Topical insulin accelerates cutaneous wound healing in insulin-resistant diabetic rats
- PMID: 29118927
- PMCID: PMC5666074
Topical insulin accelerates cutaneous wound healing in insulin-resistant diabetic rats
Abstract
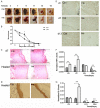
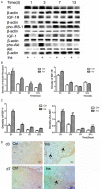
Insulin signaling defects could lead to insulin resistance in insulin target organs: typically, in the muscler, liver, and adipose tissue. We have observed that insulin accelerated diabetic wound healing in our previous works; to further elucidate the mechanism, we investigated the expression and activation of insulin and insulin-like growth factor (IGF)-1 signaling, compared insulin sensitivity in skin tissue with that in liver tissue, and also observed the regulation of insulin on inflammatory response of wounds during the healing process. We found lower expression of insulin receptor, phos-AKT, IGF-1 in type II diabetic rat skin compared with that in normal rat skin. However, the level of phos-AKT in diabetic rat skin remarkably increased after systemic insulin injection, whereas no significant change of phos-AKT was observed in liver upon insulin stimulation. In insulin-treated wounds, we detected a significant increase in insulin signaling proteins and growth factor, as well as the phosphorylated insulin receptor substrate-1 and AKT. The increased Glut1 protein level and translocation of Glut1 from cytosol to cell membrane of the basal epidermal cells were also observed after insulin application. Insulin-treated wounds showed advanced infiltration and resolution of macrophages and a change pattern similar to that of inflammatory mediators, including TNF-α and IL-6. Our findings support that insulin is a valid agent for diabetic wound healing because of its effect on ameliorating defective insulin action and regulating inflammation response. Our results indicate the presence of subtle insulin responsiveness in diabetic skin tissue, regardless of the presence of impaired insulin sensitivity, which could be the cellular and molecular mechanism of insulin accelerating diabetic wound healing.
Keywords: Diabetic; insulin; insulin resistance; wound healing.
Conflict of interest statement
None.
Figures


References
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous
