Rapid enteric testing to permit targeted antimicrobial therapy, with and without Lactobacillus reuteri probiotics, for paediatric acute diarrhoeal disease in Botswana: A pilot, randomized, factorial, controlled trial
- PMID: 28991918
- PMCID: PMC5633142
- DOI: 10.1371/journal.pone.0185177
Rapid enteric testing to permit targeted antimicrobial therapy, with and without Lactobacillus reuteri probiotics, for paediatric acute diarrhoeal disease in Botswana: A pilot, randomized, factorial, controlled trial
Erratum in
-
Correction: Rapid enteric testing to permit targeted antimicrobial therapy, with and without Lactobacillus reuteri probiotics, for paediatric acute diarrhoeal disease in Botswana: A pilot, randomized, factorial, controlled trial.PLoS One. 2018 Mar 21;13(3):e0194957. doi: 10.1371/journal.pone.0194957. eCollection 2018. PLoS One. 2018. PMID: 29561910 Free PMC article.
Abstract
Introduction: Diarrhoeal disease is the second-leading cause of death in young children. Current guidelines recommend treating children with acute non-bloody diarrhea with oral rehydration solutions and zinc, but not antimicrobials. However, in many resource-limited settings, infections with treatable enteric bacterial and protozoan pathogens are common. Probiotics have shown promise as an adjunct treatment for diarrhoea but have not been studied in sub-Saharan Africa.
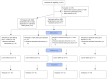
Methods: We conducted a pilot, factorial, randomized, placebo-controlled trial of children aged 2-60 months hospitalized in Botswana for acute non-bloody diarrhoea. A rapid test-and-treat intervention, consisting of multiplex PCR testing of rectal swabs taken at enrolment, accompanied by targeted antimicrobial therapy if treatable pathogens were detected, was compared to the reference standard of no stool testing. Additionally, Lactobacillus reuteri DSM 17938 x 60 days was compared to placebo treatment. The main objective of this pilot study was to assess feasibility. The primary clinical outcome was the increase in age-standardized height (HAZ) at 60 days adjusted for baseline HAZ.
Results: Seventy-six patients were enrolled over a seven-month study period. We judged that the recruitment rate, lab processing times, communication protocols, provision of specific antimicrobials, and follow-up rates were acceptable. Compared to the reference arm (no stool testing and placebo treatment), the combination of the rapid test-and-treat strategy plus L. reuteri DSM 17938 was associated with an increase of 0.61 HAZ (95% CI 0.09-1.13) and 93% lower odds of recurrent diarrhoea (OR 0.07, 95%CI 0.01-0.61) at 60 days.
Discussion: We demonstrated that it was feasible to evaluate the study interventions in Botswana. Despite the small sample size, we observed a statistically significant increase in HAZ at 60 days and significantly lower odds of recurrent diarrhoea in children receiving both rapid test-and-treat and L. reuteri. There is sufficient evidence to warrant proceeding with a larger follow-up trial in a similar setting.
Conflict of interest statement
References
-
- GBD Mortality and Causes of Death Collaborators. Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980–2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet. 2016;388(10053):1459–544. doi: 10.1016/S0140-6736(16)31012-1 . - DOI - PMC - PubMed
-
- Mata LJ, Urrutia JJ, Albertazzi C, Pellecer O, Arellano E. Influence of recurrent infections on nutrition and growth of children in Guatemala. The American journal of clinical nutrition. 1972;25(11):1267–75. . - PubMed
-
- Scrimshaw NS. Historical concepts of interactions, synergism and antagonism between nutrition and infection. The Journal of nutrition. 2003;133(1):316S–21S. . - PubMed
-
- Collins S, Dent N, Binns P, Bahwere P, Sadler K, Hallam A. Management of severe acute malnutrition in children. Lancet. 2006;368(9551):1992–2000. doi: 10.1016/S0140-6736(06)69443-9 . - DOI - PubMed
-
- Bhutta ZA, Black RE. Global maternal, newborn, and child health—so near and yet so far. The New England journal of medicine. 2013;369(23):2226–35. doi: 10.1056/NEJMra1111853 . - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous