Trends in diagnostic approaches for pediatric appendicitis: nationwide population-based study
- PMID: 29100501
- PMCID: PMC5670701
- DOI: 10.1186/s12887-017-0940-7
Trends in diagnostic approaches for pediatric appendicitis: nationwide population-based study
Abstract
Background: To define the benefits of different methods for diagnosis of pediatric appendicitis in Taiwan, a nationwide cohort study was used for analysis.
Methods: We identified 44,529 patients under 18 years old who had been hospitalized with a diagnosis of acute appendicitis between 2003 and 2012. We analyzed the percentages of cases in which ultrasound (US) and/or computed tomography (CT) were performed and non-perforated and perforated appendicitis were diagnosed for each year. Multivariate logistic regression analyses were performed to evaluate risk factors for perforated appendicitis.
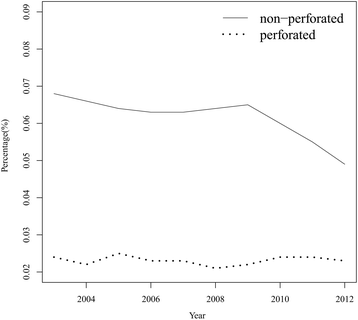
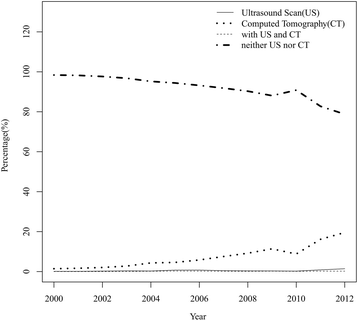
Results: There were more cases of non-perforated appendicitis (N = 32,491) than perforated appendicitis (N = 12,038). The rate of non-perforated cases decreased from 0.068% in 2003 to 0.049% in 2012; perforated cases remained relatively stable at 0.024%~0.023% from 2003 to 2012. The percentage of CT evaluation increased from 3% in 2003 to 20% in 2012; the rates of US or both US and CT evaluations were similar annually. The percentage of neither CT nor US evaluation gradually decreased from 97% in 2003, to 79% in 2012. The odds ratios of a perforated appendix for those patients diagnosed by US, CT, or both US and CT were 1.227 (95% confidence interval (CI) 0.91, 1.65; p = 0.173), 2.744 (95% CI 2.55, 2.95; p < 0.001), and 5.062 (95% CI = 3.14, 8.17; p < 0.001), respectively, compared to patients who did not receive US or CT. The odd ratios of a perforated appendix for those patients 7-12 and ≤6 years old were 1.756 (95% CI 1.67, 1.84; p < 0.001) and 3.094 (95% CI 2.87, 3.34; p < 0.001), respectively, compared to those 13-18 years old.
Conclusions: Our study demonstrated that using CT scan as a diagnostic tool for acute appendicitis increased annually; most patients especially those ≤6 years old who received CT evaluation had a greater risk of having perforated appendicitis. We recommend a prompt appendectomy in those pediatric patients with typical clinical symptoms and physical findings for non-complicated appendicitis to avoid the risk of appendiceal perforation.
Keywords: Appendicitis; Computed tomography; National Health Insurance Database; Ultrasound.
Conflict of interest statement
Ethics approval and consent to participate
The NHI database used in this study consists of anonymous secondary data released to the public for research purposes. This study did not contain confidential patient data. Taipei Medical University-Joint Institutional Review Board approved this study (No: 201,404,074). The patient’s consent to participate is not applicable in this study.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
References
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical