Food insecurity among people with severe mental disorder in a rural Ethiopian setting: a comparative, population-based study
- PMID: 29143723
- PMCID: PMC6998966
- DOI: 10.1017/S2045796017000701
Food insecurity among people with severe mental disorder in a rural Ethiopian setting: a comparative, population-based study
Abstract
Aim: In low-income African countries, ensuring food security for all segments of the population is a high priority. Mental illness is associated consistently with poverty, but there is little evidence regarding the association with food insecurity. The aim of this study was to compare the levels of food insecurity in people with severe mental disorders (SMD) with the general population in a rural African setting with a high burden of food insecurity.
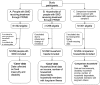
Method: Households of 292 community-ascertained people with a specialist-confirmed diagnosis of SMD (including schizophrenia and bipolar disorder) were compared with 284 households without a person with SMD in a rural district in south Ethiopia. At the time of the study, no mental health services were available within the district. Food insecurity was measured using a validated version of the Household Food Insecurity Access Scale. Disability was measured using the World Health Organisation Disability Assessment Schedule 2.0.
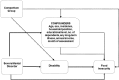
Result: Severe household food insecurity was reported by 32.5% of people with SMD and 15.9% of respondents from comparison households: adjusted odds ratio 2.82 (95% confidence interval 1.62 to 4.91). Higher annual income was associated independently with lower odds of severe food insecurity. When total disability scores were added into the model, the association between SMD and food insecurity became non-significant, indicating a possible mediating role of disability.
Conclusion: Efforts to alleviate food insecurity need to target people with SMD as a vulnerable group. Addressing the disabling effects of SMD would also be expected to reduce food insecurity. Access to mental health care integrated into primary care is being expanded in this district as part of the Programme for Improving Mental health carE (PRIME). The impact of treatment on disability and food insecurity will be evaluated.
Keywords: Disability; food insecurity; psychosis; severe mental disorder; sub-Saharan Africa.
Figures
Similar articles
-
Mental health problems and socioeconomic disadvantage: a controlled household study in rural Ethiopia.Int J Equity Health. 2019 Jul 31;18(1):121. doi: 10.1186/s12939-019-1020-4. Int J Equity Health. 2019. PMID: 31366362 Free PMC article.
-
Food insecurity and work impairment in people with severe mental disorders in a rural district of Ethiopia: a cross-sectional survey.Soc Psychiatry Psychiatr Epidemiol. 2019 Sep;54(9):1055-1066. doi: 10.1007/s00127-019-01709-7. Epub 2019 Apr 19. Soc Psychiatry Psychiatr Epidemiol. 2019. PMID: 31004179
-
Impact of integrated mental health care on food insecurity of households of people with severe mental illness in a rural African district: a community-based, controlled before-after study.Trop Med Int Health. 2020 Apr;25(4):414-423. doi: 10.1111/tmi.13370. Epub 2020 Feb 3. Trop Med Int Health. 2020. PMID: 31925844
-
Prevalence of food insecurity in people with major depression, bipolar disorder, and schizophrenia and related psychoses: A systematic review and meta-analysis.Crit Rev Food Sci Nutr. 2023;63(20):4485-4502. doi: 10.1080/10408398.2021.2002806. Epub 2021 Nov 16. Crit Rev Food Sci Nutr. 2023. PMID: 34783286
-
Food insecurity in adults with severe mental illness: A systematic review with meta-analysis.J Psychiatr Ment Health Nurs. 2024 Apr;31(2):133-151. doi: 10.1111/jpm.12969. Epub 2023 Aug 24. J Psychiatr Ment Health Nurs. 2024. PMID: 37621069
Cited by
-
The relationship between protective factors and common mental disorders among female urban slum dwellers in Ibadan, Nigeria.PLoS One. 2022 Feb 8;17(2):e0263703. doi: 10.1371/journal.pone.0263703. eCollection 2022. PLoS One. 2022. PMID: 35134096 Free PMC article.
-
Moving towards universal health coverage for mental disorders in Ethiopia.Int J Ment Health Syst. 2019 Feb 25;13:11. doi: 10.1186/s13033-019-0268-9. eCollection 2019. Int J Ment Health Syst. 2019. PMID: 30891082 Free PMC article.
-
Studying the context of psychoses to improve outcomes in Ethiopia (SCOPE): Protocol paper.PLoS One. 2024 May 9;19(5):e0293232. doi: 10.1371/journal.pone.0293232. eCollection 2024. PLoS One. 2024. PMID: 38722946 Free PMC article.
-
Measuring Disability Inclusion: Feasibility of Using Existing Multidimensional Poverty Data in South Africa.Int J Environ Res Public Health. 2021 Apr 22;18(9):4431. doi: 10.3390/ijerph18094431. Int J Environ Res Public Health. 2021. PMID: 33921932 Free PMC article.
-
Functional impairment among people with severe and enduring mental disorder in rural Ethiopia: a cross-sectional study.Soc Psychiatry Psychiatr Epidemiol. 2018 Aug;53(8):803-814. doi: 10.1007/s00127-018-1546-6. Epub 2018 Jun 14. Soc Psychiatry Psychiatr Epidemiol. 2018. PMID: 29947862
References
-
- Azevedo MH, Soares MJ, Coelho I, Dourado A, Valente J, Macedo A, Pato M, Pato C (1999). Using consensus OPCRIT diagnoses. An efficient procedure for best-estimate lifetime diagnoses. British Journal of Psychiatry 175, 154–157. - PubMed
-
- BasicNeeds (2008). Mental Health and Development: A Model in Practice. Leamington Spa: BasicNeeds.
-
- Coates J, Swindale A, Bilinsky P (2007). Household Food Insecurity Access Scale (HFIAS) for Measurement of Food Access: Indicator Guide. Food and Nutrition Technical Assistance (FANTA) project. United States Agency for International Development: Washington, DC.
-
- Cole S, Tembo G (2011). The effect of food insecurity on mental health: panel evidence from rural Zambia. Social Science and Medicine 73, 1071–1079. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical