Respiratory outcomes after initial hospital discharge in children with ventricular shunts and bronchopulmonary dysplasia
- PMID: 28941226
- PMCID: PMC5698015
- DOI: 10.1002/ppul.23792
Respiratory outcomes after initial hospital discharge in children with ventricular shunts and bronchopulmonary dysplasia
Abstract
Introduction: Children born premature who require ventricular shunt placement for post hemorrhagic hydrocephalus are at increased risk for neurodevelopmental delay. We hypothesized that preterm infants with bronchopulmonary dysplasia (BPD) who require ventricular shunt (VS) placement are at additive risk for long-term respiratory morbidities due to their higher likelihood of neurodevelopmental delay. We also hypothesized that children with BPD and ventricular shunts would require frequent shunt revisions during early childhood following initial shunt placement.
Methods: All subjects were recruited from the Johns Hopkins Bronchopulmonary Dysplasia Clinic between January 2008 and November 2016. A review of demographic and clinical information was undertaken and a respiratory outcomes questionnaire was completed by the primary caregiver.
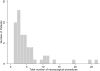
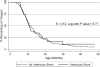
Results: Fifty-five (8.9%) of 623 subjects in the study population had ventricular shunts, with a mean 4.6 ± 2.3 years of follow-up data (range: 0.5-10.1). Subjects with VS were more likely to be born at earlier gestational ages and be discharged on supplemental oxygen compared to BPD subjects alone. Outpatient respiratory symptoms and acute care usage were similar between the two groups. BPD subjects with VS were more likely to have had gastric tubes placed. A total of 270 neurosurgical procedures were performed in subjects with VS with a mean of 4.9 ± 5.4 procedures/subject.
Conclusion: Children with ventricular shunts and BPD had similar outpatient respiratory outcomes compared to children with BPD alone; however respiratory morbidities may have been mitigated by the greater use of gastric tubes in the VS + BPD group. Multiple neurosurgical procedures were common in children with ventricular shunts.
Keywords: bronchopulmonary dysplasia (BPD); intraventricular hemorrhage; prematurity; respiratory outcomes; ventricular shunts.
© 2017 Wiley Periodicals, Inc.
Figures
References
-
- Vento M, Cheung PY, Aguar M. The first golden minutes of the extremely-low-gestational-age neonate: a gentle approach. Neonatology. 2009;95:286–298. - PubMed
-
- Limbrick DD, Jr, Mathur A, Johnston JM, et al. Neurosurgical treatment of progressive posthemorrhagic ventricular dilation in preterm infants: a 10-year single-institution study. J Neurosurg Pediatr. 2010;6:224–230. - PubMed
-
- Radic JA, Vincer M, McNeely PD. Temporal trends of intraventricular hemorrhage of prematurity in Nova Scotia from 1993 to 2012. J Neurosurg Pediatr. 2015;15:573–579. - PubMed
-
- Badhiwala JH, Hong CJ, Nassiri F, Hong BY, Riva-Cambrin J, Kulkarni AV. Treatment of posthemorrhagic ventricular dilation in preterm infants: a systematic review and meta-analysis of outcomes and complications. J Neurosurg Pediatr. 2015;16:545–555. - PubMed
-
- Winfield NR, Barker NJ, Turner ER, Quin GL. Non-pharmaceutical management of respiratory morbidity in children with severe global developmental delay. Cochrane Database Syst Rev. 2014:CD010382. https://doi.org/10.1002/14651858.CD010382.pub2. - DOI - PMC - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources