Magnetic resonance elastography: beyond liver fibrosis-a case-based pictorial review
- PMID: 29143076
- PMCID: PMC6731769
- DOI: 10.1007/s00261-017-1383-1
Magnetic resonance elastography: beyond liver fibrosis-a case-based pictorial review
Abstract
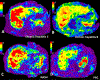
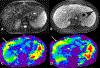
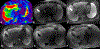
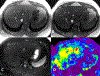
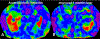
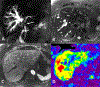
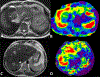
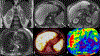
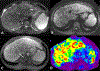
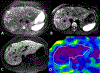
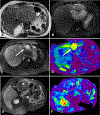
Magnetic resonance elastography (MRE) has been introduced for clinical evaluation of liver fibrosis for nearly a decade. MRE has proven to be a robust and accurate technique for diagnosis and staging of liver fibrosis. As clinical experience with MRE grows, the possible role in evaluation of other diffuse and focal disorders of liver is emerging. Stiffness maps provide an opportunity to evaluate mechanical properties within a large volume of liver tissue. This enables appreciation of spatial heterogeneity of stiffness. Stiffness maps may reveal characteristic and differentiating features of chronic liver diseases and focal liver lesions and therefore provide useful information for clinical management. The objective of this pictorial review is to recapture the essentials of MRE technique and illustrate with examples, the utility of stiffness maps in other chronic liver disorders and focal liver lesions.
Keywords: Acute hepatitis; Amyloidosis; Congestive hepatopathy; Diffuse liver diseases; Elastograms; Focal liver lesions; Infiltrative diseases; Primary sclerosing cholangitis; Sarcoidosis.
Conflict of interest statement
Figures
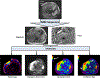
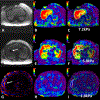
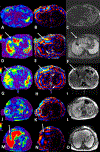
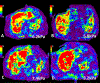






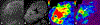


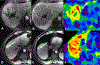
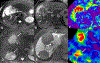
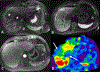
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

