CORP: Ultrasound assessment of vascular function with the passive leg movement technique
- PMID: 28883048
- PMCID: PMC5814681
- DOI: 10.1152/japplphysiol.00557.2017
CORP: Ultrasound assessment of vascular function with the passive leg movement technique
Abstract
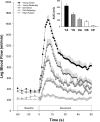
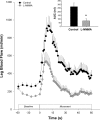
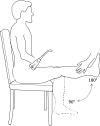
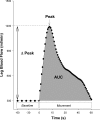
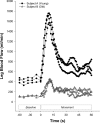
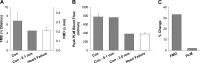
As dysfunction of the vascular system is an early, modifiable step in the progression of many cardiovascular diseases, there is demand for methods to monitor the health of the vascular system noninvasively in clinical and research settings. Validated by very good agreement with more technical assessments of vascular function, like intra-arterial drug infusions and flow-mediated dilation, the passive leg movement (PLM) technique has emerged as a powerful, yet relatively simple, test of peripheral vascular function. In the PLM technique, the change in leg blood flow elicited by the passive movement of the leg through a 90° range of motion is quantified with Doppler ultrasound. This relatively easy-to-learn test has proven to be ≤80% dependent on nitric oxide bioavailability and is especially adept at determining peripheral vascular function across the spectrum of cardiovascular health. Indeed, multiple reports have documented that individuals with decreased cardiovascular health such as the elderly and those with heart failure tend to exhibit a substantially blunted PLM-induced hyperemic response (~50 and ~85% reduction, respectively) compared with populations with good cardiovascular health such as young individuals. As specific guidelines have not yet been put forth, the purpose of this Cores of Reproducibility in Physiology (CORP) article is to provide a comprehensive reference for the assessment and interpretation of vascular function with PLM with the aim to increase reproducibility and consistency among studies and facilitate the use of PLM as a research tool with clinical relevance.
Keywords: cardiovascular health; endothelial function; guidelines; nitric oxide.
Figures


Similar articles
-
Single passive leg movement assessment of vascular function: contribution of nitric oxide.J Appl Physiol (1985). 2017 Dec 1;123(6):1468-1476. doi: 10.1152/japplphysiol.00533.2017. Epub 2017 Aug 31. J Appl Physiol (1985). 2017. PMID: 28860173 Free PMC article.
-
The passive leg movement technique for assessing vascular function: defining the distribution of blood flow and the impact of occluding the lower leg.Exp Physiol. 2019 Oct;104(10):1575-1584. doi: 10.1113/EP087845. Epub 2019 Aug 21. Exp Physiol. 2019. PMID: 31400019 Free PMC article.
-
Reliability of the passive leg movement assessment of vascular function in men.Exp Physiol. 2022 May;107(5):541-552. doi: 10.1113/EP090312. Epub 2022 Apr 5. Exp Physiol. 2022. PMID: 35294784 Free PMC article.
-
Physiological Impact and Clinical Relevance of Passive Exercise/Movement.Sports Med. 2019 Sep;49(9):1365-1381. doi: 10.1007/s40279-019-01146-1. Sports Med. 2019. PMID: 31264182 Free PMC article. Review.
-
Flow-mediated vasodilation as a diagnostic modality for vascular failure.Hypertens Res. 2008 Dec;31(12):2105-13. doi: 10.1291/hypres.31.2105. Hypertens Res. 2008. PMID: 19139600 Review.
Cited by
-
The effect of the speed and range of motion of movement on the hyperemic response to passive leg movement.Physiol Rep. 2019 Apr;7(8):e14064. doi: 10.14814/phy2.14064. Physiol Rep. 2019. PMID: 31004411 Free PMC article.
-
Sleep duration regularity, but not sleep duration, is associated with microvascular function in college students.Sleep. 2021 Feb 12;44(2):zsaa175. doi: 10.1093/sleep/zsaa175. Sleep. 2021. PMID: 32905591 Free PMC article.
-
Photoplethysmography for the Assessment of Arterial Stiffness.Sensors (Basel). 2023 Dec 17;23(24):9882. doi: 10.3390/s23249882. Sensors (Basel). 2023. PMID: 38139728 Free PMC article. Review.
-
Evidence of reduced peripheral microvascular function in young Black women across the menstrual cycle.J Appl Physiol (1985). 2021 Dec 1;131(6):1783-1791. doi: 10.1152/japplphysiol.00452.2021. Epub 2021 Oct 28. J Appl Physiol (1985). 2021. PMID: 34709068 Free PMC article.
-
Vascular dysfunction and the age-related decline in critical power.Exp Physiol. 2024 Feb;109(2):240-254. doi: 10.1113/EP091571. Epub 2023 Nov 7. Exp Physiol. 2024. PMID: 37934136 Free PMC article.
References
-
- Ahmetaj-Shala B, Kirkby NS, Knowles R, Al’Yamani M, Mazi S, Wang Z, Tucker AT, Mackenzie L, Armstrong PC, Nüsing RM, Tomlinson JA, Warner TD, Leiper J, Mitchell JA. Evidence that links loss of cyclooxygenase-2 with increased asymmetric dimethylarginine: novel explanation of cardiovascular side effects associated with anti-inflammatory drugs. Circulation 131: 633–642, 2015. doi:10.1161/CIRCULATIONAHA.114.011591. - DOI - PMC - PubMed
-
- Anderson TJ, Uehata A, Gerhard MD, Meredith IT, Knab S, Delagrange D, Lieberman EH, Ganz P, Creager MA, Yeung AC, Selwyn AP. Close relation of endothelial function in the human coronary and peripheral circulations. J Am Coll Cardiol 26: 1235–1241, 1995. doi:10.1016/0735-1097(95)00327-4. - DOI - PubMed
-
- Brook RD, Urch B, Dvonch JT, Bard RL, Speck M, Keeler G, Morishita M, Marsik FJ, Kamal AS, Kaciroti N, Harkema J, Corey P, Silverman F, Gold DR, Wellenius G, Mittleman MA, Rajagopalan S, Brook JR. Insights into the mechanisms and mediators of the effects of air pollution exposure on blood pressure and vascular function in healthy humans. Hypertension 54: 659–667, 2009. doi:10.1161/HYPERTENSIONAHA.109.130237. - DOI - PMC - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

