Increasing Rates of Imaging in Failed Back Surgery Syndrome Patients: Implications for Spinal Cord Stimulation
- PMID: 28934801
- PMCID: PMC8327287
Increasing Rates of Imaging in Failed Back Surgery Syndrome Patients: Implications for Spinal Cord Stimulation
Abstract
Background: Failed back surgery syndrome (FBSS) has a high incidence following spinal surgery, is notoriously refractory to treatment, and results in high health care utilization. Spinal cord stimulation (SCS) is a well-accepted modality for pain relief in this population; however, until recently magnetic resonance imaging (MRI) was prohibited due to risk of heat conduction through the device.
Objectives: We examined trends in imaging use over the past decade in patients with FBSS to determine its impact on health care utilization and implications for patients receiving SCS.
Study design: Retrospective.
Setting: Inpatient and outpatient sample.
Methods: We identified patients from 2000 to 2012 using the Truven MarketScan database. Annual imaging rates (episodes per 1000 patient months) were determined for MRI, computed tomography (CT) scan, x-ray, and ultrasound. A multivariate Poisson regression model was used to determine imaging trends over time, and to compare imaging in SCS and non-SCS populations.
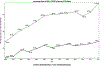
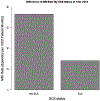
Results: A total of 311,730 patients with FBSS were identified, of which 5.17% underwent SCS implantation (n = 16,118). The median (IQR) age was 58.0 (49.0 - 67.0) years. Significant increases in imaging rate ratios were found in all years for each of the modalities. Increases were seen in the use of CT scans (rate ratio [RR] = 3.03; 95% confidence interval [CI]: 2.79 - 3.29; P < 0.0001), MRI (RR = 1.73; 95% CI: 1.61 - 1.85; P < 0.0001), ultrasound (RR = 2.00; 95% CI: 1.84 - 2.18; P < 0.0001), and x-ray (RR = 1.10; 95% CI: 1.05 - 1.15; P < 0.0001). Despite rates of MRI in SCS patients being half that in the non-SCS group, these patients underwent 19% more imaging procedures overall (P < 0.0001). SCS patients had increased rates of x-ray (RR = 1.27; 95% CI: 1.25 - 1.29), CT scans (RR = 1.32; 95% CI: 1.30 - 1.35), and ultrasound (RR = 1.10; 95% CI: 1.07 - 1.13) (all P < 0.0001).
Limitations: This study is limited by a lack of clinical and historical variables including the complexity of prior surgeries and pain symptomatology. Miscoding cannot be precluded, as this sample is taken from a large nationwide database.
Conclusions: We found a significant trend for increased use of advanced imaging modalities between the years 2000 and 2012 in FBSS patients. Those patients treated with SCS were 50% less likely to receive an MRI (as expected, given prior incompatibility of neuromodulation devices), yet 32% and 27% more likely to receive CT and x-ray, respectively. Despite the decrease in the use of MRI in those patients treated with SCS, their overall imaging rate increased by 19% compared to patients without SCS. This underscores the utility of MR-conditional SCS systems. These findings demonstrate that imaging plays a significant role in driving health care expenditures. This is the largest analysis examining the role of imaging in the FBSS population and the impact of SCS procedures. Further studies are needed to assess the impact of MRI-conditional SCS systems on future trends in imaging in FBSS patients receiving neuromodulation therapies. Key words: Failed back surgery syndrome, spinal cord stimulation, imaging, health care utilization, MRI, chronic pain, back pain, neuromodulation.
Conflict of interest statement
The remaining authors report no conflicts of interest or financial disclosures.
Figures
References
-
- Schmidt CO, Raspe H, Pfingsten M, Hasenbring M, Basler HD, Eich W, Kohlmann T. Back pain in the German adult population: Prevalence, severity, and sociodemographic correlates in a multiregional survey. Spine (Phila Pa: 1976) 2007; 32:2005–2011. - PubMed
-
- Patel AT, Ogle AA. Diagnosis and management of acute low back pain. Am Fam Physician 2000; 61:1779–1786, 1789–1790. - PubMed
-
- Dagenais S, Caro J, Haldeman S. A systematic review of low back pain cost of illness studies in the United States and internationally. Spine J 2008; 8:8–20. - PubMed
-
- Slipman CW, Shin CH, Patel RK, Isaac Z, Huston CW, Lipetz JS, Lenrow DA, Braverman DL, Vresilovic EJ. Etiologies of failed back surgery syndrome. Pain Medicine 2002; 3:200–214. - PubMed
-
- Schofferman J, Reynolds J, Herzog R, Covington E, Dreyfuss P, O’Neill C. Failed back surgery: Etiology and diagnostic evaluation. Spine J 2003; 3:400–403. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous