Serologic Evidence of Gut-driven Systemic Inflammation in Juvenile Idiopathic Arthritis
- PMID: 28916545
- PMCID: PMC5904838
- DOI: 10.3899/jrheum.161589
Serologic Evidence of Gut-driven Systemic Inflammation in Juvenile Idiopathic Arthritis
Abstract
Objective: Accumulating evidence links juvenile idiopathic arthritis (JIA) to nonhost factors such as gut microbes. We hypothesize that children with new-onset JIA have increased intestinal bacterial translocation and circulating lipopolysaccharide (LPS).
Methods: We studied systemic treatment-naive patients with JIA [polyarticular JIA, n = 22, oligoarticular JIA, n = 31, and spondyloarthropathies (SpA), n = 16], patients with established inflammatory bowel disease-related arthritis (IBD-RA, n = 11), and 34 healthy controls. We determined circulating IgG reactivity against LPS, LPS-binding protein (LBP), α-1-acid glycoprotein (α-1AGP), and C-reactive protein (CRP) in plasma or serum from these patients and controls. Juvenile Arthritis Disease Activity Score (JADAS-27) was calculated for patients with JIA.
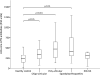
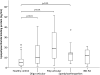
Results: Circulating anticore LPS antibody concentrations in patients with polyarticular JIA (p = 0.001), oligoarticular JIA (p = 0.024), and SpA (p = 0.001) were significantly greater than in controls, but there were no significant intergroup differences. Circulating LBP concentrations were also significantly greater in patients with polyarticular JIA (p = 0.001), oligoarticular JIA (p = 0.002), and SpA (p = 0.006) than controls, as were α-1AGP concentrations (p = 0.001, 0.001, and 0.003, respectively). No differences were observed between controls and patients with IBD-RA in any of the assays. Circulating concentrations of LBP and α-1AGP correlated strongly with CRP concentrations (r = 0.78 and r = 0.66, respectively). Anticore LPS antibody levels and CRP (r = 0.26), LBP (r = 0.24), and α-AGP (r = 0.22) concentrations had weaker correlations. JADAS-27 scores correlated with LBP (r = 0.66) and α-1AGP concentrations (r = 0.58).
Conclusion: Children with polyarticular JIA, oligoarticular JIA, and SpA have evidence of increased exposure to gut bacterial products. These data reinforce the concept that the intestine is a source of immune stimulation in JIA.
Keywords: ACUTE-PHASE PROTEINS; INTESTINAL PERMEABILITY; JUVENILE IDIOPATHIC ARTHRITIS; LIPOPOLYSACCHARIDE; LIPOPOLYSACCHARIDE-BINDING PROTEIN; α1-ACID GLYCOPROTEIN.
Figures

Comment in
-
Is Gut Microbial LPS a Potential Trigger of Juvenile Idiopathic Arthritis?J Rheumatol. 2017 Nov;44(11):1569-1571. doi: 10.3899/jrheum.170791. Epub 2017 Nov 1. J Rheumatol. 2017. PMID: 29093074 No abstract available.
References
-
- Lerner A, Matthias T. Rheumatoid arthritis-celiac disease relationship: joints get that gut feeling. Autoimmun Rev. 2015;14:1038–47. - PubMed
-
- Kokkonen J, Arvonen M, Vähäsalo P, Karttunen TJ. Intestinal immune activation in juvenile idiopathic arthritis and connective tissue disease. Scand J Rheumatol. 2007;36:386–9. - PubMed
-
- Arvonen M, Ikni L, Augustin M, Karttunen TJ, Vähäsalo P. Increase of duodenal and ileal mucosal cytotoxic lymphocytes in juvenile idiopathic arthritis. Clin Exp Rheumatol. 2010;28:128–34. - PubMed
-
- Weber P, Brune T, Ganser G, Zimmer KP. Gastrointestinal symptoms and permeability in patients with juvenile idiopathic arthritis. Clin Exp Rheumatol. 2003;21:657–62. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous
