Preoperative asymptomatic leukocytosis and postoperative outcome in cardiac surgery patients
- PMID: 28873411
- PMCID: PMC5584953
- DOI: 10.1371/journal.pone.0182118
Preoperative asymptomatic leukocytosis and postoperative outcome in cardiac surgery patients
Abstract
Background: Despite showing a prognostic value in general surgical patients, preoperative asymptomatic elevated white blood cell (WBC) count is not considered a risk factor for cardiac surgery. Whereas there is sporadic evidence of its value as a preoperative risk marker, it has not been looked at methodically as a specific index of outcome during cardiac surgery. Using a national database we sought to determine the relationship between preoperative WBC count and postoperative outcome in cardiac surgical patients.
Methods: Cardiac surgeries were extracted from the 2007-2013 American College of Surgeons National Surgical Quality Improvement Program database. Leukocytosis was defined by a preoperative WBC count greater than 11,000 cells/μL. A univariate analysis compared the incidence of adverse outcomes for patients with and without leukocytosis. A multivariate logistic regression model was constructed in order to test whether leukocytosis was an independent predictor of morbidity and mortality.
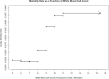
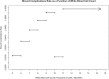
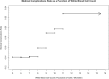
Results: Out of a total of 10,979 cardiac surgery patients 863 (7.8%) had preoperative leukocytosis. On univariate analysis, patients with leukocytosis experienced greater incidences of 30-day mortality, wound complications, and medical complications. Wound complications included surgical site infection as well as wound dehiscence. The medical complications included all other non-surgical causes of increased morbidity and infection leading to urinary tract infection, pneumonia, ventilator dependence, sepsis and septic shock. After stepwise model adjustment, leukocytosis was a strong predictor of medical complications (OR 1.22, 95% CI: 1.09-1.36, p = 0.002) with c-statistic of 0.667. However, after stepwise model adjustment leukocytosis was not a significant predictor of 30-day mortality and wound complications.
Conclusion: Preoperative leukocytosis is associated with adverse postoperative outcome after cardiac surgery and is an independent predictor of infection-related postoperative complications.
Conflict of interest statement
Figures
Similar articles
-
Asymptomatic Preoperative Leukocytosis Before Carotid Endarterectomy is Associated With Increased Risk of Stroke: A Study From NSQIP Database.Ann Vasc Surg. 2022 Feb;79:46-55. doi: 10.1016/j.avsg.2021.07.011. Epub 2021 Oct 10. Ann Vasc Surg. 2022. PMID: 34644656
-
Preoperative Leukocytosis in Colorectal Cancer Patients.J Am Coll Surg. 2015 Jul;221(1):207-14. doi: 10.1016/j.jamcollsurg.2015.03.044. Epub 2015 Mar 30. J Am Coll Surg. 2015. PMID: 26095574
-
Leukopenia and leukocytosis are associated with early postoperative complications following aseptic revision total shoulder arthroplasty.Eur J Orthop Surg Traumatol. 2025 Jun 2;35(1):227. doi: 10.1007/s00590-025-04343-z. Eur J Orthop Surg Traumatol. 2025. PMID: 40455277 Free PMC article.
-
Importance of pre- and postoperative physiotherapy in pediatric cardiac surgery.Rev Bras Cir Cardiovasc. 2009 Jul-Sep;24(3):397-400. doi: 10.1590/s0102-76382009000400021. Rev Bras Cir Cardiovasc. 2009. PMID: 20011889 Review. English, Portuguese.
-
Preoperative risk assessment tools for morbidity after cardiac surgery: a systematic review.Eur J Cardiovasc Nurs. 2022 Oct 14;21(7):655-664. doi: 10.1093/eurjcn/zvac003. Eur J Cardiovasc Nurs. 2022. PMID: 35171231
Cited by
-
A preoperative nomogram for sepsis in percutaneous nephrolithotomy treating solitary, unilateral and proximal ureteral stones.PeerJ. 2020 Jun 29;8:e9435. doi: 10.7717/peerj.9435. eCollection 2020. PeerJ. 2020. PMID: 32655994 Free PMC article.
-
Impact of preoperative nasopharyngeal cultures on surgical site infection after open heart surgery.JTCVS Open. 2021 Sep 16;8:478-486. doi: 10.1016/j.xjon.2021.09.019. eCollection 2021 Dec. JTCVS Open. 2021. PMID: 36004050 Free PMC article.
-
Identification of risk factors for infection after mitral valve surgery through machine learning approaches.Front Cardiovasc Med. 2023 Jun 13;10:1050698. doi: 10.3389/fcvm.2023.1050698. eCollection 2023. Front Cardiovasc Med. 2023. PMID: 37383697 Free PMC article.
-
The role of preoperative albumin and white blood cell count in surgical site infections following whipple surgery.Sci Rep. 2022 Nov 10;12(1):19184. doi: 10.1038/s41598-022-21849-2. Sci Rep. 2022. PMID: 36357432 Free PMC article.
-
Preoperative Hemoglobin Level Predicts Surgical Site Infections in Trauma Orthopedic Surgery: A Cohort Study.J Trop Med. 2025 Feb 4;2025:7737328. doi: 10.1155/jotm/7737328. eCollection 2025. J Trop Med. 2025. PMID: 39949898 Free PMC article.
References
-
- Lindner HA, Balaban Ü, Sturm T, Wei C, Thiel M, Schneider-Lindner V. An Algorithm for Systemic Inflammatory Response Syndrome Criteria-Based Prediction of Sepsis in a Polytrauma Cohort. Crit Care Med. 2016. doi: 10.1097/CCM.0000000000001955 - DOI - PubMed
-
- Davies MG, Hagen PO. Systemic inflammatory response syndrome. Br J Surg. 1997;84: 920–935. - PubMed
-
- Walport MJ. Complement. First of two parts. N Engl J Med. 2001;344: 1058–1066. doi: 10.1056/NEJM200104053441406 - DOI - PubMed
-
- Walport MJ. Complement. Second of two parts. N Engl J Med. 2001;344: 1140–1144. doi: 10.1056/NEJM200104123441506 - DOI - PubMed
-
- Durandy Y. Minimizing systemic inflammation during cardiopulmonary bypass in the pediatric population. Artif Organs. 2014;38: 11–18. doi: 10.1111/aor.12195 - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

