Predicting prognosis of short survival time after palliative whole-brain radiotherapy
- PMID: 29069502
- PMCID: PMC5778609
- DOI: 10.1093/jrr/rrx058
Predicting prognosis of short survival time after palliative whole-brain radiotherapy
Abstract
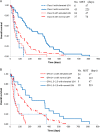
Using existing prognostic models, including the Graded Prognostic Assessment (GPA), it is difficult to identify patients with brain metastases (BMs) who are not likely to survive 2 months after whole-brain radiotherapy (WBRT). The purpose of this study was to identify a subgroup of patients who would not benefit clinically from WBRT. We retrospectively reviewed the records of 111 patients with BMs who were ineligible for surgery or stereotactic irradiation and who underwent WBRT between March 2013 and April 2016. Most patients were scheduled to receive a total dose of 30 Gy in 10 fractions. Non-small cell lung cancer represented the most common primary cancer type (67%), followed by breast cancer (12%). Median survival time (MST) was 109 days (range, 4-883). Univariate analysis identified five factors significantly associated with poor prognosis: performance status (PS) 2-4, perilesional edema, elevated serum lactate dehydrogenase (LDH), using steroids during WBRT, and presence of hepatic metastases. Multivariate analysis confirmed elevated LDH (>300 IU/l) as an independent predictor. MST for LDH >300 IU/l (n = 30) and LDH ≤300 IU/L (n = 87) cohorts were 47 days and 148 days, respectively (P < 0.001). MSTs for GPA 0-1 patients (n = 85) with and without elevated LDH were 37 days and 123 days, respectively (P < 0.001). More than half of the patients with GPA 0-1 and elevated LDH died within two months. Adding elevated LDH to the GPA will permit identification of patients with BMs who have extremely unfavorable prognoses.
Keywords: brain metastases; palliative radiotherapy; prognostic factors; whole-brain radiotherapy.
© The Author 2017. Published by Oxford University Press on behalf of The Japan Radiation Research Society and Japanese Society for Radiation Oncology.
Figures
References
-
- Barnholtz-Sloan JS, Sloan AE, Davis FG et al. Incidence proportions of brain metastases in patients diagnosed (1973 to 2001) in the Metropolitan Detroit Cancer Surveillance System. J Clin Oncol 2004;22:2865–72. - PubMed
-
- Borgelt B, Gelber R, Kramer S et al. The palliation of brain metastases: final results of the first two studies by the Radiation Therapy Oncology Group. Int J Radiat Oncol Biol Phys 1980;6:1–9. - PubMed
-
- Zimm S, Wampler GL, Stablein D et al. Intracerebral metastases in solid-tumor patients: natural history and results of treatment. Cancer 1981;48:384–94. - PubMed
-
- Egawa S, Tukiyama I, Akine Y et al. Radiotherapy of brain metastases. Int J Radiat Oncol Biol Phys 1986;12:1621–5. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

