Posterior shoulder dislocation with associated reverse Hill-Sachs lesion: treatment options and functional outcome after a 5-year follow up
- PMID: 29132328
- PMCID: PMC5683370
- DOI: 10.1186/s12891-017-1808-6
Posterior shoulder dislocation with associated reverse Hill-Sachs lesion: treatment options and functional outcome after a 5-year follow up
Abstract
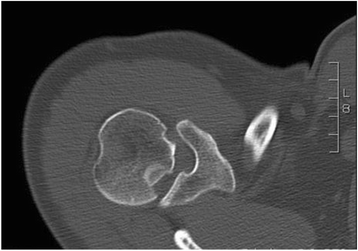
Background: The current study describes several surgical techniques for the treatment of the reverse Hill - Sachs lesion after posterior shoulder dislocation; we also aimed to present long term results followed for a minimum of five years.
Methods: This study is a prospective case series of 17 patients who were treated in our clinic between 2008 and 2011. Patients with a defect size smaller than 25% of the articular surface were treated conservatively. An endoprosthesis of the glenohumeral joint was implanted in patients with a defect size bigger than 40%. All remaining patients were treated by a variety of operative techniques, depending on the quality of the bone and size of the defect.
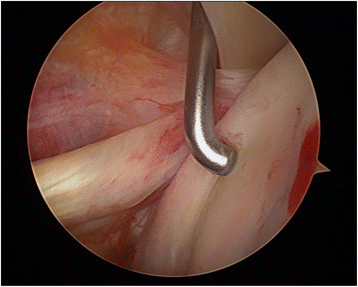
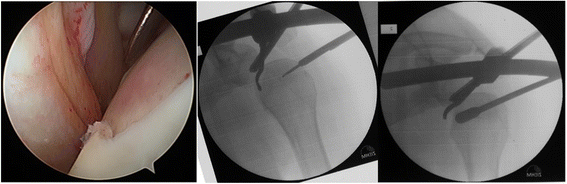
Results: Twelve of seventeen patients had a defect size of the humeral articular surface between 25% and 40% with a mean age of 39 years. Depending on the defect size these patients were treated with retrograde chondral elevation, antegrade cylindrical graft or a graft of the iliac bone crest with an open approach. All the procedures showed fair results, e.g. the open approach with a graft of the iliac bone crest (2010: Dash 3.89, Constant 90.33, Rowe 86.67; 2015: Dash 2.22, Constant 92.00, Rowe 93.33).
Conclusion: The open approach is not a disadvantage for the functional outcome. The treatment algorithm should involve the superficial size of the defect as well as the depth of the defect and the time interval between the dislocation and the surgical treatment.
Trial registration: 223/2012BO2 , 02 August 2010.
Keywords: Defect size; Osteosynthesis; Outcome; Posterior shoulder dislocation.
Conflict of interest statement
Ethics approval and consent to participate
Informed written consent was obtained from all individual participants included in the study. The study was conducted according to the Helsinki Declaration (Ethical Principles for Medical Research Involving Human Subjects) and was approved by the University of Tuebingen ethics committee.
Consent for publication
Not Applicable
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures




Similar articles
-
Posterior shoulder dislocation with associated reverse Hill-Sachs lesion: clinical outcome 10 years after joint-preserving surgery.Arch Orthop Trauma Surg. 2023 May;143(5):2503-2507. doi: 10.1007/s00402-022-04482-6. Epub 2022 Jun 3. Arch Orthop Trauma Surg. 2023. PMID: 35657414 Free PMC article.
-
The epidemiology, risk of recurrence, and functional outcome after an acute traumatic posterior dislocation of the shoulder.J Bone Joint Surg Am. 2011 Sep 7;93(17):1605-13. doi: 10.2106/JBJS.J.00973. J Bone Joint Surg Am. 2011. PMID: 21915575
-
Anatomical and functional results after arthroscopic Hill-Sachs remplissage.J Bone Joint Surg Am. 2012 Apr 4;94(7):618-26. doi: 10.2106/JBJS.K.00101. J Bone Joint Surg Am. 2012. PMID: 22488618
-
Iliac bone-block autograft for posterior shoulder instability.Orthop Traumatol Surg Res. 2009 Apr;95(2):100-7. doi: 10.1016/j.otsr.2008.09.008. Epub 2009 Mar 21. Orthop Traumatol Surg Res. 2009. PMID: 19332402 Review.
-
Posterior shoulder fracture-dislocation: an update with treatment algorithm.Eur J Orthop Surg Traumatol. 2017 Apr;27(3):285-294. doi: 10.1007/s00590-016-1840-5. Epub 2016 Aug 25. Eur J Orthop Surg Traumatol. 2017. PMID: 27562590 Review.
Cited by
-
Posterior Shoulder Dislocation with Engaging Reverse Hill-Sachs Lesion: A Retrospective Study of Ten Patients Treated with Arthroscopy or Open Reduction and Stabilization.J Clin Med. 2021 Apr 1;10(7):1410. doi: 10.3390/jcm10071410. J Clin Med. 2021. PMID: 33915791 Free PMC article.
-
Evolving concepts in the treatment of posterior shoulder instability with glenohumeral bone loss.Ann Jt. 2024 Jul 12;9:28. doi: 10.21037/aoj-23-45. eCollection 2024. Ann Jt. 2024. PMID: 39114415 Free PMC article. Review.
-
Posterior Glenohumeral Capsular Reconstruction With Modified McLaughlin for Chronic Locked Posterior Dislocation.Arthrosc Tech. 2019 Nov 22;8(12):e1543-e1550. doi: 10.1016/j.eats.2019.08.004. eCollection 2019 Dec. Arthrosc Tech. 2019. PMID: 31890535 Free PMC article.
-
Chronic locked posterior gleno-humeral dislocation: technical note on fibular grafting for restoration of humeral head sphericity.J Orthop Surg Res. 2021 Nov 18;16(1):683. doi: 10.1186/s13018-021-02835-2. J Orthop Surg Res. 2021. PMID: 34794483 Free PMC article.
-
The duration of dislocation is the most important prognostic factor in chronic locked posterior shoulder dislocations treated with the modified McLaughlin surgical procedure: a multicentre study.BMC Musculoskelet Disord. 2025 Jul 4;26(1):635. doi: 10.1186/s12891-025-08886-4. BMC Musculoskelet Disord. 2025. PMID: 40616041 Free PMC article.
References
-
- Hatzis N, Kaar TK, Wirth MA, Rockwood CA., Jr The often overlooked posterior dislocation of the shoulder. Tex Med. 2001;97(11):62–67. - PubMed
-
- Hawkins RJ, Neer CS, 2nd, Pianta RM, Mendoza FX. Locked posterior dislocation of the shoulder. J Bone Joint Surg Am 1987;69(1):9–18. - PubMed
-
- Mc LH. Posterior dislocation of the shoulder. J Bone Joint Surg Am. 1952;24(3):584–590. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

