Glucocorticosteroid therapy in inflammatory bowel diseases: From clinical practice to molecular biology
- PMID: 29085208
- PMCID: PMC5643284
- DOI: 10.3748/wjg.v23.i36.6628
Glucocorticosteroid therapy in inflammatory bowel diseases: From clinical practice to molecular biology
Abstract
Inflammatory bowel diseases (IBDs), such as ulcerative colitis and Crohn's disease, are chronic pathologies associated with a deregulated immune response in the intestinal mucosa, and they are triggered by environmental factors in genetically susceptible individuals. Exogenous glucocorticoids (GCs) are widely used as anti-inflammatory therapy in IBDs. In the past, patients with moderate or severe states of inflammation received GCs as a first line therapy with an important effectiveness in terms of reduction of the disease activity and the induction of remission. However, this treatment often results in detrimental side effects. This downside drove the development of second generation GCs and more precise (non-systemic) drug-delivery methods. Recent clinical trials show that most of these new treatments have similar effectiveness to first generation GCs with fewer adverse effects. The remaining challenge in successful treatment of IBDs concerns the refractoriness and dependency that some patients encounter during GCs treatment. A deeper understanding of the molecular mechanisms underlying GC response is key to personalizing drug choice for IBDs patients to optimize their response to treatment. In this review, we examine the clinical characteristics of treatment with GCs, followed by an in depth analysis of the proposed molecular mechanisms involved in its resistance and dependence associated with IBDs. This thorough analysis of current clinical and biomedical literature may help guide physicians in determining a course of treatment for IBDs patients and identifies important areas needing further study.
Keywords: Crohn’s disease; Glucocorticoid dependence; Glucocorticoid resistance; Inflammatory bowel diseases; Ulcerative colitis.
Conflict of interest statement
Conflict-of-interest statement: No potential conflicts of interest.
Figures
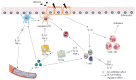
References
-
- Rietdijk ST, D’Haens GR. Recent developments in the treatment of inflammatory bowel disease. J Dig Dis. 2013;14:282–287. - PubMed
-
- De Cassan C, Fiorino G, Danese S. Second-generation corticosteroids for the treatment of Crohn’s disease and ulcerative colitis: more effective and less side effects? Dig Dis. 2012;30:368–375. - PubMed
-
- Molodecky NA, Soon IS, Rabi DM, Ghali WA, Ferris M, Chernoff G, Benchimol EI, Panaccione R, Ghosh S, Barkema HW, et al. Increasing incidence and prevalence of the inflammatory bowel diseases with time, based on systematic review. Gastroenterology. 2012;142:46–54. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

