Primary vs Secondary Endoscopic Dacryocystorhinostomy for Acute Dacryocystitis With Lacrimal Sac Abscess Formation: A Randomized Clinical Trial
- PMID: 29121183
- PMCID: PMC6583760
- DOI: 10.1001/jamaophthalmol.2017.4798
Primary vs Secondary Endoscopic Dacryocystorhinostomy for Acute Dacryocystitis With Lacrimal Sac Abscess Formation: A Randomized Clinical Trial
Abstract
Importance: Endoscopic dacryocystorhinostomy (EN-DCR) is emerging as the preferred procedure in the management of nasolacrimal duct obstructions. However, its safety and long-term efficacy in the setting of acute dacryocystitis with lacrimal sac abscess have not been well studied.
Objective: To compare outcomes of EN-DCR as primary treatment with EN-DCR as a secondary treatment after percutaneous drainage of lacrimal sac abscess in acute dacryocystitis.
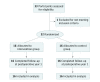
Design, setting, and participants: This randomized clinical trial was conducted from October 1, 2012, to October 31, 2015, at a tertiary ophthalmic center. The assessors of success at postoperative year 1 were masked to the procedures received by the participants. All surgical procedures were performed by 2 oculoplastic surgeons with different levels of EN-DCR experience. Eligible participants had acute dacryocystitis and lacrimal sac abscess presenting within 2 weeks of onset, who were 18 to 90 years of age. Analysis was of the intention-to-treat population.
Interventions: Patients were allocated by block randomization to receive either percutaneous drainage of lacrimal sac abscess followed by EN-DCR after the acute episode subsided (control group) or primary EN-DCR within 2 weeks of presentation (intervention group). Both groups received a course of empirical systemic antibiotics (amoxicillin and clavulanic acid, 375 mg, to be taken 3 times a day for 1 week).
Main outcomes and measures: Primary outcomes were time from presentation to documentation of symptom resolution and recurrence within 3 months.
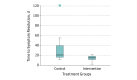
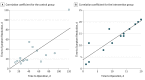
Results: Thirty-two patients were randomized equally into 2 treatment arms (control and intervention). The mean (SD) age of patients was 61 (13) years, and there was a predominance of women (27 [84%]). The mean (SD) time to symptom resolution was 13.8 (5.8) days in the intervention group compared with 31.7 (27.1) days in the control group (mean difference, 17.9; 95% CI, 3.71-32.01; P = .02). The mean (SD) time to surgery in the intervention group was shorter at 11.9 (6.3) days compared with 45.6 (30.1) days in the control group (mean difference, 33.6; 95% CI, 17.92-49.33; P < .001). Recurrences occurred once in the control group and did not occur in the intervention group. No differences in operation time and complications between the 2 groups were identified. The anatomical and functional success was 87.5% (14 of 16 cases) in both groups at postoperative year 1.
Conclusions and relevance: Primary EN-DCR in acute dacryocystitis with lacrimal sac abscess results in faster resolution compared with secondary treatment. No differences in recurrence, safety, or outcomes at postoperative year 1 were noted between the 2 treatment groups.
Conflict of interest statement
Figures
Similar articles
-
Primary Powered Endoscopic Dacryocystorhinostomy in the Setting of Acute Dacryocystitis and Lacrimal Abscess.Ophthalmic Plast Reconstr Surg. 2015 Jul-Aug;31(4):293-5. doi: 10.1097/IOP.0000000000000309. Ophthalmic Plast Reconstr Surg. 2015. PMID: 25226100
-
Primary treatment of acute dacryocystitis by endoscopic dacryocystorhinostomy with silicone intubation guided by a soft probe.Ophthalmology. 2009 Jan;116(1):116-22. doi: 10.1016/j.ophtha.2008.09.041. Ophthalmology. 2009. PMID: 19118702 Clinical Trial.
