Comparison of DWIBS/T2 image fusion and PET/CT for the diagnosis of cancer in the abdominal cavity
- PMID: 29042975
- PMCID: PMC5639341
- DOI: 10.3892/etm.2017.4987
Comparison of DWIBS/T2 image fusion and PET/CT for the diagnosis of cancer in the abdominal cavity
Abstract
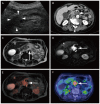
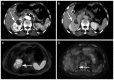
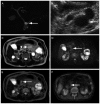
Fusion images of diffusion-weighted whole-body imaging with background body signal suppression and T2-weighted image (DWIBS/T2) demonstrate a strong signal for malignancies, with a high contrast against the surrounding tissues, and enable anatomical analysis. In the present study, DWIBS/T2 was compared with 18F-fluorodeoxyglucose (18F-FDG) positron emission tomography/computed tomography (PET/CT) for diagnosing cancer in the abdomen. Patient records, including imaging results of examination conducted between November 2012 and May 2014, were analyzed retrospectively. In total, 10 men (age, 73.6±9.6 years) and 8 women (age, 68.9±7.1 years) were enrolled into the current study. Of the enrolled patients, 2 were diagnosed with hepatocellular carcinoma, 1 with cholangiocellular carcinoma, 1 with liver metastasis, 2 with pancreatic ductal adenocarcinoma, 1 with renal cell carcinoma and 1 with malignant lymphoma. Benign lesions were also analyzed, including adenomyomatosis of the gallbladder (5 patients), intraductal papillary mucinous neoplasm (4 patients) and right adrenal adenoma (1 case). All the patients with cancer showed positive results on DWIBS/T2 images. However, only 7 out of 8 patients were positive with PET/CT. One patient with right renal cellular carcinoma was positive with DWIBS/T2, but negative with PET/CT. All the patients with benign lesions were negative with DWIBS/T2 and PET/CT. In conclusion, DWIBS/T2 was more sensitive in diagnosing cancer of organs in the abdominal cavity compared with PET/CT. Furthermore, negative results with DWIBS/T2 and PET/CT were useful for the diagnosis of benign lesions, such as adenomyomatosis of the gallbladder and intraductal papillary mucinous neoplasm.
Keywords: adenomyomatosis of the gallbladder; computed tomography; endoscopic ultrasonography; intraductal papillary mucinous neoplasm; pancreatic ductal adenocarcinoma.
Figures
Similar articles
-
Diffusion-weighted whole body imaging with background body signal suppression/T2 image fusion is negative for patients with intraductal papillary mucinous neoplasm.Hepatogastroenterology. 2015 Mar-Apr;62(138):463-5. Hepatogastroenterology. 2015. PMID: 25916083
-
Negative signals for adenomyomatosis of the gallbladder upon diffusion-weighted whole body imaging with background body signal suppression/T2-weighted image fusion analysis.Exp Ther Med. 2016 May;11(5):1777-1780. doi: 10.3892/etm.2016.3126. Epub 2016 Mar 2. Exp Ther Med. 2016. PMID: 27168802 Free PMC article.
-
Diffusion-weighted whole-body imaging with background body signal suppression/T2 image fusion and positron emission tomography/computed tomography of upper gastrointestinal cancers.Abdom Imaging. 2015 Oct;40(8):3012-9. doi: 10.1007/s00261-015-0545-2. Abdom Imaging. 2015. PMID: 26350283
-
Diagnostic accuracy of diffusion-weighted whole-body imaging with background body signal suppression/T2-weighted image fusion for the detection of abdominal solid cancer.Exp Ther Med. 2017 Jun;13(6):3509-3515. doi: 10.3892/etm.2017.4432. Epub 2017 May 5. Exp Ther Med. 2017. PMID: 28587434 Free PMC article.
-
Systematic review of the utility of 18-FDG PET in the preoperative evaluation of IPMNs and cystic lesions of the pancreas.Surgery. 2019 May;165(5):929-937. doi: 10.1016/j.surg.2018.11.006. Epub 2018 Dec 18. Surgery. 2019. PMID: 30577952
Cited by
-
Clinical Value of Diffusion-Weighted Whole-Body Imaging with Background Body Signal Suppression (DWIBS) for Staging of Patients with Suspected Head and Neck Cancer.Tomography. 2022 Oct 9;8(5):2522-2532. doi: 10.3390/tomography8050210. Tomography. 2022. PMID: 36287809 Free PMC article.
-
The Influence of Bowel Preparation on ADC Measurements: Comparison between Conventional DWI and DWIBS Sequences.Medicina (Kaunas). 2019 Jul 21;55(7):394. doi: 10.3390/medicina55070394. Medicina (Kaunas). 2019. PMID: 31330916 Free PMC article.
-
Two cases of oligometastatic castration-resistant prostate cancer detected by diffusion-weighted whole-body imaging with background body signal suppression.IJU Case Rep. 2020 Feb 17;3(2):65-68. doi: 10.1002/iju5.12146. eCollection 2020 Mar. IJU Case Rep. 2020. PMID: 32743473 Free PMC article.
References
-
- Goji T, Kimura T, Miyamoto H, Takehara M, Kagemoto K, Okada Y, Okazaki J, Takaoka Y, Miyamoto Y, Mitsui Y, et al. A phase I/II study of fixed-dose-rate gemcitabine and S-1 with concurrent radiotherapy for locally advanced pancreatic cancer. Cancer Chemother Pharmacol. 2015;76:615–620. doi: 10.1007/s00280-015-2835-3. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
