Effect of intercostal nerve block combined with general anesthesia on the stress response in patients undergoing minimally invasive mitral valve surgery
- PMID: 28912876
- PMCID: PMC5585755
- DOI: 10.3892/etm.2017.4868
Effect of intercostal nerve block combined with general anesthesia on the stress response in patients undergoing minimally invasive mitral valve surgery
Abstract
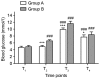
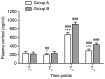
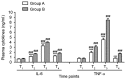
The aim of the present study was to investigate the effect of intercostal nerve block combined with general anesthesia on the stress response and postoperative recovery in patients undergoing minimally invasive mitral valve surgery (MIMVS). A total of 30 patients scheduled for MIMVS were randomly divided into two groups (n=15 each): Group A, which received intercostal nerve block combined with general anesthesia and group B, which received general anesthesia alone. Intercostal nerve block in group A was performed with 0.5% ropivacaine from T3 to T7 prior to anesthesia induction. In each group, general anesthesia was induced using midazolam, sufentanil, propofol and vecuronium. Central venous blood samples were collected to determine the concentrations of cortisol, glucose, interleukin-6 (IL-6) and tumor necrosis factor-α (TNF-α) at the following time points: During central venous catheterization (T1), 5 min prior to cardiopulmonary bypass (T2), perioperative (T3) and 24 h following surgery (T4). Clinical data, including parameters of opioid (sufentanil) consumption, time of mechanical ventilation, duration of intensive care unit (ICU) stay, visual analog scale scores and any complications arising from intercostal nerve block, were recorded. Levels of cortisol, glucose, IL-6 and TNF-α in group A were significantly lower than those in group B at T2 (all P<0.001; cortisol, P<0.05), T3 (all P<0.001) and T4 (all P<0.001; glucose, P<0.05), suggesting that intercostal nerve block combined with general anesthesia may inhibit the stress response to MIMVS. Additionally, intercostal nerve block combined with general anesthesia may significantly reduce sufentanil consumption (P<0.001), promote early tracheal extubation (P<0.001), shorten the duration of ICU stay (P<0.01) and attenuate postoperative pain (P<0.001), compared with general anesthesia alone. Thus, these results suggest that intercostal nerve block combined with general anesthesia conforms to the concept of rapid rehabilitation surgery and may be suitable for clinical practice.
Keywords: general anesthesia; intercostal nerve block; minimally invasive mitral valve surgery; postoperative analgesia; stress response.
Figures
References
LinkOut - more resources
Full Text Sources
Other Literature Sources
