Alcoholic Myopathy: Pathophysiologic Mechanisms and Clinical Implications
- PMID: 28988574
- PMCID: PMC5513686
Alcoholic Myopathy: Pathophysiologic Mechanisms and Clinical Implications
Abstract
Skeletal muscle dysfunction (i.e., myopathy) is common in patients with alcohol use disorder. However, few clinical studies have elucidated the significance, mechanisms, and therapeutic options of alcohol-related myopathy. Preclinical studies indicate that alcohol adversely affects both anabolic and catabolic pathways of muscle-mass maintenance and that an increased proinflammatory and oxidative milieu in the skeletal muscle is the primary contributing factor leading to alcohol-related skeletal muscle dysfunction. Decreased regenerative capacity of muscle progenitor cells is emerging as an additional mechanism that contributes to alcohol-induced loss in muscle mass and impairment in muscle growth. This review details the epidemiology of alcoholic myopathy, potential contributing pathophysiologic mechanisms, and emerging literature on novel therapeutic options.
Conflict of interest statement
The authors declare that they have no competing financial interests.
Figures
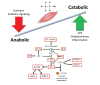


References
-
- Anty R, Canivet CM, Patouraux S, et al. Severe vitamin D deficiency may be an additional cofactor for the occurrence of alcoholic steatohepatitis. Alcoholism: Clinical and Experimental Research. 2015;39(6):1027–1033. - PubMed
-
- Barnes MJ, Mundel T, Stannard SR. Post-exercise alcohol ingestion exacerbates eccentric-exercise induced losses in performance. European Journal of Applied Physiology. 2010;108(5):1009–1014. - PubMed
-
- Bouchery EE, Harwood HJ, Sacks JJ, et al. Economic costs of excessive alcohol consumption in the U.S., 2006. American Journal of Preventive Medicine. 2011;41(5):516–524. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

