A comparison of postoperative morphometric and hemodynamic changes between saphenous vein and left internal mammary artery grafts
- PMID: 29122958
- PMCID: PMC5688779
- DOI: 10.14814/phy2.13487
A comparison of postoperative morphometric and hemodynamic changes between saphenous vein and left internal mammary artery grafts
Abstract
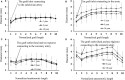
There is higher long-term failure of the saphenous vein graft (SVG) compared with the left internal mammary artery (LIMA) graft, which is affected by the hemodynamic environment. A comprehensive analysis of postoperative structure-function changes is important to study the atherogenesis in the SVG A comparison of morphometric and hemodynamic parameters was carried out between LIMA grafts and SVGs and between different time points postoperatively. Various parameters were obtained from the image reconstruction and flow simulation in patients, who underwent CT exams for ~1 year, 5 and 10 years after revascularization. Morphometric data showed a decrease in lumen size in the entire SVG and anastomosis of different patients in a sequence of ~1 year, 5 and 10 years postoperatively despite negligible changes of LIMA size. Computational results indicated the fourfold increased surface area ratio (SAR) of low time-averaged wall shear stress (TAWSS) in the SVG and anastomosis at postoperative 10 years than that at postoperative ~1 year. The SAR of high TAWSS gradient (TAWSSG) at the distal anastomosis between SVG and coronary arteries was significantly higher (14 ± 9% vs. 6 ± 8%) than that in the LIMA group at postoperative ~1 year. There were strong correlations between morphometric and hemodynamic parameters in the SVG and distal anastomosis at various time points postoperatively, which showed deterioration relevant to persistent diffuse diseases at postoperative ~10 years.
Keywords: CABG; LIMA; SVG; flow simulation; hemodynamics.
© 2017 The Authors. Physiological Reports published by Wiley Periodicals, Inc. on behalf of The Physiological Society and the American Physiological Society.
Figures




Similar articles
-
Hemodynamics of left internal mammary artery bypass graft: Effect of anastomotic geometry, coronary artery stenosis, and postoperative time.J Biomech. 2016 Mar 21;49(5):645-652. doi: 10.1016/j.jbiomech.2016.01.031. Epub 2016 Feb 8. J Biomech. 2016. PMID: 26900034
-
Use of the right internal mammary artery and the great saphenous vein for left anterior descending artery revascularization in patients whose left internal mammal artery cannot be used: a study based on transit-time flow measurement.J Cardiothorac Surg. 2020 Jun 5;15(1):126. doi: 10.1186/s13019-020-01172-5. J Cardiothorac Surg. 2020. PMID: 32503570 Free PMC article.
-
21-Year Survival of Left Internal Mammary Artery-Radial Artery-Y Graft.J Am Coll Cardiol. 2018 Sep 18;72(12):1332-1340. doi: 10.1016/j.jacc.2018.06.064. J Am Coll Cardiol. 2018. PMID: 30213324
-
Patency of conduits in patients who received internal mammary artery, radial artery and saphenous vein grafts.BMC Cardiovasc Disord. 2020 Mar 24;20(1):148. doi: 10.1186/s12872-020-01433-0. BMC Cardiovasc Disord. 2020. PMID: 32204693 Free PMC article.
-
Comparison of fractional flow reserve of composite Y-grafts with saphenous vein or right internal thoracic arteries.J Thorac Cardiovasc Surg. 2010 Sep;140(3):639-45. doi: 10.1016/j.jtcvs.2009.11.013. Epub 2010 Feb 18. J Thorac Cardiovasc Surg. 2010. PMID: 20167333
Cited by
-
Determination of the Frequency of Right and Left Internal Mammary Artery Embolization in Single Ventricle Patients: A Two-Center Study.Pediatr Cardiol. 2018 Dec;39(8):1657-1662. doi: 10.1007/s00246-018-1946-0. Epub 2018 Aug 13. Pediatr Cardiol. 2018. PMID: 30105467
-
Morphometric and hemodynamic parameter dataset for coronary artery aneurysms caused by atherosclerosis.Data Brief. 2019 Jul 19;25:104293. doi: 10.1016/j.dib.2019.104293. eCollection 2019 Aug. Data Brief. 2019. PMID: 31388526 Free PMC article.
-
Author`s Reply.Anatol J Cardiol. 2019 Feb;21(2):116-117. Anatol J Cardiol. 2019. PMID: 30694807 Free PMC article. No abstract available.
-
Low Wall Shear Stress Is Associated with Saphenous Vein Graft Stenosis in Patients with Coronary Artery Bypass Grafting.J Cardiovasc Transl Res. 2021 Aug;14(4):770-781. doi: 10.1007/s12265-020-09982-7. Epub 2020 Apr 2. J Cardiovasc Transl Res. 2021. PMID: 32240496 Free PMC article.
-
Reducing vasospasm of vein and arterial conduits used in coronary artery bypass surgery: are solutions the solution or is preserved perivascular fat the answer?Front Physiol. 2025 Jan 31;16:1539102. doi: 10.3389/fphys.2025.1539102. eCollection 2025. Front Physiol. 2025. PMID: 39958693 Free PMC article. Review.
References
-
- Bassiouny, H. S. , White S., Glagov S., Choi E., Giddens D. P., and Zarins C. K.. 1992. Anastomotic intimal hyperplasia: mechanical injury or flow induced. J. Vasc. Surg. 15:708–716; discussion 716‐707. - PubMed
-
- Berger, A. , MacCarthy P.A., Siebert U., Carlier S., Wijns W., Heyndrickx G., et al. 2004. Long‐term patency of internal mammary artery bypass grafts: relationship with preoperative severity of the native coronary artery stenosis. Circulation 110:II36–II40. - PubMed
-
- Campeau, L. , Enjalbert M., Lesperance J., Vaislic C., Grondin C. M., and Bourassa M. G.. 1983. Atherosclerosis and late closure of aortocoronary saphenous vein grafts: sequential angiographic studies at 2 weeks, 1 year, 5 to 7 years, and 10 to 12 years after surgery. Circulation 68:II1–II7. - PubMed
-
- Canver, C. C. 1995. Conduit options in coronary artery bypass surgery. Chest 108:1150–1155. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

