Neoadjuvant treatment of pancreatic adenocarcinoma: a systematic review and meta-analysis of 5520 patients
- PMID: 29017581
- PMCID: PMC5634869
- DOI: 10.1186/s12957-017-1240-2
Neoadjuvant treatment of pancreatic adenocarcinoma: a systematic review and meta-analysis of 5520 patients
Abstract
Background: Recent years have seen standardization of the anatomic definitions of pancreatic adenocarcinoma, and increasing utilization of neoadjuvant therapy (NAT). The aim of the current review was to summarize the evidence for NAT in pancreatic adenocarcinoma since 2009, when consensus criteria for resectable (R), borderline resectable (BR), and locally advanced (LA) disease were endorsed.
Methods: PubMed search was undertaken along with extensive backward search of the references of published articles to identify studies utilizing NAT for pancreatic adenocarcinoma. Abstracts from ASCO-GI 2014 and 2015 were also searched.
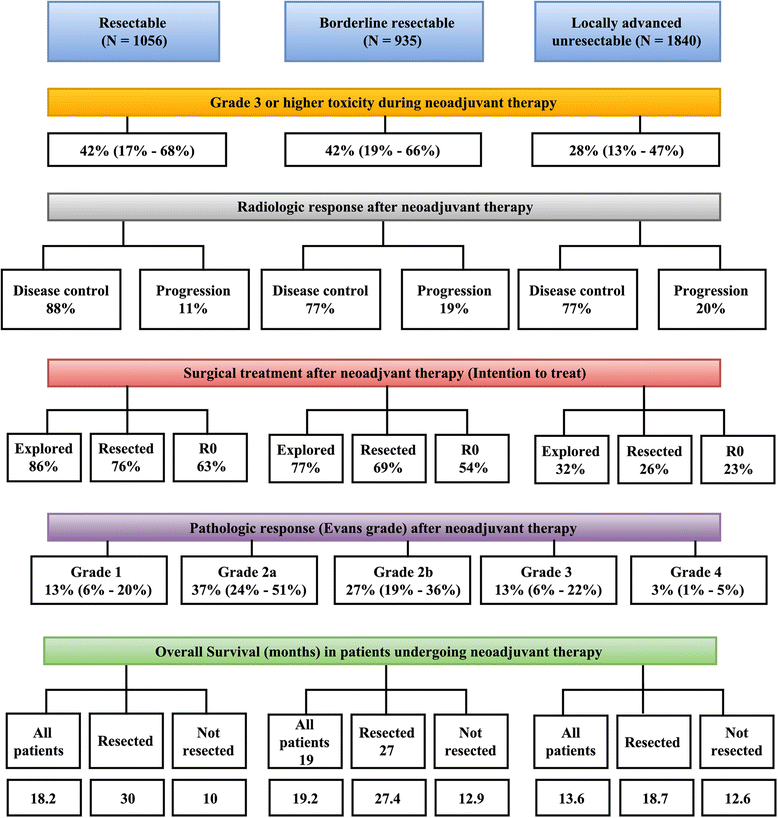
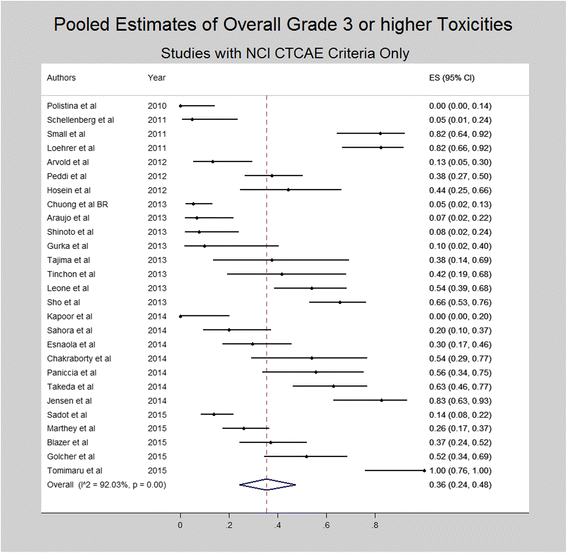
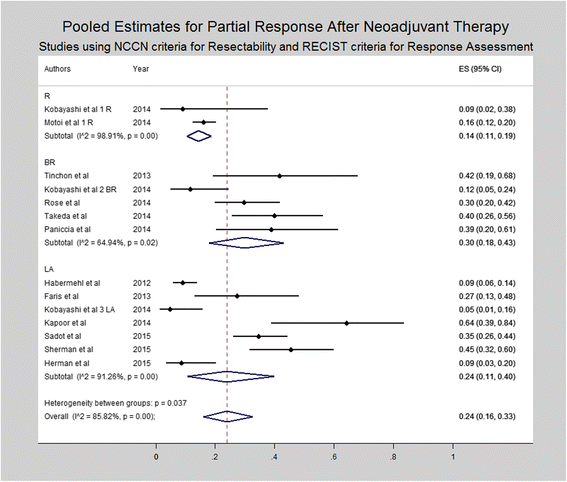
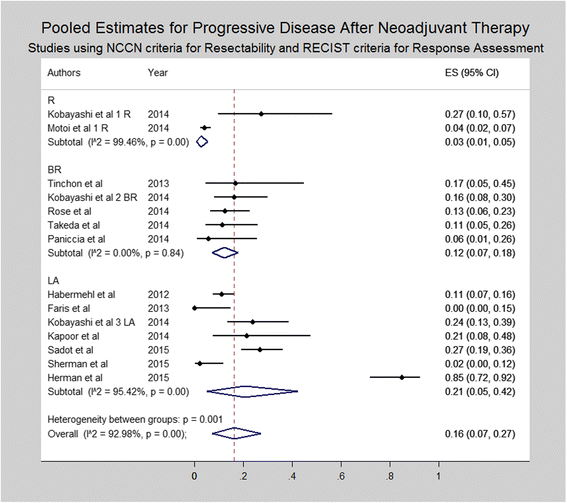
Results: A total of 96 studies including 5520 patients were included in the final quantitative synthesis. Pooled estimates revealed 36% grade ≥ 3 toxicities, 5% biliary complications, 21% hospitalization rate and low mortality (0%, range 0-16%) during NAT. The majority of patients (59%) had stable disease. On an intention-to-treat basis, R0-resection rates varied from 63% among R patients to 23% among LA patients. R0 rates were > 80% among all patients who were resected after NAT. Among R and BR patients who underwent resection after NAT, median OS was 30 and 27.4 months, respectively.
