Impact of Center Left Ventricular Assist Device Volume on Outcomes After Implantation: An INTERMACS Analysis
- PMID: 28888521
- PMCID: PMC8453659
- DOI: 10.1016/j.jchf.2017.05.011
Impact of Center Left Ventricular Assist Device Volume on Outcomes After Implantation: An INTERMACS Analysis
Abstract
Objectives: This study examined patient outcomes after left ventricular assist device (LVAD) implantation across a range of center surgical volumes.
Background: In order for a center to qualify for reimbursement, Centers for Medicare and Medicaid Services (CMS) requires it to implant ≥10 LVADs or total artificial hearts over a 3-year period. The impact of center LVAD surgical volumes on patient outcomes has not been thoroughly scrutinized.
Methods: Center volumes were provided for 7,416 patients undergoing LVAD implantation who were enrolled in INTERMACS (Interagency Registry for Mechanically Assisted Circulatory Support). Center LVAD volume was categorized as either very low (≤10 implants/year, n = 617), low (11 to 30 implants/year, n = 2,561), medium (31 to 50 implants/year, n = 2,458), or high (>50 implants/year, n = 1,750). The main outcome of interest was patient survival based on center volume derived from Kaplan-Meier and multivariate Cox regression.
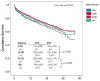
Results: Overall survival was associated with center volume (p = 0.003), as follows: 71 ± 1.8% (very low volume), 81 ± 0.8% (low volume), 83 ± 0.8% (medium volume), and 79 ± 1.0% (high volume) at 1 year. Compared with medium volume centers, the 90-day mortality was higher in very low volume (odds ratio [OR]: 1.35; p = 0.04) and high volume (OR: 1.28; p = 0.018) VAD centers. The adjusted hazard ratios (HRs) for mortality were 1.32 (95% confidence interval [CI]: 1.11 to 1.56), 1.07 (95% CI: 0.95 to 1.21), and 1.17 (95% CI: 1.03 to 1.30) for very low, low, and high volume centers, respectively. Center volume did not predict mortality (p = 0.25; n = 3,688) in INTERMACS profile 1 patients (patients who had sustained cardiogenic shock) and profile 2 patients (patients with progressive hemodynamic decline despite inotropes).
Conclusions: Center volume correlates with post-VAD survival, with worse survival noted at very-low volume centers. These findings suggest that current U.S. VAD center standards warrant reconsideration.
Keywords: LVAD; mortality; risks; volume.
Copyright © 2017 American College of Cardiology Foundation. Published by Elsevier Inc. All rights reserved.
Figures

Comment in
-
Are Outcomes Related to Left Ventricular Assist Device Center Volume?: Too Complex to Answer.JACC Heart Fail. 2017 Oct;5(10):700-702. doi: 10.1016/j.jchf.2017.07.003. Epub 2017 Sep 6. JACC Heart Fail. 2017. PMID: 28888520 No abstract available.
References
-
- Birkmeyer JD, Siewers AE, Finlayson EV, et al. Hospital volume and surgical mortality in the United States. N Engl J Med. 2002;346(15):1128–1137. - PubMed
-
- Hannan EL, Kilburn H, Jr, Bernard H, O’Donnell JF, Lukacik G, Shields EP. Coronary artery bypass surgery: the relationship between inhospital mortality rate and surgical volume after controlling for clinical risk factors. Med Care. 1991;29(11):1094–1107. - PubMed
-
- Birkmeyer JD, Stukel TA, Siewers AE, Goodney PP, Wennberg DE, Lucas FL. Surgeon volume and operative mortality in the United States. N Engl J Med. 2003;349(22):2117–2127. - PubMed
-
- Davis KF, Hohmann SF, Doukky R, Levine D, Johnson T. The Impact of Hospital and Surgeon Volume on In-Hospital Mortality of Ventricular Assist Device Recipients. Journal of Cardiac Failure. 2016;22(3):226–231. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