-
Acquired fistula of the lacrimal sac and laisser-faire approach. Description of the natural history of acquired fistulas between the lacrimal sac and the skin occurring before planned endonasal dacryocystorhinostomy (DCR) and without any treatment of the fistula.J Fr Ophtalmol. 2016 Oct;39(8):687-690. doi: 10.1016/j.jfo.2016.03.009. Epub 2016 Aug 29. J Fr Ophtalmol. 2016. PMID: 27587346
-
An update on endoscopic mechanical and powered dacryocystorhinostomy in acute dacryocystitis and lacrimal abscess.Ann Anat. 2020 Jan;227:151408. doi: 10.1016/j.aanat.2019.07.009. Epub 2019 Aug 26. Ann Anat. 2020. PMID: 31465822 Review.
-
Evidence-based review of surgical practices in endoscopic endonasal dacryocystorhinostomy for primary acquired nasolacrimal duct obstruction and other new indications.Curr Opin Ophthalmol. 2014 Sep;25(5):443-8. doi: 10.1097/ICU.0000000000000084. Curr Opin Ophthalmol. 2014. PMID: 24979582 Review.
Cited by
-
A case report of exophytic nasal papilloma with acute dacryocystitis as the first symptom.BMC Ophthalmol. 2021 Dec 29;21(1):458. doi: 10.1186/s12886-021-02223-8. BMC Ophthalmol. 2021. PMID: 34965868 Free PMC article.
-
Surgical outcomes in acute dacryocystitis patients undergoing endonasal endoscopic dacryocystorhinostomy with or without silicone tube intubation.Int J Ophthalmol. 2021 Jun 18;14(6):844-848. doi: 10.18240/ijo.2021.06.08. eCollection 2021. Int J Ophthalmol. 2021. PMID: 34150538 Free PMC article.
-
Update on lacrimal apparatus dysfunction associated with differentiated thyroid cancer after I-131 therapy.Int Ophthalmol. 2024 Jun 23;44(1):257. doi: 10.1007/s10792-024-03192-9. Int Ophthalmol. 2024. PMID: 38909080 Review.
-
Endoscopy in the field of oculo-facial plastic surgery.J Curr Ophthalmol. 2018 May 18;30(2):99-101. doi: 10.1016/j.joco.2018.04.005. eCollection 2018 Jun. J Curr Ophthalmol. 2018. PMID: 29988945 Free PMC article. No abstract available.
-
Outcome of transcanalicular laser dacryocystorhinostomy with endonasal augmentation in acute versus post-acute dacryocystitis.Eye (Lond). 2023 Apr;37(6):1225-1230. doi: 10.1038/s41433-022-02104-4. Epub 2022 May 19. Eye (Lond). 2023. PMID: 35590102 Free PMC article. Clinical Trial.
References
-
- Bharathi MJ, Ramakrishnan R, Maneksha V, Shivakumar C, Nithya V, Mittal S. Comparative bacteriology of acute and chronic dacryocystitis. Eye (Lond). 2008;22(7):953-960. - PubMed
-
- Mills DM, Bodman MG, Meyer DR, Morton AD III; ASOPRS Dacryocystitis Study Group . The microbiologic spectrum of dacryocystitis: a national study of acute versus chronic infection. Ophthal Plast Reconstr Surg. 2007;23(4):302-306. - PubMed
-
- Cahill KV, Burns JA. Management of acute dacryocystitis in adults. Ophthal Plast Reconstr Surg. 1993;9(1):38-41. - PubMed
-
- Burns JA, Cahill KV. Modified Kinosian dacryocystorhinostomy: a review of 122 cases. Ophthalmic Surg. 1985;16(11):710-716. - PubMed
-
- Ali MJ, Joshi SD, Naik MN, Honavar SG. Clinical profile and management outcome of acute dacryocystitis: two decades of experience in a tertiary eye care center. Semin Ophthalmol. 2015;30(2):118-123. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