Conclusions: The current study summarizes the recent literature for NAT in pancreatic adenocarcinoma and demonstrates improving outcomes after NAT compared to those historically associated with a surgery-first approach for pancreatic adenocarcinoma.
Keywords: Neoadjuvant therapy; Outcomes; Pancreatic adenocarcinoma; Pancreatic cancer; Survival.
Conflict of interest statement
Ethics approval and consent to participate
Not applicable as the current article is a review.
Consent for publication
Not applicable
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures



References
-
- Siegel RL, Miller KD, Jemal A. Cancer statistics, 2017. CA Cancer J Clin. 2017;67:7–30. - PubMed
-
- National Cancer Institute Surveillance, Epidemiology and End Results Program SEER Stat Fact Sheets: Pancreas Cancer http://seercancergov/statfacts/html/pancreashtml Accessed July 13, 2016.
-
- Miller KD, Siegel RL, Lin CC, Mariotto AB, Kramer JL, Rowland JH, Stein KD, Alteri R, Jemal A. Cancer treatment and survivorship statistics, 2016. CA Cancer J Clin. 2016;66:271–289. - PubMed
-
- Abrams RA, Lowy AM, O'Reilly EM, Wolff RA, Picozzi VJ, Pisters PW. Combined modality treatment of resectable and borderline resectable pancreas cancer: expert consensus statement. Ann Surg Oncol. 2009;16:1751–1756. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

