Effect of cervical cancer education and provider recommendation for screening on screening rates: A systematic review and meta-analysis
- PMID: 28873092
- PMCID: PMC5584806
- DOI: 10.1371/journal.pone.0183924
Effect of cervical cancer education and provider recommendation for screening on screening rates: A systematic review and meta-analysis
Erratum in
-
Correction: Effect of cervical cancer education and provider recommendation for screening on screening rates: A systematic review and meta-analysis.PLoS One. 2017 Dec 29;12(12):e0190661. doi: 10.1371/journal.pone.0190661. eCollection 2017. PLoS One. 2017. PMID: 29287125 Free PMC article.
Abstract
Background: Although cervical cancer is largely preventable through screening, detection and treatment of precancerous abnormalities, it remains one of the top causes of cancer-related morbidity and mortality globally.
Objectives: The objective of this systematic review is to understand the evidence of the effect of cervical cancer education compared to control conditions on cervical cancer screening rates in eligible women population at risk of cervical cancer. We also sought to understand the effect of provider recommendations for screening to eligible women on cervical cancer screening (CCS) rates compared to control conditions in eligible women population at risk of cervical cancer.
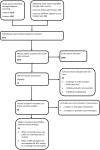
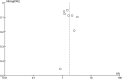
Methods: We used the PICO (Problem or Population, Interventions, Comparison and Outcome) framework as described in the Cochrane Collaboration Handbook to develop our search strategy. The details of our search strategy has been described in our systematic review protocol published in the International Prospective Register of systematic reviews (PROSPERO). The protocol registration number is CRD42016045605 available at: http://www.crd.york.ac.uk/prospero/display_record.asp?src=trip&ID=CRD42016045605. The search string was used in Pubmed, Embase, Cochrane Systematic Reviews and Cochrane CENTRAL register of controlled trials to retrieve study reports that were screened for inclusion in this review. Our data synthesis and reporting was guided by the Preferred Reporting Items for Systematic Reviews and Meta-analysis (PRISMA). We did a qualitative synthesis of evidence and, where appropriate, individual study effects were pooled in meta-analyses using RevMan 5.3 Review Manager. The Higgins I2 was used to assess for heterogeneity in studies pooled together for overall summary effects. We did assessment of risk of bias of individual studies included and assessed risk of publication bias across studies pooled together in meta-analysis by Funnel plot.
Results: Out of 3072 study reports screened, 28 articles were found to be eligible for inclusion in qualitative synthesis (5 of which were included in meta-analysis of educational interventions and 8 combined in meta-analysis of HPV self-sampling interventions), while 45 were excluded for various reasons. The use of theory-based educational interventions significantly increased CCS rates by more than double (OR, 2.46, 95% CI: 1.88, 3.21). Additionally, offering women the option of self-sampling for Human Papillomavirus (HPV) testing increased CCS rates by nearly 2-fold (OR = 1.71, 95% CI: 1.32, 2.22). We also found that invitation letters alone (or with a follow up phone contact), making an appointment, and sending reminders to patients who are due or overdue for screening had a significant effect on improving participation and CCS rates in populations at risk.
Conclusion: Our findings supports the implementation of theory-based cervical cancer educational interventions to increase women's participation in cervical cancer screening programs, particularly when targeting communities with low literacy levels. Additionally, cervical cancer screening programs should consider the option of offering women the opportunity for self-sample collection particularly when such women have not responded to previous screening invitation or reminder letters for Pap smear collection as a method of screening.
Conflict of interest statement
Figures
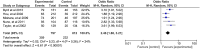

References
-
- Global Burden of Disease Cancer C, Fitzmaurice C, Dicker D, Pain A, Hamavid H, Moradi-Lakeh M, et al. The Global Burden of Cancer 2013. JAMA oncology. 2015;1(4):505–27. doi: 10.1001/jamaoncol.2015.0735 . - DOI - PMC - PubMed
-
- Allemani C, Weir HK, Carreira H, Harewood R, Spika D, Wang X-S, et al. Global surveillance of cancer survival 1995–2009: analysis of individual data for 25 676 887 patients from 279 population-based registries in 67 countries (CONCORD-2). The Lancet. 2015;385(9972):977–1010. doi: 10.1016/s0140-6736(14)62038-9 - DOI - PMC - PubMed
-
- Forouzanfar MH, Foreman KJ, Delossantos AM, Lozano R, Lopez AD, Murray CJL, et al. Breast and cervical cancer in 187 countries between 1980 and 2010: a systematic analysis. The Lancet. 2011;378(9801):1461–84. doi: 10.1016/s0140-6736(11)61351-2 - DOI - PubMed
-
- Campos NG, Tsu V, Jeronimo J, Mvundura M, Kim JJ. Evidence-based policy choices for efficient and equitable cervical cancer screening programs in low-resource settings. Cancer Med. 2017. doi: 10.1002/cam4.1123 . - DOI - PMC - PubMed
-
- WHO. WHO guidelines for Screening and Treatment of Precancerous lesions for Cervical Cancer Prevention. WHO guidelines; 2013. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

