Effectiveness of Laboratory Practices to Reducing Patient Misidentification Due to Specimen Labeling Errors at the Time of Specimen Collection in Healthcare Settings: LMBP™ Systematic Review
- PMID: 29181454
- PMCID: PMC5701285
- DOI: 10.1373/jalm.2017.023762
Effectiveness of Laboratory Practices to Reducing Patient Misidentification Due to Specimen Labeling Errors at the Time of Specimen Collection in Healthcare Settings: LMBP™ Systematic Review
Abstract
Background: Specimen labeling errors have long plagued the laboratory industry putting patients at risk of transfusion-related death, medication errors, misdiagnosis, and patient mismanagement. Many interventions have been implemented and deemed to be effective in reducing sample error rates. The objective of this review was to identify and evaluate the effectiveness of laboratory practices/ interventions to develop evidence based recommendations for the best laboratory practices to reduce labeling errors.
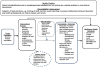
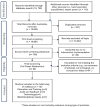
Content: The standardized LMBP™ A-6 methods were used to conduct this systematic review. Total evidence included 12 studies published during the time periods of 1980 to September 2015. Combined data from seven studies found that the interventions developed as a result of improved communication and collaboration between the laboratory and clinical staff resulted in substantial decrease in specimen labeling errors (Median relative percent change in labeling errors: -75.86; IQI: -84.77, -58.00). Further data from subset of four studies showed a significant decrease in specimen labeling errors after the institution of the standardized specimen labeling protocols (Median relative percent decrease in specimen labeling errors: -72.45; IQI: -83.25, -46.50).
Summary: Based on the evidence included in this review, the interventions that enhance the communication and collaboration between laboratory and healthcare professionals can decrease the specimen identification errors in healthcare settings. However, more research is needed to make the conclusion on the effectiveness of other evaluated practices in this review including training and education of the specimen collection staff, audit and feedback of labeling errors, and implementation of new technology (other than barcoding).
Figures




Similar articles
-
The future of Cochrane Neonatal.Early Hum Dev. 2020 Nov;150:105191. doi: 10.1016/j.earlhumdev.2020.105191. Epub 2020 Sep 12. Early Hum Dev. 2020. PMID: 33036834
-
Development and evaluation of a de-escalation training intervention in adult acute and forensic units: the EDITION systematic review and feasibility trial.Health Technol Assess. 2024 Jan;28(3):1-120. doi: 10.3310/FGGW6874. Health Technol Assess. 2024. PMID: 38343036 Free PMC article.
-
Quality Control Circle Practices to Reduce Specimen Rejection Rates.J Multidiscip Healthc. 2024 Oct 26;17:4925-4935. doi: 10.2147/JMDH.S486276. eCollection 2024. J Multidiscip Healthc. 2024. PMID: 39479378 Free PMC article.
-
A quality initiative to decrease pathology specimen-labeling errors using radiofrequency identification in a high-volume endoscopy center.Am J Gastroenterol. 2009 Apr;104(4):972-5. doi: 10.1038/ajg.2008.170. Epub 2009 Mar 3. Am J Gastroenterol. 2009. PMID: 19259073
-
Evidence Brief: Comparative Effectiveness of Appointment Recall Reminder Procedures for Follow-up Appointments [Internet].Washington (DC): Department of Veterans Affairs (US); 2015 Jul. Washington (DC): Department of Veterans Affairs (US); 2015 Jul. PMID: 27606388 Free Books & Documents. Review.
Cited by
-
Intervention efficacy for eliminating patient misidentification using step-by-step problem-solving procedures to improve patient safety.Nagoya J Med Sci. 2020 May;82(2):315-321. doi: 10.18999/nagjms.82.2.315. Nagoya J Med Sci. 2020. PMID: 32581410 Free PMC article.
-
Feasibility and acceptability of an iris biometric system for unique patient identification in routine HIV services in Kenya.Int J Med Inform. 2020 Jan;133:104006. doi: 10.1016/j.ijmedinf.2019.104006. Epub 2019 Oct 18. Int J Med Inform. 2020. PMID: 31706230 Free PMC article.
-
Assessment of the Use of Patient Vital Sign Data for Preventing Misidentification and Medical Errors.Healthcare (Basel). 2022 Dec 2;10(12):2440. doi: 10.3390/healthcare10122440. Healthcare (Basel). 2022. PMID: 36553964 Free PMC article.
-
Liability for embryo mix-ups in fertility practices in the USA.J Assist Reprod Genet. 2021 May;38(5):1101-1107. doi: 10.1007/s10815-021-02108-1. Epub 2021 Feb 18. J Assist Reprod Genet. 2021. PMID: 33598752 Free PMC article. Review.
References
-
- Ford Catching ID errors where it counts---in the lab. CAP Today. 2005;19(9):34–40.
-
- Sauer DMC, Boshkov L. Errors in transfusion medicine. Lab Med. 2001;4(32):205–7. 4(32):205-7. 2001;4(32):205-7.
-
- Jones BA, Calam RR, Howanitz PJ. Chemistry specimen acceptability: a College of American Pathologists Q-Probes study of 453 laboratories. Arch Pathol Lab Med. 1997;121(1):19–26. - PubMed
-
- Dale JC, Novis DA. Outpatient phlebotomy success and reasons for specimen rejection. Arch Pathol Lab Med. 2002;126(4):416–9. - PubMed
-
- Ford Disabling mislabeling---solutions for blood banks. CAP Today. 29(11):62–64. 2009;23(1):5-8.
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

