A Prospective International Multicentre Cohort Study of Intraoperative Heart Rate and Systolic Blood Pressure and Myocardial Injury After Noncardiac Surgery: Results of the VISION Study
- PMID: 29077608
- PMCID: PMC5815500
- DOI: 10.1213/ANE.0000000000002560
A Prospective International Multicentre Cohort Study of Intraoperative Heart Rate and Systolic Blood Pressure and Myocardial Injury After Noncardiac Surgery: Results of the VISION Study
Abstract
Background: The association between intraoperative cardiovascular changes and perioperative myocardial injury has chiefly focused on hypotension during noncardiac surgery. However, the relative influence of blood pressure and heart rate (HR) remains unclear. We investigated both individual and codependent relationships among intraoperative HR, systolic blood pressure (SBP), and myocardial injury after noncardiac surgery (MINS).
Methods: Secondary analysis of the Vascular Events in Noncardiac Surgery Cohort Evaluation (VISION) study, a prospective international cohort study of noncardiac surgical patients. Multivariable logistic regression analysis tested for associations between intraoperative HR and/or SBP and MINS, defined by an elevated serum troponin T adjudicated as due to an ischemic etiology, within 30 days after surgery. Predefined thresholds for intraoperative HR and SBP were: maximum HR >100 beats or minimum HR <55 beats per minute (bpm); maximum SBP >160 mm Hg or minimum SBP <100 mm Hg. Secondary outcomes were myocardial infarction and mortality within 30 days after surgery.
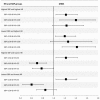
Results: After excluding missing data, 1197 of 15,109 patients (7.9%) sustained MINS, 454 of 16,031 (2.8%) sustained myocardial infarction, and 315 of 16,061 patients (2.0%) died within 30 days after surgery. Maximum intraoperative HR >100 bpm was associated with MINS (odds ratio [OR], 1.27 [1.07-1.50]; P < .01), myocardial infarction (OR, 1.34 [1.05-1.70]; P = .02), and mortality (OR, 2.65 [2.06-3.41]; P < .01). Minimum SBP <100 mm Hg was associated with MINS (OR, 1.21 [1.05-1.39]; P = .01) and mortality (OR, 1.81 [1.39-2.37]; P < .01), but not myocardial infarction (OR, 1.21 [0.98-1.49]; P = .07). Maximum SBP >160 mm Hg was associated with MINS (OR, 1.16 [1.01-1.34]; P = .04) and myocardial infarction (OR, 1.34 [1.09-1.64]; P = .01) but, paradoxically, reduced mortality (OR, 0.76 [0.58-0.99]; P = .04). Minimum HR <55 bpm was associated with reduced MINS (OR, 0.70 [0.59-0.82]; P < .01), myocardial infarction (OR, 0.75 [0.58-0.97]; P = .03), and mortality (OR, 0.58 [0.41-0.81]; P < .01). Minimum SBP <100 mm Hg with maximum HR >100 bpm was more strongly associated with MINS (OR, 1.42 [1.15-1.76]; P < .01) compared with minimum SBP <100 mm Hg alone (OR, 1.20 [1.03-1.40]; P = .02).
Conclusions: Intraoperative tachycardia and hypotension are associated with MINS. Further interventional research targeting HR/blood pressure is needed to define the optimum strategy to reduce MINS.
Conflict of interest statement
Conflicts of Interest: See Disclosures at the end of the article.
Figures



References
-
- Devereaux PJ, Chan MT, Alonso-Coello P; Vascular Events In Noncardiac Surgery Patients Cohort Evaluation Study Investigators. Association between postoperative troponin levels and 30-day mortality among patients undergoing noncardiac surgery. J Am Med Assoc. 2012;307:2295–2304.. - PubMed
-
- Gillies MA, Shah AS, Mullenheim J, et al. Perioperative myocardial injury in patients receiving cardiac output-guided haemodynamic therapy: a substudy of the OPTIMISE Trial. Br J Anaesth. 2015;115:227–233.. - PubMed
-
- Weiser TG, Haynes AB, Molina G, et al. Estimate of the global volume of surgery in 2012: an assessment supporting improved health outcomes. Lancet. 2015;385suppl 2S11. - PubMed
-
- Pearse RM, Moreno RP, Bauer P, et al. ; European Surgical Outcomes Study (EuSOS) group for the Trials groups of the European Society of Intensive Care Medicine and the European Society of Anaesthesiology. Mortality after surgery in Europe: a 7 day cohort study. Lancet. 2012;380:1059–1065.. - PMC - PubMed
-
- Abbott TEF, Fowler AJ, Dobbs TD, Harrison EM, Gillies MA, Pearse RM. Frequency of surgical treatment and related hospital procedures in the UK: a national ecological study using hospital episode statistics. Br J Anaesth. 2017;119:249–257.. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

