Impaired contractile function of the supraspinatus in the acute period following a rotator cuff tear
- PMID: 29121906
- PMCID: PMC5679320
- DOI: 10.1186/s12891-017-1789-5
Impaired contractile function of the supraspinatus in the acute period following a rotator cuff tear
Abstract
Background: Rotator cuff (RTC) tears are a common clinical problem resulting in adverse changes to the muscle, but there is limited information comparing histopathology to contractile function. This study assessed supraspinatus force and susceptibility to injury in the rat model of RTC tear, and compared these functional changes to histopathology of the muscle.
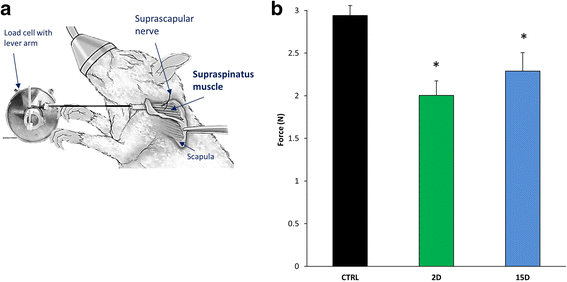
Methods: Unilateral RTC tears were induced in male rats via tenotomy of the supraspinatus and infraspinatus. Maximal tetanic force and susceptibility to injury of the supraspinatus muscle were measured in vivo at day 2 and day 15 after tenotomy. Supraspinatus muscles were weighed and harvested for histologic analysis of the neuromuscular junction (NMJ), intramuscular lipid, and collagen.
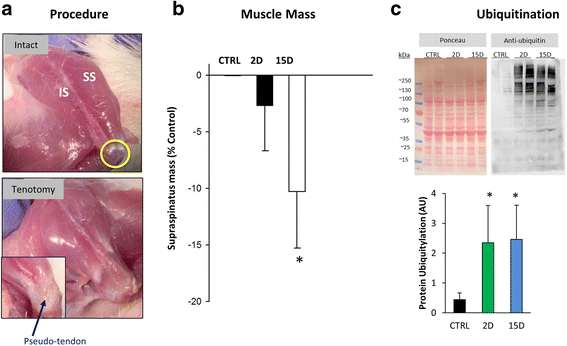
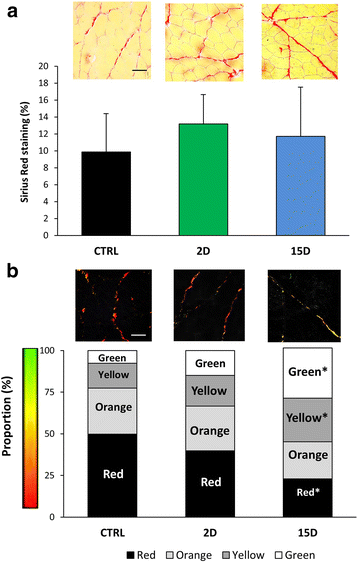
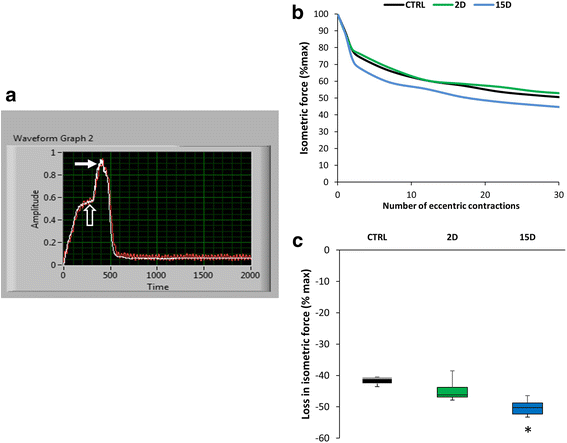
Results: Tenotomy resulted in eventual atrophy and weakness. Despite no loss in muscle mass at day 2 there was a 30% reduction in contractile force, and a decrease in NMJ continuity and size. Reduced force persisted at day 15, a time point when muscle atrophy was evident but NMJ morphology was restored. At day 15, torn muscles had decreased collagen-packing density and were also more susceptible to contraction-induced injury.
