A review of antimicrobial resistance in East Africa
- PMID: 28879114
- PMCID: PMC5436405
- DOI: 10.4102/ajlm.v5i1.432
A review of antimicrobial resistance in East Africa
Abstract
Background and objectives: Knowledge of local and regional antimicrobial resistance (AMR) is important for clinical decision making. However, surveillance capacity for AMR is lacking throughout East Africa, and current AMR data are sparse. We sought to address this gap by summarising all available high-quality data on AMR in the East Africa region.
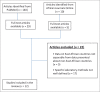
Method: We searched the PubMed database and African Journals Online archives in April and May 2015 using the search term 'antimicrobial resistance AND sub-Saharan Africa' to find articles published from 2005 onwards. Only full-text articles in English were included.
Results: We included 12 published articles in our analysis. Most articles were on bloodstream infections, hospital-based and cross-sectional in design; a majority described either community- or hospital-acquired infections. High levels of AMR to commonly-used antibiotics were reported, including 50% - 100% resistance to ampicillin and cotrimoxazole infections, emerging resistance to gentamicin (20% - 47%) and relatively high levels of resistance to ceftriaxone (46% - 69%) among Gram-negative infections. Much of the resistance was reported to be in Klebsiella species and Escherichia coli. Among Gram-positive infections, extensive resistance was reported to ampicillin (100%), gentamicin and ceftriaxone (50% - 100%), with methicillin-resistant Staphylococcus aureus prevalence ranging from 2.6% - 4.0%.
Conclusion: Overall, bacterial resistance was reported among commonly-used antibiotics (ampicillin, gentamicin and ceftriaxone), raising concern that these antibiotics may no longer be useful for treating moderate or severe bacterial infections in East Africa. Thus, empirical treatment of bacterial infections needs to be reconsidered and guided by local assessment of AMR. Improvements in the limited amount of quality data and lack of harmonisation in assessing the burden of AMR are also needed.
Conflict of interest statement
The authors declare that they have no financial or personal relationships which may have inappropriately influenced them in writing this article.
Figures
References
-
- Murray CJL, Ezzati M, Flaxman AD, et al. GBD 2010: a multi-investigator collaboration for global comparative descriptive epidemiology. Lancet. 2012;380(9859):2055–2058. http://dx.doi.org/10.1016/S0140-6736(12)62134-5 - DOI - PubMed
-
- Okeke IN, Aboderin OA, Byarugaba DK, et al. Growing problem of multidrug-resistant enteric pathogens in Africa. Emerg Infect Dis. 2007;13(11):1640–1646. http://dx.doi.org/10.3201/eid1311.070674 - DOI - PMC - PubMed
-
- World Health Organization Antimicrobial resistance: global report on surveillance. WHO Press: Geneva, Switzerland; 2014.
-
- Cockburn R, Newton PN, Agyarko EK, et al. The global threat of counterfeit drugs: why industry and governments must communicate the dangers. PLoS Med. 2005;2(4):e100 http://dx.doi.org/10.1371/journal.pmed.0020100 - DOI - PMC - PubMed
-
- Laxminarayan R, Bhutta Z, Duse A, et al. Drug resistance In: Jamison D, Breman JG, Measham AR, et al., editors. Disease control priorities in developing countries. New York: Oxford University Press; 2006; pp. 1031–1051.
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous