Anterior Cruciate Ligament Injury, Reconstruction, and the Optimization of Outcome
- PMID: 28966384
- PMCID: PMC5609382
- DOI: 10.4103/ortho.IJOrtho_237_17
Anterior Cruciate Ligament Injury, Reconstruction, and the Optimization of Outcome
Abstract
Anterior cruciate ligament reconstruction (ACLR) provides an established surgical intervention to control pathological tibiofemoral translational and rotational movement. ACLR is a safe and reproducible intervention, but there remains an underlying rate of failure to return to preinjury sporting activity levels. Postoperative pathological laxity and graft reinjury remain concerns. Previously, unrecognized meniscal lesions, disruption of the lateral capsule, and extracapsular structures offer potential avenues to treat and to therefore improve kinematic outcome and functional results, following reconstruction. Addressing laterally based injuries may also improve the durability of intraarticular ACLR. Improving the anterior cruciate ligament (ACL) graft replication of the normal ACL attachment points on the femur and the tibia, using either double bundle or anatomical single bundle techniques, improves kinematics, which may benefit outcome and functionality, following reconstruction.
Keywords: Anterior cruciate ligament; Anterior cruciate ligament reconstruction; athletic injuries; graft injury; lateral tenodesis; ramp lesion; sports injuries.
Conflict of interest statement
There are no conflicts of interest.
Figures
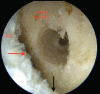
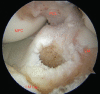
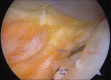
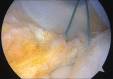
Similar articles
-
The Stability study: a protocol for a multicenter randomized clinical trial comparing anterior cruciate ligament reconstruction with and without Lateral Extra-articular Tenodesis in individuals who are at high risk of graft failure.BMC Musculoskelet Disord. 2019 May 15;20(1):216. doi: 10.1186/s12891-019-2589-x. BMC Musculoskelet Disord. 2019. PMID: 31092226 Free PMC article.
-
Restoring tibiofemoral alignment during ACL reconstruction results in better knee biomechanics.Knee Surg Sports Traumatol Arthrosc. 2018 May;26(5):1367-1374. doi: 10.1007/s00167-017-4742-0. Epub 2017 Oct 24. Knee Surg Sports Traumatol Arthrosc. 2018. PMID: 29067474
-
An In Vitro Robotic Assessment of the Anterolateral Ligament, Part 2: Anterolateral Ligament Reconstruction Combined With Anterior Cruciate Ligament Reconstruction.Am J Sports Med. 2016 Mar;44(3):593-601. doi: 10.1177/0363546515620183. Epub 2016 Feb 1. Am J Sports Med. 2016. PMID: 26831632 Clinical Trial.
-
Good mid-term outcomes and low rates of residual rotatory laxity, complications and failures after revision anterior cruciate ligament reconstruction (ACL) and lateral extra-articular tenodesis (LET).Knee Surg Sports Traumatol Arthrosc. 2020 Feb;28(2):418-431. doi: 10.1007/s00167-019-05625-w. Epub 2019 Jul 19. Knee Surg Sports Traumatol Arthrosc. 2020. PMID: 31324964
-
Passive anterior tibia translation in anterior cruciate ligament-injured, anterior cruciate ligament-reconstructed and healthy knees: a systematic review.Musculoskelet Surg. 2019 Aug;103(2):121-130. doi: 10.1007/s12306-018-0572-6. Epub 2018 Oct 16. Musculoskelet Surg. 2019. PMID: 30328030 Free PMC article.
Cited by
-
Upsurge of Sports Injuries and Their Treatment.Indian J Orthop. 2017 Sep-Oct;51(5):485-486. doi: 10.4103/ortho.IJOrtho_431_17. Indian J Orthop. 2017. PMID: 28966370 Free PMC article. No abstract available.
-
The effectiveness of arthroscopic irrigation and debridement in the management of septic arthritis following anterior cruciate ligament reconstruction: A Systematic Review and Meta-Analysis.Acta Orthop Traumatol Turc. 2025 Mar 17;59(1):7-17. doi: 10.5152/j.aott.2025.24070. Acta Orthop Traumatol Turc. 2025. PMID: 40337953 Free PMC article.
-
Associating Social Determinants of Health With PROMIS CAT Scores and Health Care Utilization After ACL Reconstruction.Orthop J Sports Med. 2023 Jan 16;11(1):23259671221139350. doi: 10.1177/23259671221139350. eCollection 2023 Jan. Orthop J Sports Med. 2023. PMID: 36683912 Free PMC article.
-
Sex, military occupation and rank are associated with risk of anterior cruciate ligament injury in tactical-athletes.BMJ Mil Health. 2023 Nov 22;169(6):535-541. doi: 10.1136/bmjmilitary-2021-002059. BMJ Mil Health. 2023. PMID: 35165197 Free PMC article.
-
A More Positive Culture by Resin-containing Media Usage after Suspicious Arthroscopic Infections in Patients Receiving Antimicrobial Therapy.Arch Bone Jt Surg. 2021 Sep;9(5):496-502. doi: 10.22038/abjs.2020.51361.2540. Arch Bone Jt Surg. 2021. PMID: 34692931 Free PMC article.
References
-
- Englund M, Eriksson K, Forssbland M, Frobell R, Kvist J, Herbertsson P. Swedish ACL Register. Annual Report. The Swedish National Knee Ligament Register. X Base. 2014
-
- Sanders TL, Maradit Kremers H, Bryan AJ, Larson DR, Dahm DL, Levy BA, et al. Incidence of anterior cruciate ligament tears and reconstruction: A 21-year population-based study. Am J Sports Med. 2016;44:1502–7. - PubMed
-
- Owens BD, Mountcastle SB, Dunn WR, DeBerardino TM, Taylor DC. Incidence of anterior cruciate ligament injury among active duty U.S. military servicemen and servicewomen. Mil Med. 2007;172:90–1. - PubMed
-
- Prodromos CC, Han Y, Rogowski J, Joyce BT, Shi K. The incidence of anterior cruciate ligament injury as a function of gender, sport, and injury-reduction programs. In: Prodromos CC, Brown CH, Fu FH, Georgoulis A, Gobbi A, Howell SM, Johnson D, Paulos LE, Shelbourne KD, editors. The Anterior Cruciate Ligament. Philadelphia: Saunders Elsevier; 2008. pp. 28–41.
LinkOut - more resources
Full Text Sources
Other Literature Sources
