A Systematic Review and Meta-analysis of Timing and Outcome of Intestinal Failure Surgery in Patients with Enteric Fistula
- PMID: 28924879
- PMCID: PMC5801381
- DOI: 10.1007/s00268-017-4224-z
A Systematic Review and Meta-analysis of Timing and Outcome of Intestinal Failure Surgery in Patients with Enteric Fistula
Abstract
Background: The timing of intestinal failure (IF) surgery has changed. Most specialized centers now recommend postponing reconstructive surgery for enteric fistula and emphasize that abdominal sepsis has to be resolved and the patient's condition improved. Our aim was to study the outcome of postponed surgery, to identify risk factors for recurrence and mortality, and to define more precisely the optimal timing of reconstructive surgery.
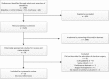
Methods: PubMed, Embase, and the Cochrane Library were systematically reviewed on the outcomes of reconstructive IF surgery (fistula recurrence, mortality, morbidity, hernia recurrence, total closure, enteral autonomy). If appropriate, meta-analyses were performed. Optimal timing was explored, and risk factors for recurrence and mortality were identified.
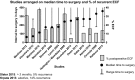
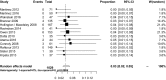
Results: Fifteen studies were included. The weighted pooled fistula recurrence rate was 19% (95% CI 15-24). Lower recurrence rates were found in studies with a longer median time and/or, at the minimum of the range, a longer time interval to surgery. Overall mortality was 3% (95% CI 2-5). Total fistula closure rates ranged from 80 to 97%. Enteral autonomy after reconstructive surgery, mentioned in four studies, varied between 79 and 100%.
Conclusions: Postponed IF surgery for enteric fistula is associated with lower recurrence. Due to the wide range of time to definitive surgery within each study, optimal timing of surgery could not be defined from published data.
Conflict of interest statement
Prof. M.A. Boermeester received institutional research grants from Acelity (Acelity Center of Expertise grant), Ipsen, Mylan, Baxter, Bard and Johnson&Johnson and is involved in consultancies for Acelity and Johnson & Johnson and a speaker for Acelity, Bard and Johnson&Johnson. Miss C.J. Vaizey is involved in consultancies for Acelity and a speaker for Acelity.
Figures
References
-
- Moher D, Liberati A, Tetzlaff J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Phys Ther. 2009;89:873–880. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous