Usual interstitial pneumonia: typical, possible, and "inconsistent" patterns
- PMID: 29160385
- PMCID: PMC5790657
- DOI: 10.1590/S1806-37562016000000368
Usual interstitial pneumonia: typical, possible, and "inconsistent" patterns
Abstract
Idiopathic pulmonary fibrosis is a severe and progressive chronic fibrosing interstitial lung disease, a definitive diagnosis being established by specific combinations of clinical, radiological, and pathological findings. According to current international guidelines, HRCT plays a key role in establishing a diagnosis of usual interstitial pneumonia (UIP). Current guidelines describe three UIP patterns based on HRCT findings: a typical UIP pattern; a pattern designated "possible UIP"; and a pattern designated "inconsistent with UIP", each pattern having important diagnostic implications. A typical UIP pattern on HRCT is highly accurate for the presence of histopathological UIP, being currently considered to be diagnostic of UIP. The remaining patterns require further diagnostic investigation. Other known causes of a UIP pattern include drug-induced interstitial lung disease, chronic hypersensitivity pneumonitis, occupational diseases (e.g., asbestosis), and connective tissue diseases, all of which should be included in the clinical differential diagnosis. Given the importance of CT studies in establishing a diagnosis and the possibility of interobserver variability, the objective of this pictorial essay was to illustrate all three UIP patterns on HRCT.
RESUMO: A fibrose pulmonar idiopática é uma pneumopatia intersticial fibrosante crônica de curso grave e progressivo, e seu diagnóstico se dá em combinações específicas de correlações clínicas e radiológicas, ou ainda patológicas. A TCAR tem papel chave no diagnóstico morfológico do padrão de pneumonia intersticial usual (PIU), segundo as recomendações internacionais vigentes. Os níveis de certeza para a leitura do padrão tomográfico foram inseridos em diretrizes atuais, descritos como padrão PIU típico, padrão PIU possível e padrão inconsistente com PIU, cada qual com importantes implicações na cadeia diagnóstica. A presença do padrão PIU típico tem alta concordância com o padrão PIU histopatológico, e, nessa situação, a TCAR é tida como suficiente para a determinação do padrão morfológico. Nos demais padrões, investigações diagnósticas complementares são indicadas. O diagnóstico diferencial com outras entidades, incluindo pneumopatias intersticiais por exposição medicamentosa, exposições extrínsecas (pneumonite de hipersensibilidade crônica), doenças ocupacionais (asbestose) e doenças do tecido conjuntivo, deve ser considerado clinicamente. Dada a importância da abordagem tomográfica, a qual pode apresentar relevantes discordâncias na avaliação interobservador, nosso objetivo foi ilustrar os padrões tomográficos de PIU neste ensaio pictórico.
Figures
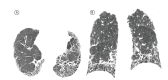







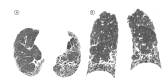



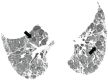


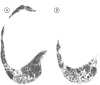
References
-
- 1 Raghu G, Collard HR, Egan JJ, Martinez FJ, Behr J, Brown KK, et al. An official ATS/ERS/JRS/ALAT statement: idiopathic pulmonary fibrosis: evidence-based guidelines for diagnosis and management. Am J Respir Crit Care Med. 2011;183(6):788-824. https://doi.org/10.1164/rccm.2009-040GL - DOI - PMC - PubMed
- Raghu G, Collard HR, Egan JJ, Martinez FJ, Behr J, Brown KK. An official ATS/ERS/JRS/ALAT statement idiopathic pulmonary fibrosis: evidence-based guidelines for diagnosis and management. Am J Respir Crit Care Med. 2011;183(6):788–824. https://doi.org/10.1164/rccm.2009-040GL - DOI - PMC - PubMed
-
- 2 Baddini-Martinez J, Baldi BG, Costa CH, Jezler S, Lima MS, Rufino R. Update on diagnosis and treatment of idiopathic pulmonary fibrosis. J Bras Pneumol. 2015;41(5):454-66. https://doi.org/10.1590/S1806-37132015000000152 - DOI - PMC - PubMed
- Baddini-Martinez J, Baldi BG, Costa CH, Jezler S, Lima MS, Rufino R. Update on diagnosis and treatment of idiopathic pulmonary fibrosis. J Bras Pneumol. 2015;41(5):454–466. https://doi.org/10.1590/S1806-37132015000000152 - DOI - PMC - PubMed
-
- 3 Raghu G, Rochwerg B, Zhang Y, Garcia CA, Azuma A, Behr J, et al. An Official ATS/ERS/JRS/ALAT Clinical Practice Guideline: Treatment of Idiopathic Pulmonary Fibrosis. An Update of the 2011 Clinical Practice Guideline. Am J Respir Crit Care Med. 2015;192(2):e3-19. https://doi.org/10.1164/rccm.201506-1063ST - DOI - PubMed
- Raghu G, Rochwerg B, Zhang Y, Garcia CA, Azuma A, Behr J. An Official ATS/ERS/JRS/ALAT Clinical Practice Guideline Treatment of Idiopathic Pulmonary Fibrosis. An Update of the 2011 Clinical Practice Guideline. Am J Respir Crit Care Med. 2015;192(2):e3–19. https://doi.org/10.1164/rccm.201506-1063ST - DOI - PubMed
-
- 4 Travis WD, Costabel U, Hansell DM, King Jr TE, Lynch DA, Nicholson AG, et al. An official American Thoracic Society/European Respiratory Society statement: Update of the international multidisciplinary classification of the idiopathic interstitial pneumonias. Am J Respir Crit Care Med. 2013;188(6),733-48. https://doi.org/10.1164/rccm.201308-1483ST - DOI - PMC - PubMed
- Travis WD, Costabel U, Hansell DM, King TE, Jr, Lynch DA, Nicholson AG, et al. An official American Thoracic Society/European Respiratory Society statement: Update of the international multidisciplinary classification of the idiopathic interstitial pneumonias. Am J Respir Crit Care Med. 2013;188(6):733–748. https://doi.org/10.1164/rccm.201308-1483ST - DOI - PMC - PubMed
-
- 5 Hodnett PA, Naidich DP. Fibrosing interstitial lung disease. A practical high-resolution computed tomography-based approach to diagnosis and management and a review of the literature. Am J Resp Crit Care Med. 2013;188(2):141-9. https://doi.org/10.1164/rccm.201208-1544CI - DOI - PubMed
- Hodnett PA, Naidich DP. Fibrosing interstitial lung disease A practical high-resolution computed tomography-based approach to diagnosis and management and a review of the literature. Am J Resp Crit Care Med. 2013;188(2):141–149. https://doi.org/10.1164/rccm.201208-1544CI - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