Conclusion: Muscle size and histopathology are not direct indicators of overall RTC contractile health. Changes in NMJ morphology and collagen organization were associated with changes in contractile function and thus may play a role in response to injury. Although our findings are limited to the acute phase after a RTC tear, the most salient finding is that RTC tenotomy results in increased susceptibility to injury of the supraspinatus.
Keywords: Collagen organization; Contractility; Eccentric injury; Muscle force; Neuromuscular junction; Rat.
Conflict of interest statement
Ethics approval and consent to participate
As noted in the text, all protocols were approved by the University of Maryland Institutional Animal Care & Use Committee.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures


Similar articles
-
Fatty Infiltration Is a Prognostic Marker of Muscle Function After Rotator Cuff Tear.Am J Sports Med. 2018 Jul;46(9):2161-2169. doi: 10.1177/0363546518769267. Epub 2018 May 11. Am J Sports Med. 2018. PMID: 29750541 Free PMC article.
-
Lateral to medial fibro-adipogenic degeneration are greater in infraspinatus than supraspinatus following nerve and tendon injury of murine rotator cuff.J Orthop Res. 2021 Jan;39(1):184-195. doi: 10.1002/jor.24847. Epub 2020 Sep 14. J Orthop Res. 2021. PMID: 32886404
-
A method to test contractility of the supraspinatus muscle in mouse, rat, and rabbit.J Appl Physiol (1985). 2016 Feb 1;120(3):310-7. doi: 10.1152/japplphysiol.00788.2015. Epub 2015 Nov 19. J Appl Physiol (1985). 2016. PMID: 26586911 Free PMC article.
-
Histopathology of rotator cuff tears.Sports Med Arthrosc Rev. 2011 Sep;19(3):227-36. doi: 10.1097/JSA.0b013e318213bccb. Sports Med Arthrosc Rev. 2011. PMID: 21822106 Review.
-
The role of mechanobiology in progression of rotator cuff muscle atrophy and degeneration.J Orthop Res. 2018 Feb;36(2):546-556. doi: 10.1002/jor.23662. Epub 2017 Aug 11. J Orthop Res. 2018. PMID: 28755470 Free PMC article. Review.
Cited by
-
Rotator cuff tears.Nat Rev Dis Primers. 2024 Feb 8;10(1):8. doi: 10.1038/s41572-024-00492-3. Nat Rev Dis Primers. 2024. PMID: 38332156 Review.
-
Tenotomy-induced muscle atrophy is sex-specific and independent of NFκB.Elife. 2022 Dec 12;11:e82016. doi: 10.7554/eLife.82016. Elife. 2022. PMID: 36508247 Free PMC article.
-
MiR-21 regulates skeletal muscle atrophy and fibrosis by targeting TGF-beta/SMAD7-SMAD2/3 signaling pathway.Heliyon. 2024 Jun 19;10(12):e33062. doi: 10.1016/j.heliyon.2024.e33062. eCollection 2024 Jun 30. Heliyon. 2024. PMID: 39027432 Free PMC article.
-
Biotoxins in muscle regeneration research.J Muscle Res Cell Motil. 2019 Dec;40(3-4):291-297. doi: 10.1007/s10974-019-09548-4. Epub 2019 Jul 29. J Muscle Res Cell Motil. 2019. PMID: 31359301 Review.
-
Geometric modeling predicts architectural adaptations are not responsible for the force deficit following tenotomy in the rotator cuff.J Biomech. 2022 Jun;138:111105. doi: 10.1016/j.jbiomech.2022.111105. Epub 2022 Apr 28. J Biomech. 2022. PMID: 35504146 Free PMC article.
References
MeSH terms
Substances
Grants and funding
- AR07592-20/National Institute of Arthritis and Musculoskeletal and Skin Diseases
- R44 AG026815/AG/NIA NIH HHS/United States
- T32 AR007592/AR/NIAMS NIH HHS/United States
- T32AG00026815S1/National Heart, Lung, and Blood Institute
- R01-AR059179/National Institute of Arthritis and Musculoskeletal and Skin Diseases
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

