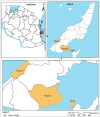
Lymphatic filariasis transmission on Mafia Islands, Tanzania: Evidence from xenomonitoring in mosquito vectors
- PMID: 28985217
- PMCID: PMC5646871
- DOI: 10.1371/journal.pntd.0005938
Lymphatic filariasis transmission on Mafia Islands, Tanzania: Evidence from xenomonitoring in mosquito vectors
Abstract
Introduction: Lymphatic filariasis (LF) is a chronic nematode infection transmitted by mosquitoes and in sub-Saharan Africa it is caused by Wuchereria bancrofti. The disease was targeted for global elimination by 2020 using repeated community-wide mass drug administration (MDA) distributed in endemic areas. However, recently, there has been a growing recognition of the potential role of including vector control as a supplement to MDA to achieve elimination goal. This study was carried out to determine mosquito abundance and transmission of bancroftian filariasis on Mafia Islands in Tanzania as a prerequisite for a search for appropriate vector control methods to complement the ongoing MDA campaign.
Methods: Mosquitoes were collected indoor and outdoor using Centre for Disease Control (CDC) light and gravid traps, respectively. Collected mosquitoes were identified based on their differential morphological features and Anopheles gambiae complex and An. funestus group were further identified to their respective sibling species by polymerase chain reaction (PCR). Filarial mosquito vectors were then examined for infection with Wuchereria bancrofti by microscopy and PCR technique.
Results: Overall, a total of 35,534 filarial mosquito vectors were collected, of which Anopheles gambiae complex, An. funestus group and Culex quinquefasciatus Say accounted for 1.3, 0.5 and 98.2%, respectively. Based on PCR identification, An. gambiae sensu stricto (s.s) and An. funestus s.s sibling species accounted for 88.3% and 99.1% of the identified members of the An. gambiae complex and An. funestus group, respectively. A total of 7,936 mosquitoes were examined for infection with W. bancrofti by microscopy. The infection and infectivity rates were 0.25% and 0.08%, respectively. Using pool screen PCR technique, analysis of 324 mosquito pools (each with 25 mosquitoes) resulted to an estimated infection rate of 1.7%.
Conclusion: The study has shown that Cx. quinquefasciatus is the dominant mosquito on Mafia Islands. By using mosquito infectivity as proxy to human infection, the study indicates that W. bancrofti transmission is still ongoing on Mafia Islands after more than a decade of control activities based on MDA.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
Lymphatic filariasis, infection status in Culex quinquefasciatus and Anopheles species after six rounds of mass drug administration in Masasi District, Tanzania.Infect Dis Poverty. 2021 Mar 1;10(1):20. doi: 10.1186/s40249-021-00808-5. Infect Dis Poverty. 2021. PMID: 33648600 Free PMC article.
-
Lymphatic filariasis transmission in Rufiji District, southeastern Tanzania: infection status of the human population and mosquito vectors after twelve rounds of mass drug administration.Parasit Vectors. 2018 Nov 13;11(1):588. doi: 10.1186/s13071-018-3156-2. Parasit Vectors. 2018. PMID: 30424781 Free PMC article.
-
Molecular xenomonitoring reveals Anopheles funestus and An. rivulorum as the primary vectors of lymphatic filariasis in coastal Kenya.Parasit Vectors. 2024 Oct 9;17(1):425. doi: 10.1186/s13071-024-06513-0. Parasit Vectors. 2024. PMID: 39385178 Free PMC article.
-
Prospects, drawbacks and future needs of xenomonitoring for the endpoint evaluation of lymphatic filariasis elimination programs in Africa.Trans R Soc Trop Med Hyg. 2016 Feb;110(2):90-7. doi: 10.1093/trstmh/trv104. Trans R Soc Trop Med Hyg. 2016. PMID: 26822601 Review.
-
Mosquitoes, Lymphatic Filariasis, and Public Health: A Systematic Review of Anopheles and Aedes Surveillance Strategies.Pathogens. 2023 Nov 29;12(12):1406. doi: 10.3390/pathogens12121406. Pathogens. 2023. PMID: 38133290 Free PMC article. Review.
Cited by
-
Lymphatic filariasis, infection status in Culex quinquefasciatus and Anopheles species after six rounds of mass drug administration in Masasi District, Tanzania.Infect Dis Poverty. 2021 Mar 1;10(1):20. doi: 10.1186/s40249-021-00808-5. Infect Dis Poverty. 2021. PMID: 33648600 Free PMC article.
-
Lymphatic filariasis elimination status: Wuchereria bancrofti infections in human populations and factors contributing to continued transmission after seven rounds of mass drug administration in Masasi District, Tanzania.PLoS One. 2022 Jan 19;17(1):e0262693. doi: 10.1371/journal.pone.0262693. eCollection 2022. PLoS One. 2022. PMID: 35045109 Free PMC article.
-
Culex species diversity, susceptibility to insecticides and role as potential vector of Lymphatic filariasis in the city of Yaoundé, Cameroon.PLoS Negl Trop Dis. 2019 Apr 3;13(4):e0007229. doi: 10.1371/journal.pntd.0007229. eCollection 2019 Apr. PLoS Negl Trop Dis. 2019. PMID: 30943198 Free PMC article.
-
Molecular xenomonitoring as a post-MDA surveillance tool for global programme to eliminate lymphatic filariasis: Field validation in an evaluation unit in India.PLoS Negl Trop Dis. 2020 Jan 24;14(1):e0007862. doi: 10.1371/journal.pntd.0007862. eCollection 2020 Jan. PLoS Negl Trop Dis. 2020. PMID: 31978060 Free PMC article.
-
Characterizations of Larval Gut Bacteria of Anopheles subpictus Grassi (1899) and their Role in Mosquito Development in Hooghly, West Bengal, India.Appl Biochem Biotechnol. 2022 Dec;194(12):6140-6163. doi: 10.1007/s12010-021-03706-6. Epub 2022 Jul 27. Appl Biochem Biotechnol. 2022. PMID: 35895250
References
-
- World Health Organization; Global Programme to Eliminate Lymphatic Filariasis: Managing Morbidity and Preventing Disability. Geneva, Switzerland: WHO, 2013.
-
- Zeldenryk LM, Gray M, Speare R, Gordon S, Melrose W. The emerging story of disability associated with lymphatic filariasis: A critical review. PLoS Negl Trop Dis. 2011, 5:e1366 doi: 10.1371/journal.pntd.0001366 - DOI - PMC - PubMed
-
- Bockarie MJ, Pedersen EM, White GB, Michael E. Role of vector control in the global program to eliminate lymphatic filariasis. Annu Rev Entomol. 2009, 54:469–87. doi: 10.1146/annurev.ento.54.110807.090626 - DOI - PubMed
-
- Hotez PJ, Kamath A. Neglected tropical diseases in sub-saharan Africa: review of their prevalence, distribution, and disease burden. PLoS Negl Trop Dis. 2009, 3:e412 doi: 10.1371/journal.pntd.0000412 - DOI - PMC - PubMed
-
- Malecela MN, Lazarus W, Mwingira U, Mwakitalu E, Makene C, Kabali C, Mackenzie C: Eliminating LF : A progress report from Tanzania. J Lymph. 2009, 4:10–12.
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources