Focused echocardiography and lung ultrasound protocol for guiding treatment in acute heart failure
- PMID: 28960894
- PMCID: PMC5793966
- DOI: 10.1002/ehf2.12208
Focused echocardiography and lung ultrasound protocol for guiding treatment in acute heart failure
Abstract
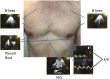
Aims: There is little evidence-based therapy existing for acute heart failure (AHF), hospitalizations are lengthy and expensive, and optimal monitoring of AHF patients during in-hospital treatment is poorly defined. We evaluated a rapid cardiothoracic ultrasound (CaTUS) protocol, combining focused echocardiographic evaluation of cardiac filling pressures, that is, medial E/e' and inferior vena cava index, with lung ultrasound (LUS) for guiding treatment in hospitalized AHF patients.
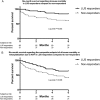
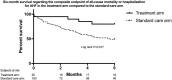
Methods and results: We enrolled 20 consecutive patients hospitalized for AHF, whose in-hospital treatment was guided using the CaTUS protocol according to a pre-specified treatment protocol targeting resolution of pulmonary congestion on LUS and lowering cardiac filling pressures. Treatment results of these 20 patients were compared with those of a standard care sample of 100 patients, enrolled previously for follow-up purposes. The standard care sample had CaTUS performed daily for follow-up and received standard in-hospital treatment without ultrasound guidance. All CaTUS exams were performed by a single experienced sonographer. The CaTUS-guided therapy resulted in significantly larger decongestion as defined by reduction in symptoms, cardiac filling pressures, natriuretic peptides, cumulative fluid loss, and resolution of pulmonary congestion (P < 0.05 for all) despite a shorter mean length of hospitalization. Congestion parameters were significantly lower also at discharge (P < 0.05 for all), without any significant difference in these parameters on admission. The treatment arm displayed better survival regarding the combined endpoint of 6 month all-cause death or AHF re-hospitalization (log rank P = 0.017). No significant difference in adverse events occurred between the groups.
Conclusions: The CaTUS-guided therapy for AHF resulted in greater decongestion during shorter hospitalization without increased adverse events in this small pilot study and might be associated with a better post-discharge prognosis.
Keywords: Acute heart failure; Cardiac filling pressures; Echocardiography; Lung ultrasound; Prognosis; Pulmonary congestion; Treatment.
© 2017 The Authors. ESC Heart Failure published by John Wiley & Sons Ltd on behalf of the European Society of Cardiology.
Conflict of interest statement
None declared.
Figures
References
-
- van Riet EE , Hoes AW, Wagenaar KP, Limburg A, Landman MA, Rutten FH. Epidemiology of heart failure: the prevalence of heart failure and ventricular dysfunction in older adults over time. A systematic review. Eur J Heart Fail 2016. Mar; 18: 242–252. - PubMed
-
- Adams KF Jr, Fonarow GC, Emerman CL, LeJemtel TH, Costanzo MR, Abraham WT, Berkowitz RL, Galvao M, Horton DP; ADHERE Scientific Advisory Committee and Investigators. Characteristics and outcomes of patients hospitalized for heart failure in the United States: rationale, design, and preliminary observations from the first 100,000 cases in the Acute Decompensated Heart Failure National Registry (ADHERE). Am Heart J 2005; 149: 209–216. - PubMed
-
- Ambrosy AP, Fonarow GC, Butler J, Chioncel O, Greene SJ, Vaduganathan M, Nodari S, Lam CS, Sato N, Shah AN, Gheorghiade M. The global health and economic burden of hospitalizations for heart failure: lessons learned from hospitalized heart failure registries. J Am Coll Cardiol 2014; 63: 1123–1133. - PubMed
-
- Greene SJ, Fonarow GC, Vaduganathan M, Khan SS, Butler J, Gheorghiade M. The vulnerable phase after hospitalization for heart failure. Nat Rev Cardiol 2015; 12: 220–229. - PubMed
-
- Ambrosy AP, Cerbin LP, Armstrong PW, Butler J, Coles A, DeVore AD, Dunlap ME, Ezekowitz JA, Felker GM, Fudim M, Greene SJ, Hernandez AF, O'Connor CM, Schulte P, Starling RC, Teerlink JR, Voors AA, Mentz RJ. Body weight change during and after hospitalization for acute heart failure: patient characteristics, markers of congestion, and outcomes: findings from the ASCEND‐HF Trial. JACC Heart Fail 2017; 5: 1–13. - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

