Opioid Prescribing for Opioid-Naive Patients in Emergency Departments and Other Settings: Characteristics of Prescriptions and Association With Long-Term Use
- PMID: 28967517
- PMCID: PMC6295192
- DOI: 10.1016/j.annemergmed.2017.08.042
Opioid Prescribing for Opioid-Naive Patients in Emergency Departments and Other Settings: Characteristics of Prescriptions and Association With Long-Term Use
Abstract
Study objective: We explore the emergency department (ED) contribution to prescription opioid use for opioid-naive patients by comparing the guideline concordance of ED prescriptions with those attributed to other settings and the risk of patients' continuing long-term opioid use.
Methods: We used analysis of administrative claims data (OptumLabs Data Warehouse 2009 to 2015) of opioid-naive privately insured and Medicare Advantage (aged and disabled) beneficiaries to compare characteristics of opioid prescriptions attributed to the ED with those attributed to other settings. Concordance with Centers for Disease Control and Prevention (CDC) guidelines and rate of progression to long-term opioid use are reported.
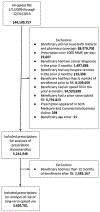
Results: We identified 5.2 million opioid prescription fills that met inclusion criteria. Opioid prescriptions from the ED were more likely to adhere to CDC guidelines for dose, days' supply, and formulation than those attributed to non-ED settings. Disabled Medicare beneficiaries were the most likely to progress to long-term use, with 13.4% of their fills resulting in long-term use compared with 6.2% of aged Medicare and 1.8% of commercial beneficiaries' fills. Compared with patients in non-ED settings, commercial beneficiaries receiving opioid prescriptions in the ED were 46% less likely, aged Medicare patients 56% less likely, and disabled Medicare patients 58% less likely to progress to long-term opioid use.
Conclusion: Compared with non-ED settings, opioid prescriptions provided to opioid-naive patients in the ED were more likely to align with CDC recommendations. They were shorter, written for lower daily doses, and less likely to be for long-acting formulations. Prescriptions from the ED are associated with a lower risk of progression to long-term use.
Copyright © 2017 American College of Emergency Physicians. Published by Elsevier Inc. All rights reserved.
Figures

Comment in
-
What Role Has Emergency Medicine Played in the Opioid Epidemic: Partner in Crime or Canary in the Coal Mine?: March 2018 Annals of Emergency Medicine Journal Club.Ann Emerg Med. 2018 Mar;71(3):426-428. doi: 10.1016/j.annemergmed.2018.01.033. Ann Emerg Med. 2018. PMID: 29458802 No abstract available.
References
-
- Vital signs: overdoses of prescription opioid pain relievers---United States, 1999--2008. MMWR Morbidity and mortality weekly report 2011;60:1487–92. - PubMed
-
- Jones CM, Mack KA, Paulozzi LJ. Pharmaceutical overdose deaths, United States, 2010. Jama 2013;309:657–9. - PubMed
-
- Hoppe JA, Kim H, Heard K. Association of emergency department opioid initiation with recurrent opioid use. Annals of emergency medicine 2015;65:493–9.e4. - PubMed
-
- Emergency Physicians Use New Tool to Detect Drug-Seekers in the ER. American College of Emergency Physicians (ACEP), 2013. (Accessed 1/24/17, at http://newsroom.acep.org/2013-07-10-Emergency-Physicians-Use-New-Tool-to....)
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

