Comparison of two cash transfer strategies to prevent catastrophic costs for poor tuberculosis-affected households in low- and middle-income countries: An economic modelling study
- PMID: 29112693
- PMCID: PMC5675360
- DOI: 10.1371/journal.pmed.1002418
Comparison of two cash transfer strategies to prevent catastrophic costs for poor tuberculosis-affected households in low- and middle-income countries: An economic modelling study
Abstract
Background: Illness-related costs for patients with tuberculosis (TB) ≥20% of pre-illness annual household income predict adverse treatment outcomes and have been termed "catastrophic." Social protection initiatives, including cash transfers, are endorsed to help prevent catastrophic costs. With this aim, cash transfers may either be provided to defray TB-related costs of households with a confirmed TB diagnosis (termed a "TB-specific" approach); or to increase income of households with high TB risk to strengthen their economic resilience (termed a "TB-sensitive" approach). The impact of cash transfers provided with each of these approaches might vary. We undertook an economic modelling study from the patient perspective to compare the potential of these 2 cash transfer approaches to prevent catastrophic costs.
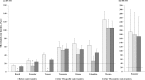
Methods and findings: Model inputs for 7 low- and middle-income countries (Brazil, Colombia, Ecuador, Ghana, Mexico, Tanzania, and Yemen) were retrieved by literature review and included countries' mean patient TB-related costs, mean household income, mean cash transfers, and estimated TB-specific and TB-sensitive target populations. Analyses were completed for drug-susceptible (DS) TB-related costs in all 7 out of 7 countries, and additionally for drug-resistant (DR) TB-related costs in 1 of the 7 countries with available data. All cost data were reported in 2013 international dollars ($). The target population for TB-specific cash transfers was poor households with a confirmed TB diagnosis, and for TB-sensitive cash transfers was poor households already targeted by countries' established poverty-reduction cash transfer programme. Cash transfers offered in countries, unrelated to TB, ranged from $217 to $1,091/year/household. Before cash transfers, DS TB-related costs were catastrophic in 6 out of 7 countries. If cash transfers were provided with a TB-specific approach, alone they would be insufficient to prevent DS TB catastrophic costs in 4 out of 6 countries, and when increased enough to prevent DS TB catastrophic costs would require a budget between $3.8 million (95% CI: $3.8 million-$3.8 million) and $75 million (95% CI: $50 million-$100 million) per country. If instead cash transfers were provided with a TB-sensitive approach, alone they would be insufficient to prevent DS TB-related catastrophic costs in any of the 6 countries, and when increased enough to prevent DS TB catastrophic costs would require a budget between $298 million (95% CI: $219 million-$378 million) and $165,367 million (95% CI: $134,085 million-$196,425 million) per country. DR TB-related costs were catastrophic before and after TB-specific or TB-sensitive cash transfers in 1 out of 1 countries. Sensitivity analyses showed our findings to be robust to imputation of missing TB-related cost components, and use of 10% or 30% instead of 20% as the threshold for measuring catastrophic costs. Key limitations were using national average data and not considering other health and social benefits of cash transfers.
Conclusions: A TB-sensitive cash transfer approach to increase all poor households' income may have broad benefits by reducing poverty, but is unlikely to be as effective or affordable for preventing TB catastrophic costs as a TB-specific cash transfer approach to defray TB-related costs only in poor households with a confirmed TB diagnosis. Preventing DR TB-related catastrophic costs will require considerable additional investment whether a TB-sensitive or a TB-specific cash transfer approach is used.
Conflict of interest statement
I have read the journal's policy and the authors of this manuscript have the following competing interests: CAE is a member of the Editorial Board of
Figures

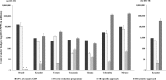
Comment in
-
Measuring success: The challenge of social protection in helping eliminate tuberculosis.PLoS Med. 2017 Nov 7;14(11):e1002419. doi: 10.1371/journal.pmed.1002419. eCollection 2017 Nov. PLoS Med. 2017. PMID: 29112688 Free PMC article.
References
-
- World Health Organization. Global tuberculosis report 2016 [Internet]. 2016 [cited 11 Oct 2017]. Available: http://apps.who.int/iris/bitstream/10665/250441/1/9789241565394-eng.pdf?...
-
- Zhang T, Tang S, Jun G, Whitehead M. Persistent problems of access to appropriate, affordable TB services in rural China: experiences of different socio-economic groups. BMC Public Health. 2007;7: 19 doi: 10.1186/1471-2458-7-19 - DOI - PMC - PubMed
-
- Ukwaja KN, Modebe O, Igwenyi C, Alobu I. The economic burden of tuberculosis care for patients and households in Africa: a systematic review. Int J Tuberc Lung Dis. 2012;16: 733–739. doi: 10.5588/ijtld.11.0193 - DOI - PubMed
-
- Laokri S, Dramaix-Wilmet M, Kassa F, Anagonou S, Dujardin B. Assessing the economic burden of illness for tuberculosis patients in Benin: determinants and consequences of catastrophic health expenditures and inequities. Trop Med Int Health. 2014;19: 1249–1258. doi: 10.1111/tmi.12365 - DOI - PubMed
-
- Lönnroth K, Aung T, Maung W, Kluge H, Uplekar M. Social franchising of TB care through private GPs in Myanmar: an assessment of treatment results, access, equity and financial protection. Health Policy Plan. 2007;22: 156–166. doi: 10.1093/heapol/czm007 - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases

