Microenvironmental regulation of the progression of oral potentially malignant disorders towards malignancy
- PMID: 29113419
- PMCID: PMC5655314
- DOI: 10.18632/oncotarget.20312
Microenvironmental regulation of the progression of oral potentially malignant disorders towards malignancy
Abstract
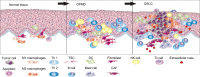
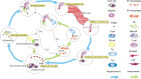
Oral potentially malignant disorders (OPMD) develop in a complex tissue microenvironment where they grow sustainably, acquiring oral squamous cell carcinoma (OSCC) characteristics. The malignant tumor depends on interactions with the surrounding microenvironment to achieve loco-regional invasion and distant metastases. Unlike abnormal cells, the multiple cell types in the tissue microenvironment are relatively stable at the genomic level and, thus, become therapeutic targets with lower risk of resistance, decreasing the risk of OPMD acquiring cancer characteristics and carcinoma recurrence. However, deciding how to disrupt the OPMD and OSCC microenvironments is itself a daunting challenge, since their microenvironments present opposite capacities, resulting in diverse consequences. Furthermore, recent studies revealed that tumor-associated immune cells also participate in the process of differentiation from OPMD to OSCC, suggesting that reeducating stromal cells may be a new strategy to prevent OPMD from acquiring OSCC characteristics and to treat OSCC. In this review, we discuss the characteristics of the microenvironment of OPMD and OSCC as well as new therapeutic strategies.
Keywords: immunity; microenvironment; oral potentially malignant disorder; premalignant condition; therapeutics.
Conflict of interest statement
CONFLICTS OF INTEREST The authors declare no conflicts of interest.
Figures


Similar articles
-
A comparative study of Candida species diversity among patients with oral squamous cell carcinoma and oral potentially malignant disorders.BMC Res Notes. 2020 Oct 20;13(1):488. doi: 10.1186/s13104-020-05336-3. BMC Res Notes. 2020. PMID: 33081839 Free PMC article.
-
Comparison of PD-L1 Expression in Oral Squamous Cell Carcinoma and Premalignant Lesions of Oral Cavity.Asian Pac J Cancer Prev. 2022 Dec 1;23(12):4039-4045. doi: 10.31557/APJCP.2022.23.12.4039. Asian Pac J Cancer Prev. 2022. PMID: 36579984 Free PMC article.
-
Is autoimmunity associated with the development of premalignant oral conditions and the progression to oral squamous cell carcinoma?: A literature review.J Stomatol Oral Maxillofac Surg. 2024 Nov 17;126(5):102139. doi: 10.1016/j.jormas.2024.102139. Online ahead of print. J Stomatol Oral Maxillofac Surg. 2024. PMID: 39561876
-
Extracellular Vesicles in Oral Squamous Cell Carcinoma and Oral Potentially Malignant Disorders: A Systematic Review.Int J Mol Sci. 2020 Feb 11;21(4):1197. doi: 10.3390/ijms21041197. Int J Mol Sci. 2020. PMID: 32054041 Free PMC article.
-
Unmet Needs and Perspectives in Oral Cancer Prevention.Cancers (Basel). 2022 Apr 2;14(7):1815. doi: 10.3390/cancers14071815. Cancers (Basel). 2022. PMID: 35406587 Free PMC article. Review.
Cited by
-
Microenvironment in Oral Potentially Malignant Disorders: Multi-Dimensional Characteristics and Mechanisms of Carcinogenesis.Int J Mol Sci. 2022 Aug 11;23(16):8940. doi: 10.3390/ijms23168940. Int J Mol Sci. 2022. PMID: 36012205 Free PMC article. Review.
-
Evaluation of Mast Cells in Oral Potentially Malignant Disorders and Oral Squamous Cell Carcinoma.Int J Dent. 2021 Aug 27;2021:5609563. doi: 10.1155/2021/5609563. eCollection 2021. Int J Dent. 2021. PMID: 34490052 Free PMC article.
-
Knowledge About the Importance of Early Diagnosis and Treatment of Oral Potentially Malignant Disorders Among the South Indian Population: An Institutional Retrospective Study.Cureus. 2024 Apr 6;16(4):e57740. doi: 10.7759/cureus.57740. eCollection 2024 Apr. Cureus. 2024. PMID: 38716030 Free PMC article.
-
Mechanism of tumour microenvironment in the progression and development of oral cancer.Mol Biol Rep. 2021 Feb;48(2):1773-1786. doi: 10.1007/s11033-020-06054-6. Epub 2021 Jan 25. Mol Biol Rep. 2021. PMID: 33492572 Review.
-
The Effect of Oral Potentially Malignant Disorders (OPMD) on Dental Implants Survival-A Systematic Review.Dent J (Basel). 2025 Jan 15;13(1):35. doi: 10.3390/dj13010035. Dent J (Basel). 2025. PMID: 39851611 Free PMC article. Review.
References
-
- Mantovani A, Allavena P, Sica A, Balkwill F. Cancer-related inflammation. Nature. 2008;454:436–444. - PubMed
-
- Noone RB, Bonner H, Jr, Raymond S, Brown AS, Graham WP, 3rd, Lehr HB. Lymph node metastases in oral carcinoma. A correlation of histopathology with survival. Plast Reconstr Surg. 1974;53:158–166. - PubMed
-
- Warnakulasuriya S, Johnson NW, van der Waal I. Nomenclature and classification of potentially malignant disorders of the oral mucosa. J Oral Pathol Med. 2007;36:575–580. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

