Portal vein resection and reconstruction with artificial blood vessels is safe and feasible for pancreatic ductal adenocarcinoma patients with portal vein involvement: Chinese center experience
- PMID: 29100433
- PMCID: PMC5652822
- DOI: 10.18632/oncotarget.20847
Portal vein resection and reconstruction with artificial blood vessels is safe and feasible for pancreatic ductal adenocarcinoma patients with portal vein involvement: Chinese center experience
Abstract
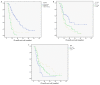
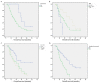
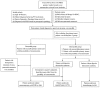
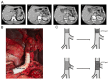
Evidence shows that portal vein resection (PVR) increase the resectability but does little benefit to overall survival in all pancreatic ductal adenocarcinoma (PDAC) patients. But for patients with portal vein involvement, PVR is the only radical choice. But whether the PDAC patients with portal vein involvement would benefit from radical pancreaticoduodenectomy with PVR or not is controversial. All 204 PDAC patients with portal vein involvement were enrolled in this study [PVR group, n=106; surgical bypass (SB) group, n=52; chemotherapy group, n=46]. Overall survival and prognostic factors were analyzed among three groups. Moreover, a literature review of 13 studies were also conducted. Among 3 groups, patients in PVR group achieved a significant longer survival (median survival: PVR group, 22.83 months; SB group, 7.26 months; chemotherapy group, 10.64 months). Therapy choice [hazard ratio (HR) =1.593, 95% confidence interval (CI) 1.323 to 1.918, P<0.001], body mass index (HR=0.772, 95% CI 0.559 to 0.994, P=0.044) and carbohydrateantigen 19-9 (HR=1.325, 95% CI 1.064 to 1.651, P=0.012) were independent prognostic factors which significantly affected overall survival. Pancreaticoduodenectomy combined with PVR and reconstruct with artificial blood vessels is a safe and an appropriate therapy choice for resectable PDAC patients with portal vein involvement.
Keywords: artificial blood vessels; pancreatic ductal adenocarcinoma; pancreaticoduodenectomy; portal vein involvement; portal vein resection.
Conflict of interest statement
CONFLICTS OF INTEREST The authors disclose no conflicts of interest.
Figures
Similar articles
-
Pancreatoduodenectomy with portal vein resection favors the survival time of patients with pancreatic ductal adenocarcinoma: A propensity score matching analysis.Oncol Lett. 2019 Nov;18(5):4563-4572. doi: 10.3892/ol.2019.10822. Epub 2019 Sep 6. Oncol Lett. 2019. PMID: 31611964 Free PMC article.
-
Pancreaticoduodenectomy for ductal adenocarcinoma of the pancreatic head with venous resection.Radiol Oncol. 2016 Jul 19;50(3):321-8. doi: 10.1515/raon-2015-0017. eCollection 2016 Sep 1. Radiol Oncol. 2016. PMID: 27679549 Free PMC article.
-
Portal or superior mesenteric vein resection for pancreatic head adenocarcinoma: prognostic value of the length of venous resection.Surgery. 2009 Apr;145(4):417-25. doi: 10.1016/j.surg.2008.12.009. Epub 2009 Feb 23. Surgery. 2009. PMID: 19303991
-
[Is pancreaticoduodenectomy with portal vein resection indicated in patients with ductal pancreatic carcinoma?].Zentralbl Chir. 1999;124(3):220-5. Zentralbl Chir. 1999. PMID: 10327579 Review. German.
-
Portal vein involvement in pancreatic cancer: a sign of unresectability?Adv Surg. 1997;31:375-94. Adv Surg. 1997. PMID: 9408502 Review.
Cited by
-
A Case of Preserved Blood Flow to the Portal Vein Due to the Concurrent Reconstruction of the Superior Mesenteric Vein and the Splenic Vein Using an Artificial Blood Vessel.Cureus. 2022 Nov 13;14(11):e31457. doi: 10.7759/cureus.31457. eCollection 2022 Nov. Cureus. 2022. PMID: 36523740 Free PMC article.
-
Pancreatoduodenectomy with portal vein resection favors the survival time of patients with pancreatic ductal adenocarcinoma: A propensity score matching analysis.Oncol Lett. 2019 Nov;18(5):4563-4572. doi: 10.3892/ol.2019.10822. Epub 2019 Sep 6. Oncol Lett. 2019. PMID: 31611964 Free PMC article.
-
Laparoscopic pancreatoduodenectomy combined with portal-superior mesenteric vein resection and reconstruction with interposition graft: Case series.Medicine (Baltimore). 2019 Jan;98(3):e14204. doi: 10.1097/MD.0000000000014204. Medicine (Baltimore). 2019. PMID: 30653175 Free PMC article.
-
What to expect with major vascular reconstruction during Whipple procedures: a single institution experience and literature review.J Gastrointest Oncol. 2019 Feb;10(1):95-102. doi: 10.21037/jgo.2018.10.03. J Gastrointest Oncol. 2019. PMID: 30788164 Free PMC article.
-
Recurrence scoring system predicting early recurrence for patients with pancreatic ductal adenocarcinoma undergoing pancreatectomy and portomesenteric vein resection.World J Gastrointest Surg. 2024 Oct 27;16(10):3185-3201. doi: 10.4240/wjgs.v16.i10.3185. World J Gastrointest Surg. 2024. PMID: 39575290 Free PMC article.
References
-
- Siegel R, Ma J, Zou Z, Jemal A. Cancer statistics, 2014. CA Cancer J Clin. 2014;64:9–29. https://doi.org/10.3322/caac.21208 - DOI - PubMed
-
- He J, Chen W. Chinese Cancer Registry Annual Report 2012. Beijing. Press of Military Medical Sciences. 2012:68–71.
-
- Ryan DP, Hong TS, Bardeesy N. Pancreatic adenocarcinoma. N Engl J Med. 2014;371:2140–1. https://doi.org/10.1056/NEJMc1412266 - DOI - PubMed
-
- Zell JA, Rhee JM, Ziogas A, Lipkin SM, Anton-Culver H. Race, socioeconomic status, treatment, and survival time among pancreatic cancer cases in California. Cancer Epidemiol Biomarkers Prev. 2007;16:546–52. https://doi.org/10.1158/1055-9965.EPI-06-0893 - DOI - PubMed
-
- Lau MK, Davila JA, Shaib YH. Incidence and survival of pancreatic head and body and tail cancers: a population-based study in the United States. Pancreas. 2010;39:458–62. https://doi.org/10.1097/MPA.0b013e3181bd6489 - DOI - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

