Complications of stent placement in patients with esophageal cancer: A systematic review and network meta-analysis
- PMID: 28968416
- PMCID: PMC5624586
- DOI: 10.1371/journal.pone.0184784
Complications of stent placement in patients with esophageal cancer: A systematic review and network meta-analysis
Abstract
Background: Palliative treatments and stents are necessary for relieving dysphagia in patients with esophageal cancer. The aim of this study was to simultaneously compare available treatments in terms of complications.
Methods: Web of Science, Medline, Scopus, Cochrane Library and Embase were searched. Statistical heterogeneity was assessed using the Chi2 test and was quantified by I2. The results of this study were summarized in terms of Risk Ratio (RR). The random effects model was used to report the results. The rank probability for each treatment was calculated using the p-score.
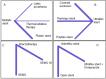
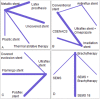
Results: Out of 17855 references, 24 RCTs reported complications including treatment related death (TRD), bleeding, stent migration, aspiration, severe pain and fistula formation. In the ranking of treatments, thermal ablative therapy (p-score = 0.82), covered Evolution® stent (p-score = 0.70), brachytherapy (p-score = 0.72) and antireflux stent (p-score = 0.74) were better treatments in the network of TRD. Thermal ablative therapy (p-score = 0.86), the conventional stent (p-score = 0.62), covered Evolution® stent (p-score = 0.96) and brachytherapy (p-score = 0.82) were better treatments in the network of bleeding complications. Covered Evolution® (p-score = 0.78), uncovered (p-score = 0.88) and irradiation stents (p-score = 0.65) were better treatments in network of stent migration complications. In the network of severe pain, Conventional self-expandable nitinol alloy covered stent (p-score = 0.73), polyflex (p-score = 0.79), latex prosthesis (p-score = 0.96) and brachytherapy (p-score = 0.65) were better treatments.
Conclusion: According to our results, thermal ablative therapy, covered Evolution® stents, brachytherapy, and antireflux stents are associated with a lower risk of TRD. Moreover, thermal ablative therapy, conventional, covered Evolution® and brachytherapy had lower risks of bleeding. Overall, fewer complications were associated with covered Evolution® stent and brachytherapy.
Conflict of interest statement
Figures



Similar articles
-
Role of Esophageal Metal Stents Placement and Combination Therapy in Inoperable Esophageal Carcinoma: A Systematic Review and Meta-analysis.Dig Dis Sci. 2018 Apr;63(4):1025-1034. doi: 10.1007/s10620-018-4957-z. Epub 2018 Feb 8. Dig Dis Sci. 2018. PMID: 29417326
-
Interventions for dysphagia in oesophageal cancer.Cochrane Database Syst Rev. 2014 Oct 30;2014(10):CD005048. doi: 10.1002/14651858.CD005048.pub4. Cochrane Database Syst Rev. 2014. PMID: 25354795 Free PMC article.
-
Radioactive self-expanding stents for palliative management of unresectable esophageal cancer: a systematic review and meta-analysis.Dis Esophagus. 2017 May 1;30(5):1-16. doi: 10.1093/dote/dow010. Dis Esophagus. 2017. PMID: 28375442
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2017 Dec 22;12(12):CD011535. doi: 10.1002/14651858.CD011535.pub2. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2020 Jan 9;1:CD011535. doi: 10.1002/14651858.CD011535.pub3. PMID: 29271481 Free PMC article. Updated.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2021 Apr 19;4(4):CD011535. doi: 10.1002/14651858.CD011535.pub4. Cochrane Database Syst Rev. 2021. Update in: Cochrane Database Syst Rev. 2022 May 23;5:CD011535. doi: 10.1002/14651858.CD011535.pub5. PMID: 33871055 Free PMC article. Updated.
Cited by
-
Efficacy and safety of standard and anti-reflux self-expanding metal stent: A systematic review and meta-analysis of randomized controlled trials.World J Gastrointest Endosc. 2019 Apr 16;11(4):271-280. doi: 10.4253/wjge.v11.i4.271. World J Gastrointest Endosc. 2019. PMID: 31040888 Free PMC article.
-
Clinical Outcomes and Prognosis of Esophageal Squamous Cell Carcinoma Presenting with Obstruction.J Gastrointest Cancer. 2024 Dec 20;56(1):35. doi: 10.1007/s12029-024-01159-8. J Gastrointest Cancer. 2024. PMID: 39702624
-
Nutritional Status and the Outcomes of Endoscopic Stenting in Benign and Malignant Diseases of Esophagus.Nutrients. 2023 Mar 21;15(6):1524. doi: 10.3390/nu15061524. Nutrients. 2023. PMID: 36986253 Free PMC article.
-
Small bowel obstruction due to migrated oesophageal metal stent.Int J Surg Case Rep. 2025 Mar;128:111034. doi: 10.1016/j.ijscr.2025.111034. Epub 2025 Feb 7. Int J Surg Case Rep. 2025. PMID: 39923446 Free PMC article.
-
Successful management of traumatic cervical esophageal injury by intraoperative microscopy and esophagoscopic assistance: a case description.Quant Imaging Med Surg. 2022 Sep;12(9):4698-4703. doi: 10.21037/qims-22-3. Quant Imaging Med Surg. 2022. PMID: 36060600 Free PMC article. No abstract available.
References
-
- Ferlay J, Shin HR, Bray F, Forman D, Mathers C, Parkin DM. Estimates of worldwide burden of cancer in 2008: GLOBOCAN 2008. International journal of cancer. 2010;127(12):2893–917. doi: 10.1002/ijc.25516 - DOI - PubMed
-
- Tytgat G, Bartelink H, Bernards R, Giaccone G, Van Lanschot J, Offerhaus G, et al. Cancer of the esophagus and gastric cardia: recent advances. Diseases of the Esophagus. 2004;17(1):10–26. doi: 10.1111/j.1442-2050.2004.00371.x - DOI - PubMed
-
- Sreedharan A, Harris K, Crellin A, Forman D, Everett SM. Interventions for dysphagia in oesophageal cancer. The Cochrane database of systematic reviews. 2009;(4):Cd005048 Epub 2009/10/13. doi: 10.1002/14651858.CD005048.pub2 . - DOI - PubMed
-
- Irani S, Kozarek R. Esophageal stents: past, present, and future. Techniques in Gastrointestinal Endoscopy. 2010;12(4):178–90.
-
- Amdal CD, Jacobsen AB, Sandstad B, Warloe T, Bjordal K. Palliative brachytherapy with or without primary stent placement in patients with oesophageal cancer, a randomised phase III trial. Radiotherapy and Oncology. 2013;107(3):428–33. doi: 10.1016/j.radonc.2013.04.008 - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

