Quantifying attention shifts in augmented reality image-guided neurosurgery
- PMID: 29184663
- PMCID: PMC5683248
- DOI: 10.1049/htl.2017.0062
Quantifying attention shifts in augmented reality image-guided neurosurgery
Abstract
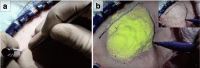
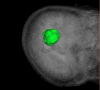
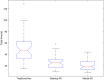
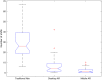
Image-guided surgery (IGS) has allowed for more minimally invasive procedures, leading to better patient outcomes, reduced risk of infection, less pain, shorter hospital stays and faster recoveries. One drawback that has emerged with IGS is that the surgeon must shift their attention from the patient to the monitor for guidance. Yet both cognitive and motor tasks are negatively affected with attention shifts. Augmented reality (AR), which merges the realworld surgical scene with preoperative virtual patient images and plans, has been proposed as a solution to this drawback. In this work, we studied the impact of two different types of AR IGS set-ups (mobile AR and desktop AR) and traditional navigation on attention shifts for the specific task of craniotomy planning. We found a significant difference in terms of the time taken to perform the task and attention shifts between traditional navigation, but no significant difference between the different AR set-ups. With mobile AR, however, users felt that the system was easier to use and that their performance was better. These results suggest that regardless of where the AR visualisation is shown to the surgeon, AR may reduce attention shifts, leading to more streamlined and focused procedures.
Keywords: augmented reality; augmented reality image-guided neurosurgery; craniotomy planning; desktop augmented reality; medical image processing; mobile augmented reality; neurophysiology; surgery; tumour; tumours.
Figures



References
-
- Kersten-Oertel M., Jannin P., Collins D.L.: ‘The state of the art of visualization in mixed reality image guided surgery’, Comput. Med. Imaging Graph., 2013, 37, (2), pp. 98–112 (doi: 10.1016/j.compmedimag.2013.01.009) - PubMed
-
- Kikinis R., Gleason P.L., Lorensen W.E., et al. : ‘Image guidance techniques for neurosurgery’. Visualization in Biomedical Computing 1994 Int. Society for Optics and Photonics, 1994, pp. 537–540
-
- Edwards P.J., King A.P., Maurer C.R., et al. : ‘Design and evaluation of a system for microscope-assisted guided interventions (magi)’, IEEE Trans. Med. Imaging, 2000, 19, (11), pp. 1082–1093 (doi: 10.1109/42.896784) - PubMed
-
- Cabrilo I., Bijlenga P., Schaller K.: ‘Augmented reality in the surgery of cerebral aneurysms: a technical report’, Oper. Neurosurg., 2011, 10, (2), pp. 252–261 - PubMed
-
- Cabrilo I., Bijlenga P., Schaller K.: ‘Augmented reality in the surgery of cerebral arteriovenous malformations: technique assessment and considerations’, Acta Neurochir., 2014, 156, (9), pp. 1769–1774 (doi: 10.1007/s00701-014-2183-9) - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

