Effect of cytomegalovirus and Epstein-Barr virus replication on intestinal mucosal gene expression and microbiome composition of HIV-infected and uninfected individuals
- PMID: 28906277
- PMCID: PMC5654609
- DOI: 10.1097/QAD.0000000000001579
Effect of cytomegalovirus and Epstein-Barr virus replication on intestinal mucosal gene expression and microbiome composition of HIV-infected and uninfected individuals
Erratum in
-
Effect of cytomegalovirus and Epstein-Barr virus replication on intestinal mucosal gene expression and microbiome composition of HIV-infected and uninfected individuals: Erratum.AIDS. 2018 Aug 24;32(13):1911. doi: 10.1097/01.aids.0000544237.42771.22. AIDS. 2018. PMID: 30045061 No abstract available.
Abstract
Background: HIV-infection is associated with dramatic changes in the intestinal mucosa. The impact of other viral pathogens is unclear.
Methods: One hundred and eight (108) biopsies from left and right colon (n = 79) and terminal ileum (n = 29) were collected from 19 HIV-infected and 22 HIV-uninfected participants. Levels of cytomegalovirus (CMV) and Epstein-Barr virus (EBV) DNA were measured by droplet digital PCR. Mucosal gene expression was measured via multiplex-assay. Microbiome analysis was performed using bacterial 16S-rDNA-pyrosequencing. The effect of CMV and EBV replication on the microbiome composition and mRNA-expression of selected cytokines (IL-6, IFN-γ, IL-1β, CCL2, IL-8, and IFN-β1) was evaluated.
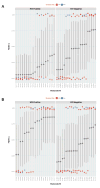
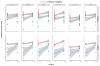
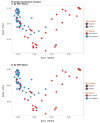
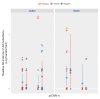
Results: Overall, CMV and EBV were detected in at least one intestinal site in 60.5 and 78.9% of participants, respectively. HIV-infected individuals demonstrated less detectable CMV (PB = 0.02); CMV was more frequently detected in terminal ileum than colon (PB = 0.05). Detectable EBV was more frequent among HIV-infected (P B= 0.04) without differences by intestinal site. The number of operational taxonomic units did not differ by CMV or EBV detection status. Among HIV-infected participants, higher CMV was only associated with lower relative abundance of Actinobacteria in the ileum (P = 0.03). Presence of CMV was associated with upregulated expression of all selected cytokines in the ileum (all P < 0.02) and higher expression of IL-8 and IFN-β1 in the colon (all P < 0.05) of HIV-uninfected participants, but not among HIV-infected. EBV had no effect on cytokine expression or microbiome composition whatsoever.
Conclusion: These results illustrate a complex interplay among HIV-infection, intestinal CMV replication, and mucosal gut environment, and highlight a possible modulatory effect of CMV on the microbial and immune homeostasis.
Conflict of interest statement
No conflicts of Interests to declare.
Figures
References
-
- Brenchley JM, Price DA, Schacker TW, et al. Microbial translocation is a cause of systemic immune activation in chronic HIV infection. Nat Med. 2006;12:1365–71. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- K24 AI100665/AI/NIAID NIH HHS/United States
- R01 MH101012/MH/NIMH NIH HHS/United States
- R21 HD094646/HD/NICHD NIH HHS/United States
- P01 AI082971/AI/NIAID NIH HHS/United States
- R21 AI134295/AI/NIAID NIH HHS/United States
- R01 MH097520/MH/NIMH NIH HHS/United States
- U01 AI043638/AI/NIAID NIH HHS/United States
- U01 AI068636/AI/NIAID NIH HHS/United States
- T32 AI007384/AI/NIAID NIH HHS/United States
- DP1 DA034978/DA/NIDA NIH HHS/United States
- P30 AI027763/AI/NIAID NIH HHS/United States
- P30 MH062512/MH/NIMH NIH HHS/United States
- P30 AI036214/AI/NIAID NIH HHS/United States
- UM1 AI106701/AI/NIAID NIH HHS/United States
- UL1 TR000100/TR/NCATS NIH HHS/United States
- U19 AI096113/AI/NIAID NIH HHS/United States
- P01 AI074621/AI/NIAID NIH HHS/United States
- P01 AI131385/AI/NIAID NIH HHS/United States
- R01 MH100974/MH/NIMH NIH HHS/United States
- UM1 AI068636/AI/NIAID NIH HHS/United States
- R24 AI106039/AI/NIAID NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

