for inadequate response or intolerable side-effects. (3) The long-term nature of the illness: expectations of cure, stigma of chronic illness, low awareness about the illness and treatment and declining social support over time. (4) The nature of SMD: difficulty conveying the person when acutely disturbed and no flexibility for proactive outreach or legal frameworks to provide care when patients lacked capacity. In those who never engaged, geographical inaccessibility was an important barrier. Alternative cultural explanations for illness were only mentioned as a barrier only by two of the respondents.
Conclusion: Economic interventions may be needed to support ongoing engagement in care for people with SMD. Systems of care for chronic illness need to be strengthened in combination with legal frameworks. Expanded options for affordable and effective medication and psychosocial interventions are required for person-centred care.
Keywords: Access; Caregivers; Community mental health services; Ethiopia; Mental health; Poverty; Primary care; Sub-Saharan Africa; Task-sharing.
Conflict of interest statement
Ethics approval and consent to participate
The study was approved by the Institutional Review Board of the College of Health Sciences of Addis Ababa University. The study objectives were explained to all participants before they were invited to participate in the interviews. The Amharic version of the information sheet was given to all participants and read out for those who are not literate. Participants were asked to give their written consent or a thumb-print to indicate consent to participate in the study and publication of the information obtained. Service users who were found to be in need of medical attention were referred to the nearest PHC.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no conflict of interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Similar articles
-
'Restoring the person's life': a qualitative study to inform development of care for people with severe mental disorders in rural Ethiopia.Epidemiol Psychiatr Sci. 2017 Feb;26(1):43-52. doi: 10.1017/S2045796015001006. Epub 2016 Mar 10. Epidemiol Psychiatr Sci. 2017. PMID: 26961343 Free PMC article.
-
Participatory planning of a primary care service for people with severe mental disorders in rural Ethiopia.Health Policy Plan. 2016 Apr;31(3):367-76. doi: 10.1093/heapol/czv072. Epub 2015 Aug 17. Health Policy Plan. 2016. PMID: 26282860 Free PMC article.
-
Equitable access to integrated primary mental healthcare for people with severe mental disorders in Ethiopia: a formative study.Int J Equity Health. 2016 Jul 26;15(1):121. doi: 10.1186/s12939-016-0410-0. Int J Equity Health. 2016. PMID: 27460038 Free PMC article.
-
A comprehensive review of mental health services across selected countries in sub-Saharan Africa: assessing progress, challenges, and future direction.Discov Ment Health. 2025 Apr 7;5(1):49. doi: 10.1007/s44192-025-00177-7. Discov Ment Health. 2025. PMID: 40195169 Free PMC article. Review.
-
Supporting family engagement with child and adolescent mental health services: A scoping review.Health Soc Care Community. 2020 Sep;28(5):1333-1342. doi: 10.1111/hsc.12947. Epub 2020 Jan 17. Health Soc Care Community. 2020. PMID: 31951087
Cited by
-
Qualitative Methodology in Translational Health Research: Current Practices and Future Directions.Healthcare (Basel). 2023 Oct 1;11(19):2665. doi: 10.3390/healthcare11192665. Healthcare (Basel). 2023. PMID: 37830701 Free PMC article. Review.
-
Studying the context of psychoses to improve outcomes in Ethiopia (SCOPE): Protocol paper.PLoS One. 2024 May 9;19(5):e0293232. doi: 10.1371/journal.pone.0293232. eCollection 2024. PLoS One. 2024. PMID: 38722946 Free PMC article.
-
Implementing integrated services for people with epilepsy in primary care in Ethiopia: a qualitative study.BMC Health Serv Res. 2018 May 21;18(1):372. doi: 10.1186/s12913-018-3190-y. BMC Health Serv Res. 2018. PMID: 29783981 Free PMC article.
-
Factors affecting access to primary health care services for persons with disabilities in rural areas: a "best-fit" framework synthesis.Glob Health Res Policy. 2018 Dec 25;3:36. doi: 10.1186/s41256-018-0091-x. eCollection 2018. Glob Health Res Policy. 2018. PMID: 30603678 Free PMC article. Review.
-
Depression and Its Help Seeking Behaviors: A Systematic Review and Meta-Analysis of Community Survey in Ethiopia.Depress Res Treat. 2018 Dec 18;2018:1592596. doi: 10.1155/2018/1592596. eCollection 2018. Depress Res Treat. 2018. PMID: 30662771 Free PMC article. Review.
References
-
- Mendenhall E, De Silva MJ, Hanlon C, Petersen I, Shidhaye R, Jordans M, Luitel N, Ssebunnya J, Fekadu A, Patel V. Acceptability and feasibility of using non-specialist health workers to deliver mental health care: stakeholder perceptions from the PRIME district sites in Ethiopia, India, Nepal, South Africa, and Uganda. Soc Sci Med. 2014;118:33–42. doi: 10.1016/j.socscimed.2014.07.057. - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous