Metabolomics and Gene Expression Analysis Reveal Down-regulation of the Citric Acid (TCA) Cycle in Non-diabetic CKD Patients
- PMID: 29128444
- PMCID: PMC5832558
- DOI: 10.1016/j.ebiom.2017.10.027
Metabolomics and Gene Expression Analysis Reveal Down-regulation of the Citric Acid (TCA) Cycle in Non-diabetic CKD Patients
Abstract
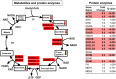
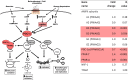
Chronic kidney disease (CKD) is a public health problem with very high prevalence and mortality. Yet, there is a paucity of effective treatment options, partly due to insufficient knowledge of underlying pathophysiology. We combined metabolomics (GCMS) with kidney gene expression studies to identify metabolic pathways that are altered in adults with non-diabetic stage 3-4 CKD versus healthy adults. Urinary excretion rate of 27 metabolites and plasma concentration of 33 metabolites differed significantly in CKD patients versus controls (estimate range-68% to +113%). Pathway analysis revealed that the citric acid cycle was the most significantly affected, with urinary excretion of citrate, cis-aconitate, isocitrate, 2-oxoglutarate and succinate reduced by 40-68%. Reduction of the citric acid cycle metabolites in urine was replicated in an independent cohort. Expression of genes regulating aconitate, isocitrate, 2-oxoglutarate and succinate were significantly reduced in kidney biopsies. We observed increased urine citrate excretion (+74%, p=0.00009) and plasma 2-oxoglutarate concentrations (+12%, p=0.002) in CKD patients during treatment with a vitamin-D receptor agonist in a randomized trial. In conclusion, urinary excretion of citric acid cycle metabolites and renal expression of genes regulating these metabolites were reduced in non-diabetic CKD. This supports the emerging view of CKD as a state of mitochondrial dysfunction.
Keywords: Chronic kidney disease; Citric acid cycle; Gene expression; Metabolomics; Mitochondria.
Copyright © 2017 The Authors. Published by Elsevier B.V. All rights reserved.
Figures

Comment in
-
Impaired Citric Acid Cycle in Nondiabetic Chronic Kidney Disease.EBioMedicine. 2017 Dec;26:6-7. doi: 10.1016/j.ebiom.2017.11.006. Epub 2017 Nov 14. EBioMedicine. 2017. PMID: 29157838 Free PMC article. No abstract available.
References
-
- Agarwal R., Hynson J.E., Hecht T.J., Light R.P., Sinha A.D. Short-term vitamin D receptor activation increases serum creatinine due to increased production with no effect on the glomerular filtration rate. Kidney Int. 2011;80:1073–1079. - PubMed
-
- Bashir S., Khan N.A., Gilani A.-H. Physiology of Renal Handling of Citrate. In: Talati J.J., Tiselius H.-G., Albala D.M., Ye Z., editors. Urolithiasis: Basic Science and Clinical Practice. Springer London; London: 2012. pp. 183–186.
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

