Heavy metals exposure levels and their correlation with different clinical forms of fetal growth restriction
- PMID: 28985223
- PMCID: PMC5630121
- DOI: 10.1371/journal.pone.0185645
Heavy metals exposure levels and their correlation with different clinical forms of fetal growth restriction
Abstract
Background: Prenatal heavy metals exposure has shown a negative impact on birth weight. However, their influence on different clinical forms of fetal smallness was never assessed.
Objectives: To investigate whether there is a differential association between heavy metals exposure and fetal smallness subclassification into intrauterine growth restriction (IUGR) and small-for-gestational age (SGA).
Method: In this prospective case-control study, we included 178 mother-infant pairs; 96 of appropriate for gestational age (AGA) and 82 of small fetuses diagnosed in third trimester. The small ones were further subclassified into IUGR, n = 49 and SGA, n = 33. Cadmium (Cd), mercury (Hg), lead (Pb), arsenic (As) and zinc (Zn) levels were measured in the maternal and cord serum, and in the placentas of the three groups.
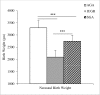
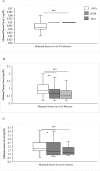
Results: Maternal serum level of Cd (p<0.001) was higher in the small fetuses compared to AGA. Fetal serum level of Cd (p<0.001) was increased in the small fetuses compared to AGA. Fetal serum level of Hg (p<0.05) showed an increase in SGA compared to both IUGR and AGA. Fetal serum level of Zn was increased in the AGA (p < 0.001) compared to each of the small fetuses groups. Only differences in the levels between the small fetuses' subgroups were detected in the fetal serum levels of Cd and Hg. Fetal birth weight was negatively correlated with the fetal serum level of Cd (p < 0.001). No differences in the placental heavy metal levels were observed among the groups.
Conclusion: Fetal serum levels of Cd showed differential correlation between small fetuses' clinical subclassification, which together with the increased Cd levels in both maternal and fetal serum of the small fetuses reinforce the negative influence of heavy metals on birth weight. These findings provide more opportunities to verify the role of heavy metals exposure in relation to small fetuses' subclassification.
Conflict of interest statement
Figures

References
-
- Bernstein IM, Horbar JD, Badger GJ, Ohlsson A, Golan A. Morbidity and mortality among very-low-birth-weight neonates with intrauterine growth restriction. The Vermont Oxford Network. Am J Obstet Gynecol. 2000. January; 182(1 Pt 1):198–206. - PubMed
-
- Brodsky D, Christou H. Current concepts in intrauterine growth restriction. J Intensive Care Med. 2004. Nov-Dec; 19(6):307–19. doi: 10.1177/0885066604269663 - DOI - PubMed
-
- Hunt CE. Small for gestational age infants and sudden infant death syndrome: a confluence of complex conditions. Arch Dis Child Fetal Neonatal Ed. 2007. November; 92(6):F428–9. doi: 10.1136/adc.2006.112243 - DOI - PMC - PubMed
-
- Bamfo J K and Odibo AO. Diagnosis and Management of Fetal Growth Restriction. J Pregnancy. 2011; 2011: 640715 doi: 10.1155/2011/640715 - DOI - PMC - PubMed
-
- Markel TA, Engelstad H, and Poindexter BB. Predicting Disease Severity of Necrotizing Enterocolitis: How to Identify Infants for Future Novel Therapies. J Clin Neonatol. 2014. Jan-Mar; 3(1): 1–9. doi: 10.4103/2249-4847.128717 - DOI - PMC - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

